Living with a chronic illness is an invisible and often exhausting daily reality that millions of people navigate without the understanding they deserve. The words people choose in these conversations carry enormous weight and can either foster genuine connection or cause lasting emotional harm. Well-meaning friends, family members, and colleagues frequently reach for phrases that feel reassuring but land as dismissive or hurtful. Understanding what not to say is one of the most meaningful ways to show up for someone managing a long-term condition.
“But You Don’t Look Sick”

Many chronic illnesses are invisible and do not present with outward physical signs that others can easily observe. Saying this to someone invalidates their lived experience and implies that suffering must be visible to be real. Conditions such as lupus, fibromyalgia, and Crohn’s disease can cause debilitating symptoms without changing a person’s outward appearance. This phrase often causes people to feel pressured to perform visible signs of illness just to be believed.
“Have You Tried Yoga?”

Offering unsolicited wellness advice to someone with a chronic illness suggests that they have not already explored every possible option to feel better. Most people living with long-term conditions have spent considerable time and resources working closely with medical professionals to manage their health. Suggesting a single lifestyle habit as a potential cure minimises the complexity of their condition and the seriousness of their treatment plan. It can also imply that their illness is somehow a result of not trying hard enough to get well.
“Everything Happens for a Reason”
This phrase attempts to assign spiritual or philosophical meaning to a person’s suffering without their invitation to do so. For someone managing a chronic condition, it can feel deeply dismissive and suggest that their pain serves some greater purpose they should simply accept. It shifts focus away from the very real and practical challenges they face every day. Empathy and presence are far more comforting than abstract reassurances in these moments.
“You Just Need to Think More Positively”
Implying that a person’s mindset is responsible for their physical condition is a form of victim-blaming that places undue burden on the individual. Chronic illness is rooted in complex physiological processes that cannot be resolved through attitude adjustment alone. While emotional wellbeing does play a role in overall health, it does not override the biological realities of serious medical conditions. This phrase can leave people feeling guilty for their own suffering, which adds unnecessary psychological distress to their existing challenges.
“I Know How You Feel”

Unless a person has lived with the exact same condition, claiming to fully understand another person’s experience is inaccurate and minimising. Chronic illness is deeply personal and varies enormously between individuals even when they share the same diagnosis. Saying this can shut down authentic conversation and make the person feel unseen rather than supported. A more meaningful response is to acknowledge that you cannot fully understand but that you are there to listen.
“At Least It’s Not Cancer”

Comparing one illness to another in order to suggest someone should feel grateful for their condition is never a helpful response. Every chronic illness carries its own set of challenges, limitations, and emotional weight that cannot be ranked against other diagnoses. This phrase communicates that the person’s suffering is less valid or less worthy of compassion than someone else’s. It discourages people from openly discussing their struggles for fear of being judged as dramatic or ungrateful.
“You Were Fine Yesterday”
Chronic illnesses are characterised by fluctuating symptoms that can change dramatically from one day to the next, and sometimes from one hour to the next. Pointing out that someone appeared well previously suggests that their current symptoms are exaggerated or inconsistent with their diagnosis. This misunderstanding of how chronic conditions work creates an environment where people feel they must justify their bad days. Recognising that variability is a core feature of many chronic illnesses is essential to offering genuine support.
“My Aunt Had That and She Got Better”

Sharing anecdotes about other people who recovered from a similar condition implies that the person you are speaking to should also be getting better. Chronic illness, by definition, is long-term and often without a clear path to full recovery for many individuals. Each person’s medical situation is unique and is shaped by a wide range of biological, environmental, and personal factors. Anecdotal comparisons can create false hope or make someone feel as though they are failing to recover in the way they should.
“You’re Too Young to Be This Sick”

Chronic illness does not discriminate by age, and millions of children, teenagers, and young adults live with serious long-term health conditions every day. Saying this to someone implies that their age makes their diagnosis surprising or somehow less legitimate. It can also reinforce internal struggles that younger people with chronic illness already face around identity, independence, and being taken seriously by others. Acknowledging that illness affects people at every stage of life is a critical part of removing stigma.
“Just Push Through It”

Advising someone with a chronic illness to ignore their symptoms and push forward can lead to serious physical consequences including flares, injury, and long-term setbacks. Pacing and energy management are medically recognised strategies that many people with chronic conditions rely on to function safely. What looks like a lack of effort or willpower from the outside is often a carefully managed approach to preserving health. This phrase reinforces the damaging idea that rest and self-care are signs of weakness rather than medical necessity.
“Have You Tried Cutting Out Gluten?”

