Patients routinely withhold information from their doctors out of embarrassment, fear of judgment, or the assumption that certain details are irrelevant. This habit can lead to missed diagnoses, incorrect treatment plans, and preventable health complications. Doctors are trained to handle sensitive information without judgment, and full transparency is the foundation of effective medical care. Every detail shared during a checkup gives a clearer picture of overall health and enables more accurate, personalized guidance. The following list covers the most commonly hidden health matters that doctors genuinely need to know.
Alcohol Consumption

Many patients underreport how much alcohol they drink each week, often citing embarrassment or fear of being lectured. Alcohol affects liver function, medication metabolism, blood pressure, and mental health in ways that directly influence medical decisions. Doctors use this information to screen for dependency, adjust prescriptions, and identify risks before they become serious conditions. Being accurate about intake allows for honest conversations about safe limits and relevant health screenings.
Sleep Patterns

Poor or irregular sleep is frequently dismissed as unimportant during medical appointments. Sleep quality and duration are directly connected to heart health, immune function, weight management, and cognitive performance. Conditions like sleep apnea often go undiagnosed for years simply because patients never mention snoring, gasping, or chronic fatigue. Sharing detailed information about nighttime habits helps doctors determine whether a sleep study or further investigation is warranted.
Recreational Drug Use

Patients often avoid disclosing recreational drug use due to concerns about legal judgment or social stigma. Medical professionals require this information to prevent dangerous drug interactions and to accurately interpret certain lab results and vital sign readings. Some substances significantly affect heart rate, blood pressure, and liver enzymes in ways that can mimic or mask other conditions. Disclosure is protected under medical confidentiality and is never used for law enforcement purposes.
Sexual Health Concerns

Topics related to sexual health are among the most commonly avoided during routine checkups despite being medically significant. Symptoms such as pain during intercourse, changes in libido, erectile dysfunction, or unusual discharge can signal hormonal imbalances, infections, or cardiovascular issues. Sexually transmitted infections often present without obvious symptoms and require specific testing that doctors will not order without relevant context. Open conversation in this area allows for appropriate screenings and treatment that protect both individual and partner health.
Mental Health Struggles

Feelings of anxiety, depression, persistent sadness, or emotional numbness are frequently kept private during physical health appointments. Mental health is deeply connected to physical wellbeing and influences everything from immune response to chronic pain perception and cardiovascular risk. Many patients fear a mental health label on their medical records or worry about being prescribed medication unnecessarily. Sharing these experiences allows doctors to offer referrals, monitor for physical contributors, and ensure a complete picture of overall wellness.
Dietary Habits

Patients often present an idealized version of their diet during checkups, mentioning salads while omitting fast food, excess sugar, or restrictive eating patterns. Nutritional habits directly affect cholesterol, blood sugar, inflammation, and gut health in clinically meaningful ways. Doctors rely on dietary information to contextualize lab results and to recommend targeted interventions or referrals to dietitians. An accurate account of eating patterns, including binge eating or skipping meals, helps identify risks for metabolic and gastrointestinal conditions.
Supplement and Herbal Remedy Use

A large number of people take vitamins, herbal supplements, or alternative remedies without mentioning them to their doctors. Many supplements interact with prescription medications, alter hormone levels, or affect blood clotting and organ function in significant ways. St. John’s Wort, for example, is known to reduce the effectiveness of several widely prescribed medications including antidepressants and birth control. Providing a full list of everything consumed daily, whether purchased at a pharmacy or a health food store, is essential for safe prescribing.
Smoking History

Some patients downplay their smoking history or fail to mention that they previously smoked, believing it no longer matters after quitting. A history of tobacco use remains relevant for decades and informs decisions around cancer screenings, lung function tests, and cardiovascular risk assessments. Current smokers who cut back often report quitting entirely, which affects the accuracy of risk stratification tools doctors rely on. Complete honesty about past and present tobacco use, including vaping and chewing tobacco, enables more targeted preventive care.
Financial Stress

