Your immune system works silently around the clock to protect your body from infection, disease, and cellular damage. When it begins to falter, the signals are often subtle at first before becoming impossible to ignore. Understanding these warning signs can help you take action before a weakened immune response leads to serious health complications. Recognizing patterns in how your body responds to illness, stress, and everyday life is one of the most powerful tools for protecting your long-term wellbeing. If several of these signs feel familiar, speaking with a healthcare professional is a smart and necessary step.
Frequent Infections

People with a compromised immune system tend to catch colds, throat infections, and ear infections far more often than average. Falling sick more than two or three times per year with respiratory illnesses is a recognized clinical indicator of reduced immune function. The body struggles to mount a fast and effective defence against pathogens it would normally neutralize quickly. Recovery periods also tend to stretch longer than expected, with symptoms lingering well past the typical window. Chronic or recurring infections of the sinuses, skin, or urinary tract are especially telling patterns to monitor.
Slow Wound Healing
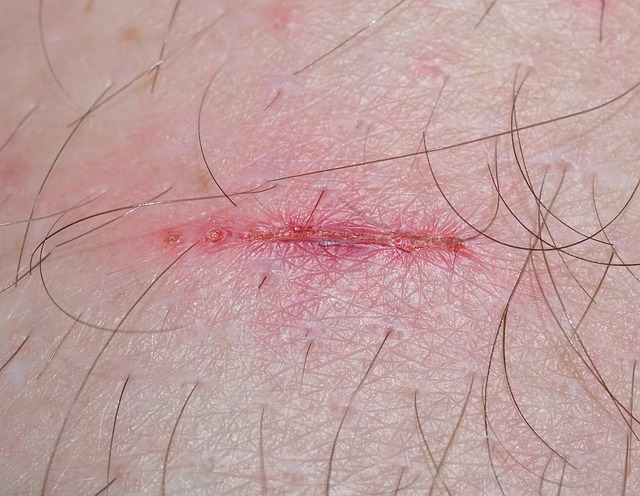
Cuts, scrapes, and bruises that take an unusually long time to close and fade can point to immune dysfunction. The healing process depends heavily on immune cells rushing to the site of injury to fight bacteria and begin tissue repair. When those cells are sluggish or insufficient in number, the skin struggles to regenerate at a normal pace. Wounds that remain open, inflamed, or prone to re-infection are a particular cause for concern. Delayed healing is often one of the earlier physical signs that something is disrupting normal immune activity.
Persistent Fatigue

Feeling exhausted despite getting adequate sleep is a widely reported symptom among those with weakened immune systems. The body expends enormous energy trying to maintain its defences when the immune system is under constant strain. This creates a cycle where the system is perpetually working overtime without achieving effective results. Unlike ordinary tiredness from overwork or poor sleep, immune-related fatigue tends to be deep, unrelenting, and resistant to rest. When fatigue coexists with other symptoms on this list, it becomes a much stronger signal worth investigating medically.
Digestive Problems

A significant portion of the immune system resides in the gut, making digestive health and immune health deeply interconnected. Frequent bouts of diarrhea, bloating, nausea, or constipation that have no clear dietary cause may reflect immune system disruption. An imbalanced gut microbiome can both result from and contribute to declining immune function in a reinforcing cycle. Inflammatory bowel conditions and food sensitivities that appear or worsen suddenly are also associated with immune dysregulation. Persistent gastrointestinal discomfort lasting more than a few weeks warrants a thorough medical evaluation.
Recurring Fever
Low-grade fevers that appear repeatedly without an obvious underlying infection suggest the immune system is in a state of ongoing activation. The body raises its temperature as a defensive mechanism, and when this happens frequently it may indicate the system is perpetually fighting something it cannot resolve. Temperatures that hover just above normal for days or weeks at a time are distinct from the high fevers associated with acute illness. This pattern is common in autoimmune conditions where the immune system becomes dysregulated and begins attacking the body’s own tissues. Recurrent unexplained fevers should always be evaluated by a physician to rule out serious underlying causes.
Stress-Related Illness