Dietary advice offered without medical context or understanding of a person’s specific condition is rarely helpful and often frustrating to receive. People with chronic illnesses typically work with dietitians and physicians to develop nutrition plans that are safe and appropriate for their individual needs. Suggesting a trendy dietary change implies that a simple food swap could solve a complex medical problem. It also trivialises the significant effort people already invest in managing their health through every available means.
“You Should Get More Sleep”

While sleep is important for general health, telling someone with a chronic illness to simply sleep more overlooks the fact that many conditions directly interfere with sleep quality and duration. Conditions such as chronic pain, autoimmune disorders, and neurological diseases frequently cause insomnia, disrupted sleep, and fatigue that is not resolved by more rest. This advice treats the symptom as a lifestyle choice rather than a physiological consequence of the illness itself. It also implies that the person is not already doing everything they can to care for their body.
“It Could Always Be Worse”

Reminding someone that their situation could be more severe does nothing to reduce the very real difficulties they are currently experiencing. Comparative suffering is not a useful framework for supporting someone who is dealing with ongoing health challenges. This phrase can cause people to suppress their feelings and feel ashamed of struggling when others have it harder. Validating a person’s experience exactly as it is represents a far more compassionate and constructive approach.
“You Don’t Seem That Sick to Me”

Personal observation is not a diagnostic tool, and this phrase communicates a fundamental misunderstanding of how chronic illness functions. People with long-term conditions often expend tremendous energy to appear functional and composed in social situations, which masks the true extent of their symptoms. Questioning the validity of someone’s illness based on how they appear in a single interaction can cause deep emotional harm. It discourages people from being honest about how they are truly feeling for fear of disbelief.
“Have You Seen a Doctor About That?”

Someone managing a chronic illness has almost certainly been engaged with the medical system for an extended period and does not need a reminder to seek professional help. This question can feel condescending and suggests a lack of trust in the person’s ability to manage their own healthcare. It also minimises the often long and complicated medical journey that led them to their current point. A better approach is to ask how their care is going rather than implying that medical attention might be something they have overlooked.
“Maybe It’s Stress”