The connection between financial hardship and physical health is well documented and clinically relevant. Chronic financial stress is linked to elevated cortisol levels, hypertension, poor sleep, and weakened immune response. Doctors who are aware of a patient’s financial situation can recommend generic medications, connect them with assistance programs, and avoid ordering tests that create unmanageable costs. This information also helps providers understand barriers to treatment adherence and lifestyle recommendations.
Bowel and Digestive Changes
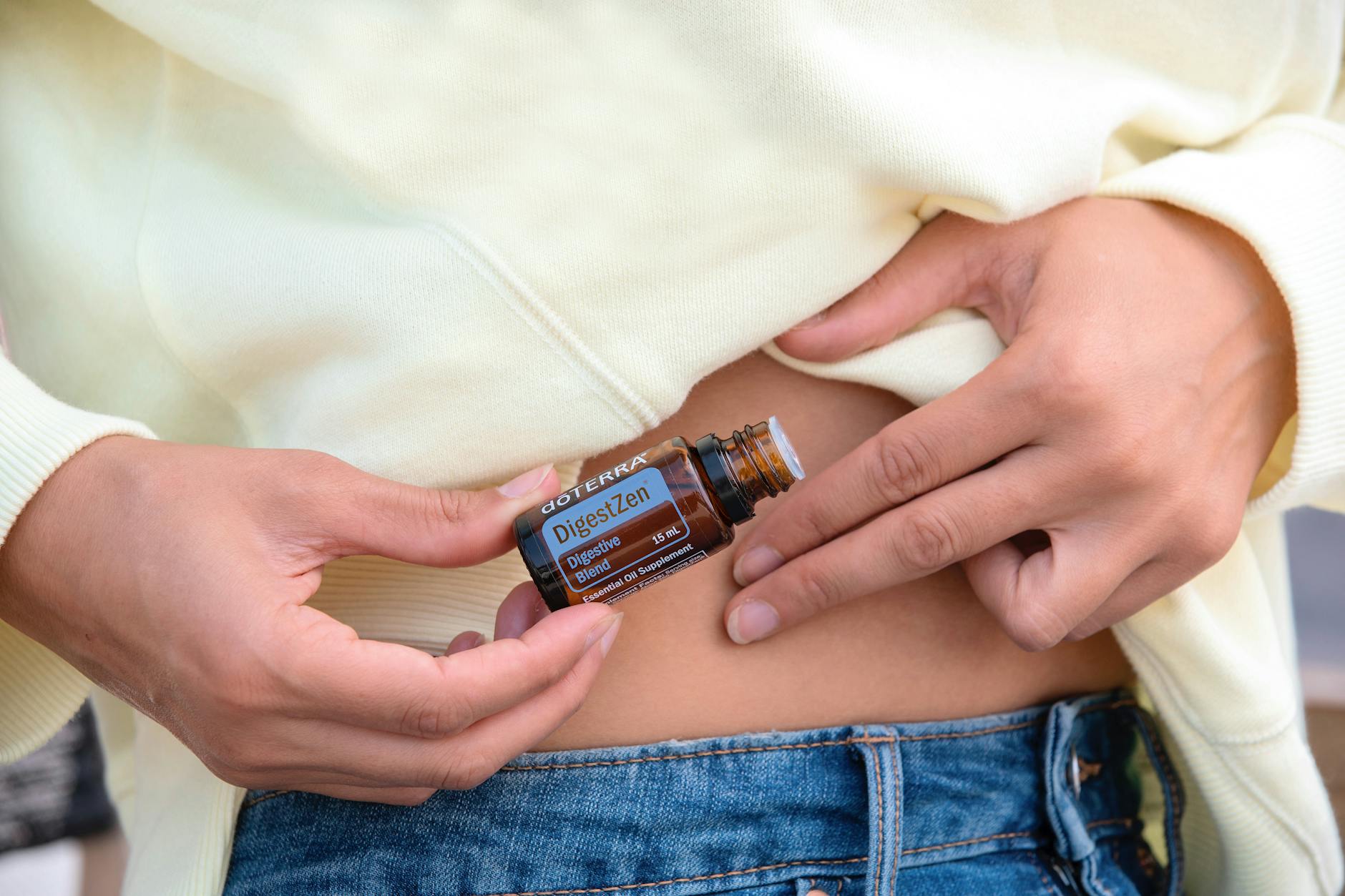
Changes in bowel habits, including frequency, consistency, color, or the presence of blood, are frequently considered too embarrassing to mention. These symptoms are among the most diagnostically important that a doctor can receive, as they relate to conditions ranging from irritable bowel syndrome to colorectal cancer. Persistent bloating, constipation, diarrhea, or abdominal discomfort should always be disclosed even when they seem minor or cyclical. Early reporting of these changes dramatically improves outcomes for gastrointestinal conditions that respond well to timely intervention.
Past Trauma or Abuse

