The heart is one of the most resilient organs in the human body, quietly adapting to the demands placed on it every single day. Yet when it begins to strain under pressure, it often sends out subtle distress signals long before a serious event occurs. Recognizing these early warning signs can make a significant difference in long-term cardiovascular health. The following list covers 25 signs that medical experts associate with a heart that may be under excessive stress.
Shortness of Breath

Feeling breathless during activities that once felt effortless is a recognized indicator that the heart may not be pumping blood efficiently. When the heart struggles, fluid can back up into the lungs and restrict normal airflow. This symptom is particularly notable when it occurs while lying flat or during minimal physical exertion. Doctors often treat unexplained breathlessness as one of the earliest red flags of cardiovascular strain. It is frequently reported by individuals later diagnosed with heart failure or coronary artery disease.
Chest Tightness

A persistent sensation of pressure or squeezing in the chest is among the most widely recognized signs of cardiac stress. This feeling may come and go throughout the day and does not always present with sharp pain. It can be triggered by physical activity, emotional stress, or even cold temperatures. Medical professionals note that chest tightness lasting more than a few minutes warrants immediate evaluation. It is commonly associated with reduced blood flow to the heart muscle itself.
Fatigue

Unusual and persistent tiredness that is not explained by poor sleep or physical exertion is frequently linked to a struggling heart. When the heart pumps less effectively, the body diverts blood away from non-essential functions to protect vital organs. This redistribution leaves muscles and the brain with less oxygen, producing a deep and chronic sense of exhaustion. Many patients describe this fatigue as fundamentally different from ordinary tiredness. It is one of the most commonly overlooked early symptoms of cardiovascular disease, particularly in women.
Heart Palpitations
An awareness of the heartbeat as fluttering, racing, or pounding when at rest is a symptom the cardiovascular system uses to communicate imbalance. Palpitations can result from irregular electrical signals within the heart that disrupt its normal rhythm. While occasional palpitations are often harmless, frequent episodes may indicate arrhythmia or other underlying conditions. They are sometimes accompanied by dizziness or a brief sense of faintness. Cardiologists recommend tracking the frequency and duration of these episodes to aid diagnosis.
Swollen Ankles

Edema in the lower legs and ankles occurs when the heart lacks the pumping force needed to return fluid from the extremities back to circulation. This swelling tends to worsen throughout the day and improves after lying down overnight. It is a classic sign of right-sided heart strain or congestive heart failure. The swelling may also extend to the feet or lower legs as the condition progresses. Salt intake and prolonged sitting can amplify this symptom in individuals with underlying cardiac vulnerability.
Dizziness

Frequent lightheadedness or sudden episodes of dizziness can indicate that the brain is not receiving a consistent supply of oxygenated blood. The heart plays a central role in maintaining steady cerebral blood flow, and any disruption can trigger this symptom. Dizziness associated with standing up quickly is sometimes a sign of low blood pressure linked to reduced cardiac output. When it occurs alongside chest discomfort or palpitations, it becomes a more urgent concern. Neurological and cardiological evaluations are typically conducted together to rule out various causes.
Irregular Heartbeat

A heartbeat that feels uneven, skipping beats, or running in unpredictable patterns may reflect an arrhythmia placing added strain on the cardiac muscle. The heart works harder when its electrical coordination is disrupted because it compensates to maintain output. Atrial fibrillation is among the most common arrhythmias and significantly increases the workload on the heart over time. It also raises the risk of blood clots forming within the heart chambers. Early detection and management are critical to preventing more serious cardiovascular complications.
Jaw Pain

Discomfort in the jaw, particularly on the left side, is a lesser-known but medically significant symptom of cardiac stress. Pain radiating from the heart can travel along nerve pathways that share connections with the jaw, neck, and shoulder. This referred pain pattern is more commonly reported during cardiac events in women than in men. It may appear without any accompanying chest discomfort, making it easy to misattribute to dental problems. Emergency medical personnel are trained to consider jaw pain as a potential cardiac symptom during assessment.
Night Sweats