While stress can exacerbate many conditions, attributing a chronic illness primarily to stress suggests that it is psychological in origin rather than physiological. This is a particularly harmful framing because it has historically been used to dismiss patients, especially women, from receiving proper medical investigation and treatment. Chronic illness involves real and measurable changes in the body that exist independently of a person’s stress levels. Reducing a diagnosis to an emotional cause denies the legitimacy of the condition entirely.
“I Wish I Could Stay Home All Day”
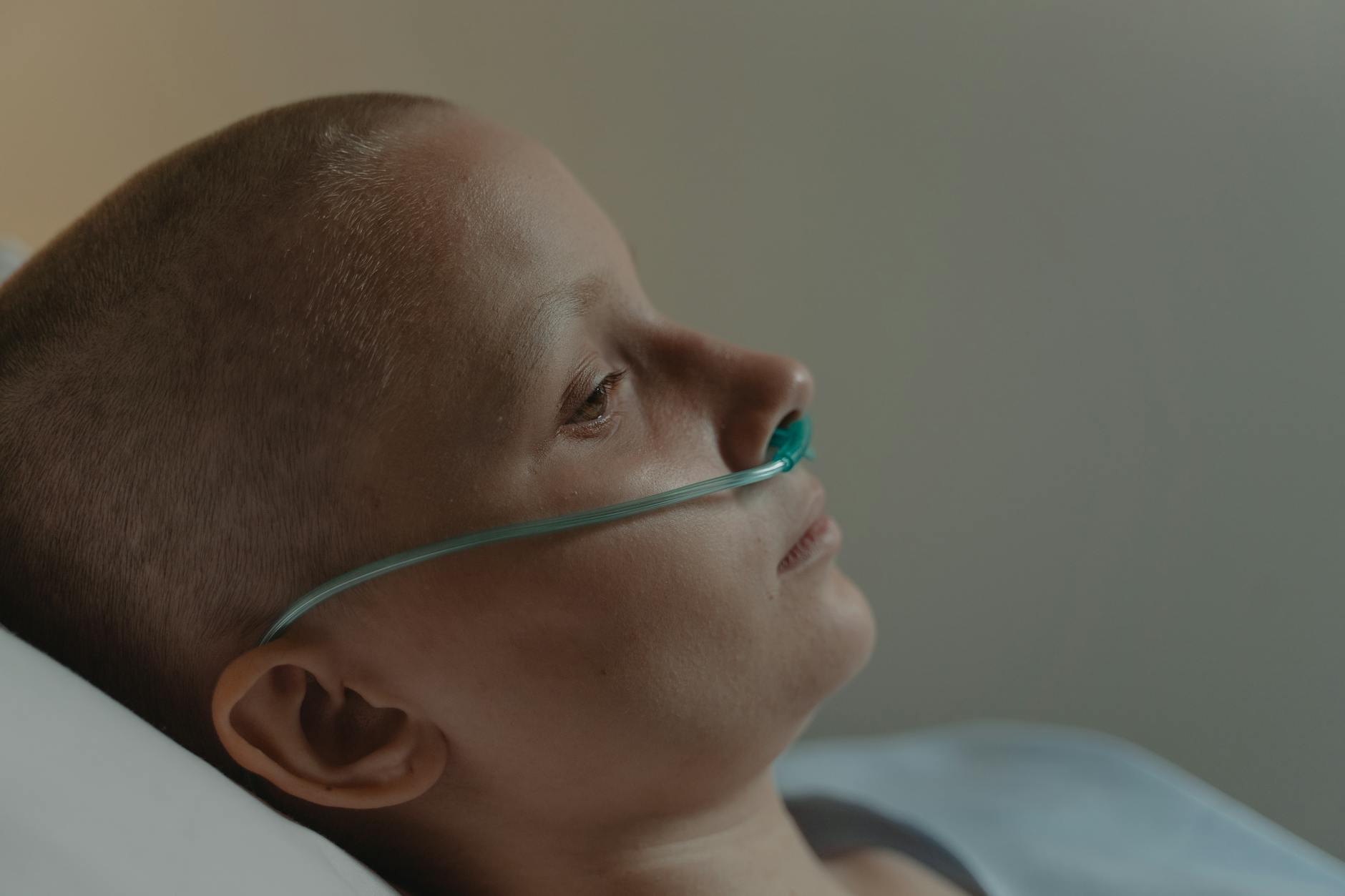
This comment trivialises the profound loss of independence, career opportunity, and social connection that can accompany a chronic illness that limits mobility or energy. Staying home due to illness is not a form of leisure and is often accompanied by significant physical discomfort, isolation, and financial stress. For many people, the inability to participate in work and social life is one of the most painful aspects of living with a long-term condition. Framing it as enviable is both inaccurate and deeply insensitive to their daily reality.
“Are You Sure It’s Not All in Your Head?”

This question directly challenges the validity of a person’s symptoms and implies that their experience is a product of their imagination or mental instability. It echoes a long history of medical gaslighting that has caused lasting harm to people with chronic conditions who have struggled to receive accurate diagnoses. Even conditions that involve the nervous system or have a psychological component are real, diagnosable, and worthy of serious medical treatment. Asking this question can cause someone to internalise doubt about their own health, which makes it harder for them to advocate for themselves.
“You’re Always Sick”

Pointing out the frequency of someone’s illness with a tone of exasperation adds social pressure to an experience that is already deeply difficult to manage. People with chronic conditions do not choose to be unwell and are not using their illness for attention or as an excuse to avoid responsibility. This phrase can make someone feel like a burden to the people around them, which is an emotionally harmful perception that is unfortunately already common among those with long-term illness. Consistent empathy regardless of how often symptoms arise is what genuine support looks like.
“Have You Tried Essential Oils?”