Physical and emotional trauma from childhood or adulthood has lasting effects on the nervous system, immune function, hormonal balance, and pain sensitivity. Patients who have experienced abuse often present with unexplained chronic pain, fatigue, or anxiety that is difficult to treat without understanding its root context. Doctors are trained to handle trauma disclosures with sensitivity and can connect patients with appropriate therapeutic support. Withholding this information often leads to years of ineffective treatment for symptoms that have a clear psychological origin.
Urinary Symptoms

Leaking urine, frequent urination, difficulty starting the flow, or incomplete bladder emptying are symptoms that patients routinely normalize or feel too embarrassed to raise. These symptoms can indicate urinary tract infections, prostate issues, bladder dysfunction, or early signs of diabetes. Urinary incontinence in particular affects millions of people and has effective treatments that are rarely explored because patients never initiate the conversation. Mentioning these symptoms leads to targeted testing and interventions that significantly improve quality of life.
Memory or Cognitive Concerns

Forgetting names, losing train of thought frequently, or noticing changes in concentration or decision-making are often brushed off as normal signs of aging. These experiences can be early indicators of nutritional deficiencies, thyroid dysfunction, sleep disorders, or the beginning stages of cognitive decline. Doctors can order simple blood panels and cognitive assessments that help rule out treatable causes before more serious conditions develop. Early disclosure creates a documented baseline that is invaluable for tracking changes over time.
Vision or Hearing Changes

Gradual changes in vision or hearing are frequently adapted to rather than reported, with patients unaware that these shifts can indicate broader health issues. Deteriorating peripheral vision can be an early sign of glaucoma, while sudden changes in hearing may relate to cardiovascular health or neurological conditions. Doctors who are informed of these changes can make appropriate referrals to specialists before irreversible damage occurs. Regular documentation of sensory changes also helps distinguish age-related progression from pathological deterioration.
Skin Changes

New moles, changes in existing spots, unusual rashes, persistent itching, or areas of discoloration are commonly overlooked during checkups because patients assume they are cosmetic concerns. The skin is the body’s largest organ and reflects internal conditions including autoimmune disease, hormonal imbalance, liver dysfunction, and nutritional deficiency. Dermatological changes noted by a general practitioner can prompt biopsies or specialist referrals that catch skin cancers at highly treatable stages. Patients should describe any skin changes they have noticed since their last appointment even if they appear minor.
Over-the-Counter Medication Reliance

Regular use of pain relievers, antacids, antihistamines, laxatives, or sleep aids is rarely volunteered during appointments. Frequent reliance on these products often signals an underlying condition that warrants investigation rather than ongoing self-management. Long-term use of anti-inflammatory medications can damage the stomach lining and kidneys, while regular antacid use may indicate acid reflux disease requiring targeted treatment. Doctors need this information to assess organ health and to determine whether ongoing symptoms deserve a more formal diagnosis.
Exercise Habits