Waking up drenched in perspiration without an obvious environmental cause can be a sign that the heart and autonomic nervous system are under strain. The body sometimes activates its sweat response when cardiac output drops and the fight-or-flight system compensates. Night sweats linked to heart stress are typically more intense than those associated with hormonal changes and may be accompanied by anxiety or rapid breathing. They can also occur as a side effect of heart infections such as endocarditis. A pattern of recurring night sweats with other cardiac symptoms warrants a thorough medical review.
Rapid Weight Gain

Gaining several pounds within a very short period, particularly around the abdomen and lower limbs, can signal that the heart is failing to manage fluid levels properly. This type of weight gain is not related to caloric intake but rather to fluid retention driven by inadequate cardiac circulation. A gain of more than two to three pounds within a single day is a benchmark commonly used by cardiologists to monitor heart failure progression. Patients with known cardiovascular conditions are often advised to weigh themselves daily for this reason. Prompt reporting of sudden weight changes to a physician can help prevent hospitalization.
Nausea

Persistent or recurring nausea that has no gastrointestinal explanation can sometimes be traced to reduced blood flow to the digestive system caused by a strained heart. The heart supplies blood to organs throughout the body, and when its output drops, the gut is among the first areas to experience reduced perfusion. This can produce feelings of queasiness, loss of appetite, and general digestive discomfort. During acute cardiac events, nausea is frequently reported alongside sweating and chest pressure. It is a symptom that tends to be underestimated when it appears in isolation from more obvious cardiac signs.
Arm Pain

Pain or heaviness extending down the left arm is one of the most recognized symptoms associated with cardiac distress, particularly during a heart attack. This sensation arises because the nerves supplying the heart share pathways with those leading to the arm. The discomfort may feel like a dull ache, numbness, or a tingling sensation rather than sharp pain. It often begins in the shoulder and travels toward the wrist or fingers. Right arm involvement is less common but has also been documented in cardiac events.
Back Pain

Unexplained upper or middle back pain, especially between the shoulder blades, can be a referred symptom of cardiac stress. The diaphragm and the nerves surrounding the heart connect to areas of the back through shared spinal pathways. This type of pain is more frequently reported by women experiencing heart attacks than by men. It tends to be described as a deep, persistent aching rather than a sharp or muscular sensation. Back pain in combination with shortness of breath or sweating should prompt an urgent cardiac evaluation.
Persistent Cough

A chronic cough that produces a white or pinkish frothy mucus is a notable sign that fluid may be accumulating in the lungs due to poor cardiac function. This occurs when a weakened left side of the heart cannot adequately drain blood from the pulmonary circulation. The resulting fluid buildup irritates the airways and triggers the coughing reflex as the body attempts to clear the lungs. Many people with heart failure describe this cough as relentless and worsening when lying down. It is a symptom that is sometimes mistaken for a respiratory condition before its cardiac origin is identified.
Brain Fog

Difficulty concentrating, memory lapses, and a general sense of cognitive sluggishness can be neurological signs that the brain is receiving insufficient blood flow due to reduced cardiac output. The brain is highly dependent on a continuous and well-oxygenated blood supply, and even mild disruptions can affect cognitive clarity. Patients with heart failure frequently report feeling mentally slower or less sharp than usual. This symptom can affect work performance and daily functioning before it is connected to cardiovascular causes. Researchers have identified a significant overlap between heart failure severity and measurable cognitive decline.
Cold Extremities

Hands and feet that remain persistently cold even in warm conditions may indicate that the heart is prioritizing blood flow to core vital organs at the expense of the peripheral circulation. This is a common compensatory response when cardiac output is diminished. Coldness in the extremities can also reflect arterial narrowing that reduces blood flow to the limbs. When combined with color changes such as pallor or a bluish tint to the fingertips, it becomes a more urgent clinical sign. Peripheral artery disease and congestive heart failure are both conditions associated with this pattern.
Sleep Apnea