Recommending alternative wellness products to someone managing a medically complex condition is unlikely to be helpful and can come across as dismissive of their serious health needs. People with chronic illnesses often live at the intersection of significant medical expenses, treatment side effects, and ongoing symptom management, making this kind of suggestion feel tone-deaf. It implies that a simple consumer product could accomplish what years of medical care have not, which minimises the gravity of their situation. Respecting the treatment journey a person is already on is a more supportive way to engage.
“I Forget You’re Sick Because You Seem So Normal”

Framing normalcy as a compliment in the context of chronic illness reinforces the idea that being sick makes a person abnormal or lesser than others. This comment, while often intended kindly, erases the significant invisible effort a person puts into managing their condition while participating in everyday life. It can also make someone feel unseen in their struggles by suggesting that their illness is not visible enough to warrant ongoing acknowledgement. Recognising someone fully, including both their resilience and their challenges, is a more complete and respectful form of recognition.
“You Need to Exercise More”

Exercise recommendations directed at someone with a chronic illness ignore the fact that physical activity can be contraindicated, dangerous, or deeply difficult for many conditions. Disorders affecting joints, muscles, the cardiovascular system, or energy metabolism may make conventional exercise harmful rather than beneficial without careful medical guidance. Many people with chronic conditions do engage in modified or therapeutic movement as part of their treatment plans, often at great effort. Assuming that more exercise is simply a matter of motivation misunderstands the physical realities of life with a long-term condition.
“At Least You Have a Diagnosis”

While receiving a diagnosis is an important milestone, it does not resolve the symptoms, the grief, or the ongoing challenges of living with a chronic condition. A diagnosis is the beginning of a medical journey rather than its resolution, and many people experience complex and conflicting emotions upon receiving one. This phrase dismisses the emotional weight of learning that a condition is long-term or without a cure. Validating the full range of feelings that come with a diagnosis is far more supportive than suggesting that having a name for the illness is sufficient comfort.
“You Should Try Intermittent Fasting”

Nutritional trends popularised in wellness culture are not medically appropriate for everyone, and suggesting them to someone with a chronic illness can be genuinely harmful. Many conditions and their associated medications require regular food intake, specific dietary compositions, or careful caloric management that makes fasting dangerous. This advice signals a lack of awareness of the medical complexity involved in managing a long-term condition and the role that nutrition plays within that framework. It also positions the person as a target for generic health advice rather than as someone navigating a specific and serious medical reality.
“You’ve Been Sick for So Long, Have You Tried a Second Opinion?”

Implying that a person’s ongoing illness is the result of misdiagnosis or poor medical choices undermines their confidence in the care they have already received. Most people with chronic illnesses have consulted multiple specialists and have often been through a lengthy and emotionally exhausting diagnostic process before arriving at their current treatment. This phrase can introduce unnecessary doubt and anxiety while failing to offer anything practically useful. Trusting that the person is already engaging thoughtfully with their healthcare is a more respectful baseline assumption.
“My Friend Cured Herself by Going Vegan”

Anecdotal stories about other people’s recoveries through lifestyle choices place implicit pressure on the person with a chronic illness to attempt the same approach. Chronic conditions are medically complex and the experiences of one individual are not transferable to another, even with a shared diagnosis. Sharing these stories in response to someone’s health struggles can feel dismissive of the legitimate medical management they are already undertaking. It also risks directing someone away from evidence-based treatment toward approaches that may be unhelpful or even unsafe for their specific condition.
“You Look Better Than You Did Last Time”

Commenting on how someone appears in relation to their illness makes their physical presentation the primary measure of how they are actually doing. A person can look well while still experiencing significant internal symptoms, pain, fatigue, or emotional distress related to their condition. This kind of observation can pressure people to perform wellness in social settings even on their worst days. Asking how someone is feeling rather than commenting on how they look opens a more authentic and supportive conversation.
“Just Be Grateful for What You Have”

Gratitude is a meaningful practice, but directing it at someone in the midst of managing a chronic illness as a way to redirect their focus away from their struggles is unhelpful. Expressing frustration, grief, or exhaustion about living with a long-term condition is a valid and necessary part of processing that experience. Telling someone to focus on gratitude implies that their negative emotions are inappropriate or excessive given their circumstances. Allowing space for the full emotional reality of chronic illness is far more compassionate than offering redirections toward positivity.
“You Should Try Cold Water Therapy”

Wellness trends that receive significant media attention are frequently offered to people with chronic illness as though they represent universal health solutions. Cold water exposure can be medically contraindicated for a wide range of conditions including cardiovascular disorders, Raynaud’s syndrome, and certain autoimmune diseases. Suggesting it without knowledge of someone’s medical history demonstrates a lack of awareness of how these trends interact with complex health conditions. People managing chronic illness deserve conversations rooted in respect for their medical expertise about their own bodies rather than recommendations borrowed from mainstream wellness culture.
Share your thoughts and experiences in the comments and let others in the community know what phrases have felt most unhelpful during your own health journey.