Both inactivity and excessive exercise are medically significant and often misrepresented during checkups. Sedentary behavior is a major risk factor for cardiovascular disease, type 2 diabetes, and musculoskeletal deterioration. Overtraining, conversely, can lead to hormonal disruption, stress fractures, and immune suppression that presents as chronic fatigue or frequent illness. Accurate reporting of physical activity levels enables doctors to tailor recommendations and identify exercise-related injuries or imbalances that need attention.
Relationship or Domestic Issues

Stressful or unsafe home environments have direct and measurable effects on physical health outcomes. Living with conflict, isolation, emotional abuse, or a controlling partner contributes to elevated blood pressure, disrupted sleep, weakened immunity, and increased inflammation. Doctors can connect patients with social workers, counselors, or domestic support services when they are aware of the broader life context. Patients are not required to share every detail but mentioning ongoing stress at home opens important doors for support.
Dental Health
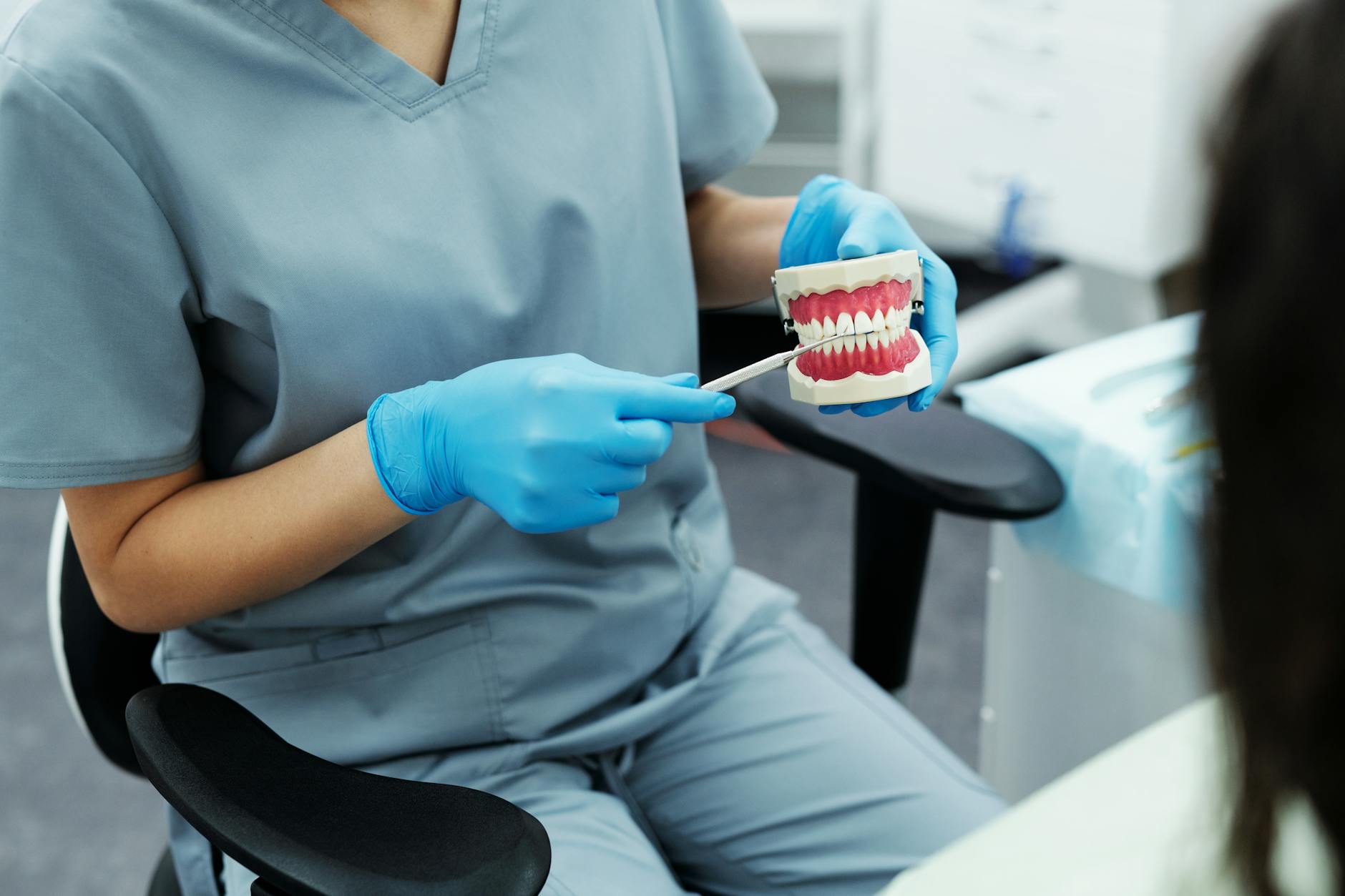
Oral health is rarely discussed during general medical checkups despite being closely linked to systemic conditions including heart disease, diabetes, and pregnancy complications. Bleeding gums, persistent bad breath, tooth pain, or jaw tension can indicate bacterial infections that affect the entire body. Patients who have not seen a dentist in several years or who have ongoing dental issues should disclose this to their general practitioner. Doctors can assess related risk factors and reinforce the importance of oral care within a broader health management plan.
Appetite Changes