Disrupted breathing during sleep that causes repeated awakenings forces the heart to work harder each time oxygen levels drop in the bloodstream. The resulting spikes in blood pressure and heart rate strain the cardiovascular system night after night. Sleep apnea is strongly associated with an increased risk of hypertension, arrhythmia, and heart failure when left untreated. The cyclical oxygen deprivation caused by apnea events places a measurable and recurring burden on cardiac tissue. Treatment with continuous positive airway pressure therapy has been shown to reduce cardiovascular stress associated with this condition.
High Resting Heart Rate
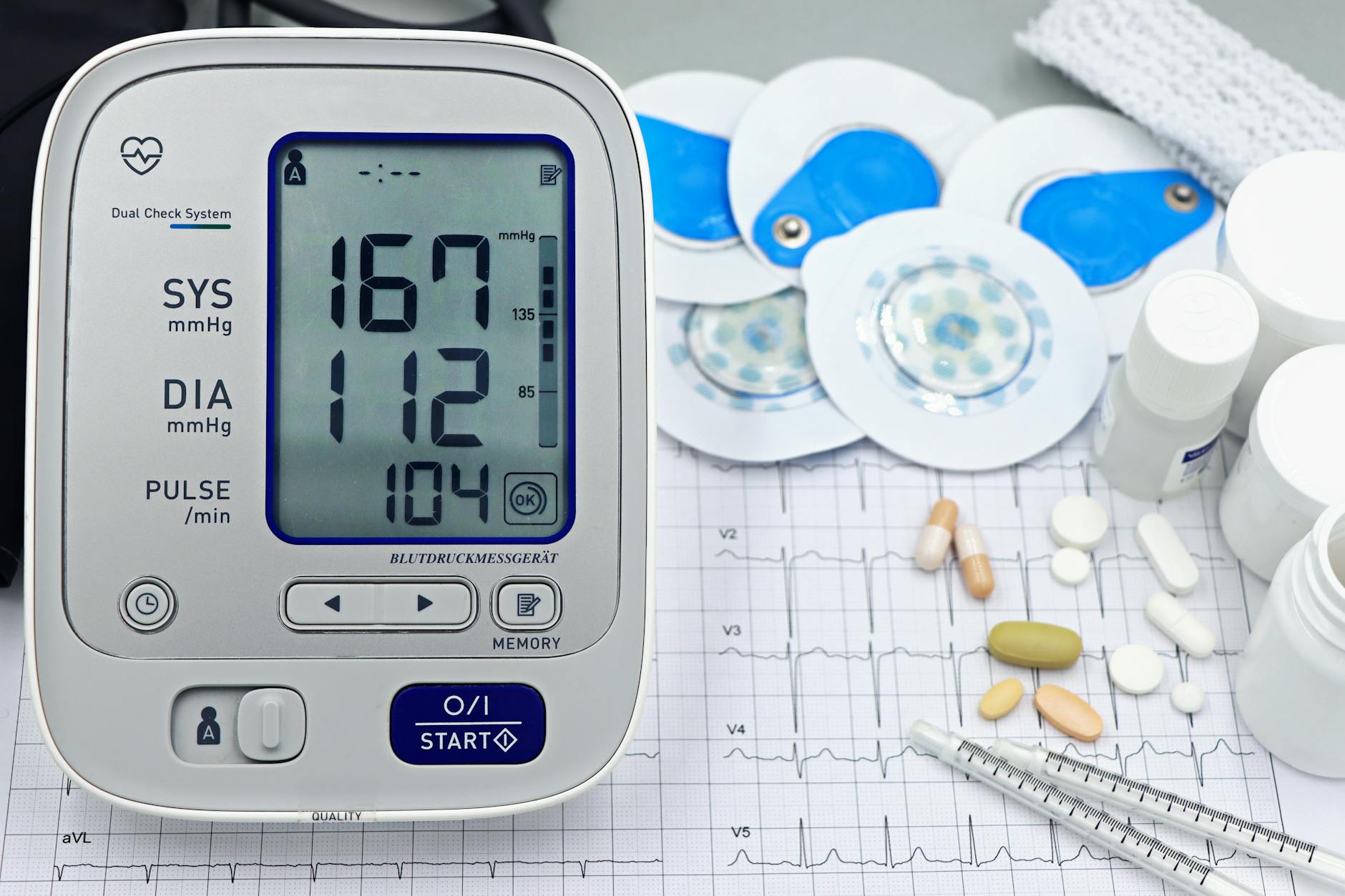
A resting heart rate consistently above 100 beats per minute places a greater cumulative demand on the cardiac muscle over the course of each day. The heart must contract more frequently to maintain adequate circulation, which accelerates wear over time. Tachycardia at rest can result from anemia, dehydration, thyroid disorders, or underlying heart disease. Even within the normal range, research suggests that a resting heart rate trending toward the higher end is associated with elevated cardiovascular risk. Tracking resting heart rate over time provides useful insight into overall cardiac efficiency.
Reduced Exercise Tolerance