Significant increases or decreases in appetite, or changes in taste and hunger cues, are often attributed to stress and left unreported. These shifts can be early indicators of thyroid conditions, diabetes, depression, digestive disorders, or in some cases malignancy. Unintentional weight loss is considered a red flag symptom in most clinical contexts and should always be disclosed even when the cause seems obvious. Tracking appetite changes alongside weight and energy levels gives doctors important data points for investigating underlying causes.
Irregular Periods or Hormonal Symptoms

Menstrual irregularities, spotting between periods, severe cramps, or symptoms suggesting perimenopause are frequently normalized rather than reported. These experiences can indicate polycystic ovary syndrome, thyroid imbalance, uterine fibroids, or other conditions with effective treatment pathways. Hormonal fluctuations also affect bone density, mood, cardiovascular health, and metabolic function in ways that require monitoring. Documenting these patterns and sharing them during checkups allows for appropriate hormone panels and gynecological referrals.
Chest Discomfort or Palpitations

Brief episodes of chest tightness, fluttering, pounding, or irregular heartbeats are often dismissed as anxiety or caffeine-related and never mentioned to a doctor. These symptoms can reflect arrhythmias, valve abnormalities, electrolyte imbalances, or early cardiovascular disease that responds well to early intervention. Patients frequently wait until symptoms become severe before reporting them, missing a window for low-risk investigation and management. Even occasional episodes are worth documenting and discussing as part of a complete cardiovascular history.
Headache Frequency and Severity

Most people experience headaches and treat them independently without considering them worth raising during a routine appointment. Frequent headaches, changes in headache pattern, or episodes accompanied by visual disturbances, nausea, or neck stiffness carry diagnostic significance. Tension headaches, migraines, cluster headaches, and headaches related to blood pressure or neurological conditions all require different management approaches. Providing a clear account of headache frequency, location, duration, and triggers allows doctors to investigate underlying causes rather than simply address symptoms.
Joint Pain or Stiffness

Aching joints, morning stiffness, swelling, or reduced range of motion are widely accepted as inevitable signs of aging and therefore rarely reported. These symptoms can indicate autoimmune conditions such as rheumatoid arthritis, inflammatory diseases, gout, or early osteoarthritis that benefit significantly from early management. Untreated joint inflammation can cause permanent structural damage that is avoidable with appropriate intervention. Describing when symptoms occur, which joints are affected, and whether they improve with movement gives doctors the context needed for accurate assessment.
Shortness of Breath

Mild breathlessness during light activity or at rest is often attributed to being unfit and left unmentioned during appointments. This symptom can indicate anemia, asthma, cardiac conditions, thyroid dysfunction, or pulmonary disease depending on the broader clinical picture. Patients who notice they are more breathless than they used to be during everyday activities should flag this even if the change seems gradual. Doctors will assess whether further testing such as lung function evaluation or cardiac imaging is appropriate based on a full symptom description.
Fatigue