Finding that physical activities requiring previously manageable effort now trigger exhaustion or discomfort is a practical indicator of declining cardiovascular capacity. The heart’s ability to increase its output in response to exercise is a key measure of overall cardiac health. A noticeable and progressive reduction in exercise tolerance without an apparent musculoskeletal cause should prompt cardiovascular investigation. This symptom is often gradual in onset, which means many individuals adjust their activity levels without recognizing the underlying reason. Cardiologists use exercise stress tests to formally evaluate how well the heart responds to increased physical demand.
Anxiety

Unexplained feelings of anxiety, dread, or a sense that something is wrong can sometimes originate from physiological changes occurring within the cardiovascular system. When the heart rate is irregular or cardiac output is dropping, the autonomic nervous system triggers a stress response that can manifest as psychological unease. Some individuals report a sudden and intense feeling of impending doom as one of the first noticeable signs of a cardiac event. The relationship between anxiety and heart health is bidirectional, with each capable of exacerbating the other. Distinguishing cardiac-driven anxiety from psychological anxiety requires clinical evaluation.
Pale Skin

A noticeable pallor or grayish skin tone that develops gradually or appears suddenly can indicate that blood is not being distributed efficiently to the body’s surface tissues. The skin color often reflects the underlying state of peripheral circulation, which is directly influenced by cardiac output. During periods of acute cardiac stress, blood is redirected inward, leaving the skin appearing unusually pale or ashen. This sign is more easily detected in lighter skin tones but can also be observed in the lips, gums, and inner eyelids in individuals with darker complexions. Sudden paleness alongside other symptoms is treated as a medical emergency.
Frequent Urination at Night

Waking multiple times during the night to urinate can be linked to the body’s redistribution of fluid that pooled in the legs during the day. When a person lies down, gravity no longer keeps excess fluid in the lower limbs, and the kidneys begin processing it. This increased nocturnal fluid load forces the kidneys to produce more urine throughout the night. While nocturia has many causes, its presence alongside swollen ankles and fatigue forms a recognizable pattern associated with heart strain. Cardiologists consider it a useful indirect marker of fluid management dysfunction in cardiac patients.
Vision Changes

Episodes of blurred vision, visual disturbances, or temporary loss of sight can reflect fluctuations in blood pressure or inadequate cerebral blood flow related to cardiac inefficiency. The small blood vessels supplying the eyes and brain are sensitive indicators of overall vascular health. Hypertension caused by a heart working under chronic excess load can damage retinal vessels over time. Transient visual disturbances may precede a stroke in individuals with unmanaged cardiovascular disease. Regular eye examinations can sometimes reveal vascular changes that prompt further cardiac investigation.
Loss of Appetite

A diminished desire to eat, particularly when persistent and unexplained, can be a symptom of heart strain rather than a digestive issue. When the heart struggles to maintain adequate circulation, blood flow to the gastrointestinal tract decreases, which can suppress hunger signals and cause discomfort after eating. Patients with advanced heart failure frequently experience significant unintentional weight loss as a result of this reduced appetite. The stomach and intestines may also feel fuller than usual if abdominal fluid accumulation is present. Nutritional decline in cardiac patients is taken seriously by clinicians because it can accelerate disease progression.
Vein Visibility
Prominently visible veins in the neck, particularly the jugular veins, can indicate elevated venous pressure resulting from a heart that is not pumping efficiently. When the right side of the heart struggles to process returning blood, pressure builds up in the venous system and causes veins to distend. This sign is typically assessed with the patient reclined at a slight angle and is a standard part of cardiovascular physical examination. Distension in the jugular veins at rest and without exercise is considered a clinical sign of congestive heart failure. It is one of the physical findings that physicians look for when evaluating patients with suspected cardiac overload.
Heart health is a topic that affects everyone regardless of age or fitness level, so share your thoughts or personal experiences in the comments.