Persistent tiredness that does not improve with rest is one of the most underreported symptoms in primary care settings. Chronic fatigue can result from thyroid disorders, anemia, sleep apnea, depression, autoimmune conditions, or nutritional deficiencies, all of which have effective treatments. Many patients assume fatigue is simply a consequence of a busy lifestyle and never consider it a legitimate medical concern to raise. Sharing how long the fatigue has persisted, whether it is constant or cyclical, and how it affects daily functioning helps doctors narrow down the most likely causes.
Family Medical History Updates

Patients often provide a family history once and assume it remains on file without needing to be revisited. New diagnoses in close relatives, particularly parents or siblings, can significantly change a patient’s own risk profile for genetic or hereditary conditions. Heart disease, certain cancers, diabetes, and autoimmune disorders all carry hereditary components that influence screening recommendations. Mentioning any relevant family health developments since the last appointment ensures that preventive strategies remain aligned with the most current risk information.
Swelling or Fluid Retention
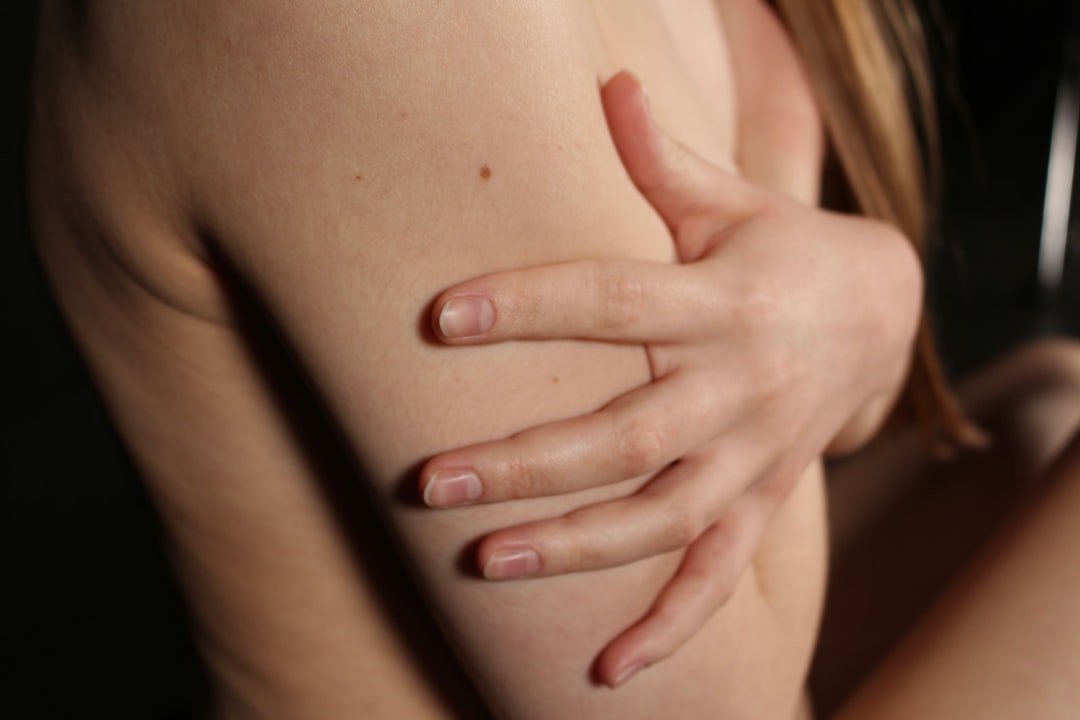
Puffiness in the hands, ankles, feet, or face that appears regularly or worsens throughout the day is frequently ignored or attributed to diet. Edema can indicate kidney dysfunction, heart failure, venous insufficiency, thyroid conditions, or medication side effects depending on the pattern and location. The timing of swelling, whether it improves overnight or is constant, and whether it is accompanied by other symptoms helps doctors determine the most appropriate investigation. Documenting these patterns before an appointment makes the clinical conversation significantly more productive.
Changes in Libido

A significant decrease or increase in sex drive is rarely volunteered during general health checkups despite being a meaningful clinical indicator. Libido changes can reflect hormonal shifts, thyroid dysfunction, depression, medication side effects, or relationship dynamics that have physical health implications. Doctors who are aware of these changes can assess hormonal panels, review prescriptions, and refer patients to appropriate specialists. Addressing this topic does not require a detailed personal disclosure but mentioning the change and its approximate timeline is sufficient to guide further inquiry.
Unexplained Weight Changes

Gaining or losing weight without intentional dietary or activity changes is considered a significant clinical symptom in most contexts. These shifts can indicate thyroid dysfunction, insulin resistance, fluid retention, hormonal imbalance, gastrointestinal conditions, or in some cases more serious underlying illness. Patients who notice consistent weight changes over weeks or months should mention them even when the amount seems small. Tracking approximate weight over time and noting any associated symptoms provides valuable data for guiding investigation.
Stress Levels

Chronic psychological stress is a major driver of physical health deterioration and is rarely discussed openly during routine appointments. Sustained stress elevates cortisol, disrupts sleep, suppresses immune function, raises blood pressure, and accelerates cellular aging in clinically measurable ways. Doctors who understand a patient’s current stress load can contextualize symptoms more accurately and recommend appropriate interventions including therapy, lifestyle modifications, or stress-related medication review. Being honest about workload, caregiving responsibilities, grief, or life transitions helps doctors provide care that reflects the full picture of a patient’s health.
Dizziness or Balance Issues

Occasional dizziness or feeling unsteady is commonly normalized, particularly among older adults, but represents a symptom category with a wide range of possible causes. Inner ear dysfunction, blood pressure irregularities, medication interactions, anemia, and neurological conditions all present with dizziness as a primary symptom. Falls related to balance problems are one of the leading causes of serious injury in adults over sixty and are highly preventable with appropriate assessment. Describing when dizziness occurs, how long it lasts, and whether it is accompanied by nausea or visual changes gives doctors a clearer diagnostic picture.
Medication Adherence

Patients who are not taking their prescribed medications as directed rarely disclose this during appointments, often fearing judgment or a lecture from their doctor. Non-adherence affects how doctors interpret lab results, blood pressure readings, and symptom patterns, potentially leading to unnecessary dose increases or additional prescriptions. Reasons for non-adherence including cost, side effects, forgetfulness, or doubts about effectiveness are all addressable issues that doctors can help resolve. Honest communication in this area leads to more practical prescribing and better health outcomes overall.
Dental Grinding or Jaw Clenching
Bruxism, or the habitual grinding and clenching of teeth during sleep or periods of stress, is rarely considered a medical issue worth raising. Chronic grinding contributes to jaw pain, tension headaches, disrupted sleep, and dental erosion that affects overall health and quality of life. It is also frequently linked to sleep apnea, anxiety disorders, and certain neurological conditions that warrant further evaluation. Mentioning jaw tightness, worn teeth, or morning headaches gives doctors the context to investigate contributing factors and recommend appropriate intervention.
Foot and Nail Changes

Changes in the appearance of feet and toenails, including discoloration, thickening, unusual growth patterns, or loss of sensation, are considered cosmetic and left unmentioned. These changes can signal peripheral artery disease, diabetes-related nerve damage, fungal infection, or nutritional deficiencies with systemic implications. Loss of sensation or cold feet in particular is an important early warning sign for conditions that become significantly harder to manage once they progress. Raising these observations during a checkup allows doctors to examine circulation, nerve function, and metabolic health in a targeted way.
What do you find hardest to bring up with your doctor, and has avoiding it ever affected your health? Share your experience in the comments.