Chronic psychological stress is one of the most well-documented suppressors of immune function in medical research. Elevated cortisol levels sustained over long periods actively reduce the production and effectiveness of immune cells. People who fall ill consistently during or immediately after periods of high stress are displaying a classic sign of stress-compromised immunity. The relationship between the nervous system and the immune system is deeply biological and not merely a matter of perception. Managing chronic stress is therefore a direct medical intervention with measurable effects on immune resilience.
Skin Conditions
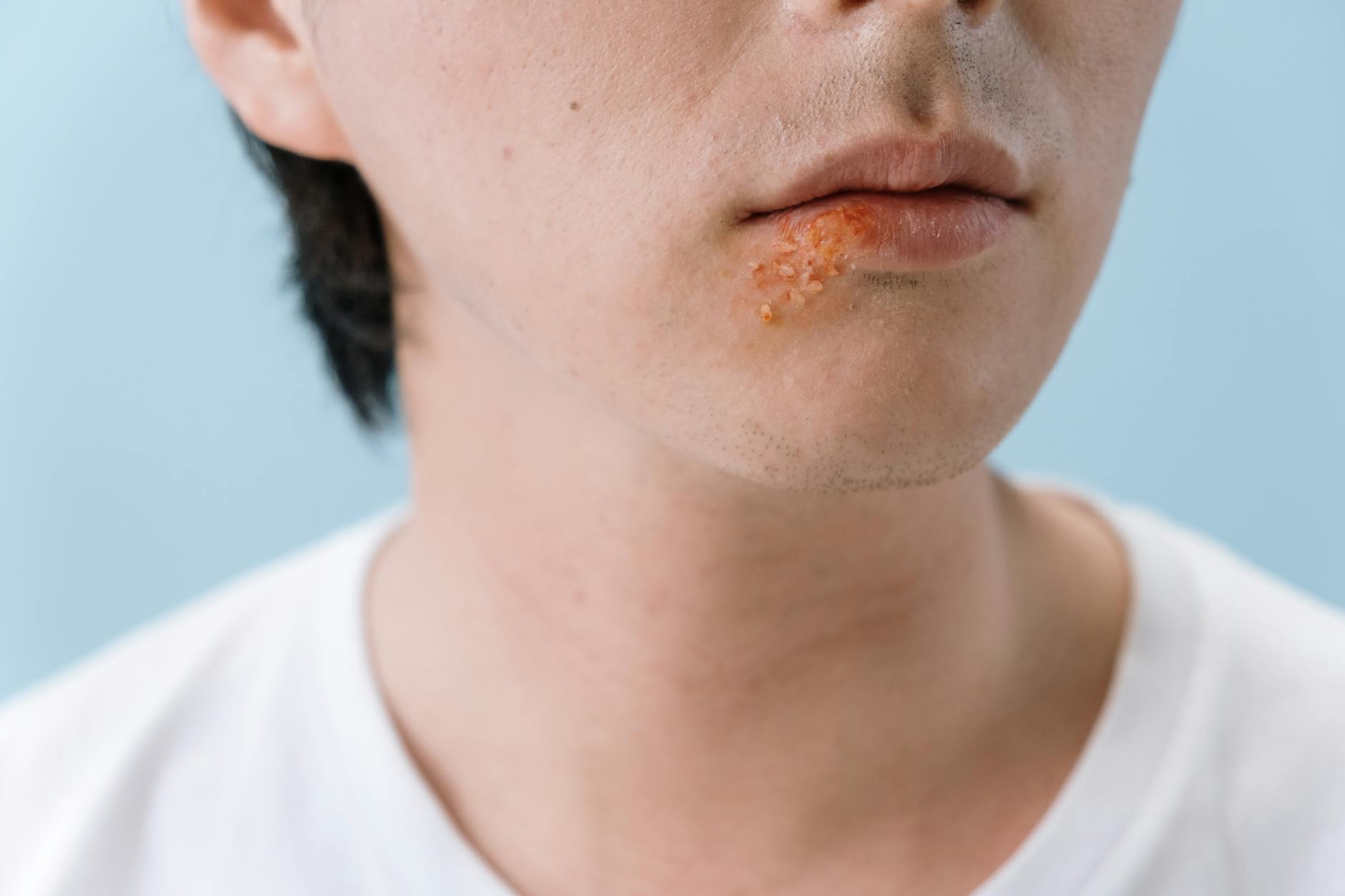
The skin is both a physical barrier and an active component of the immune system, making it a visible indicator of immune health. Recurring rashes, hives, eczema flare-ups, and unexplained skin inflammations can point to immune dysfunction rather than purely dermatological causes. A compromised immune system may fail to regulate inflammatory responses in the skin appropriately, resulting in persistent or cyclical outbreaks. Conditions like psoriasis are now understood to involve significant immune system irregularities at their core. Skin symptoms that are chronic, widespread, or unresponsive to standard topical treatments deserve further immunological investigation.
Oral Health Changes
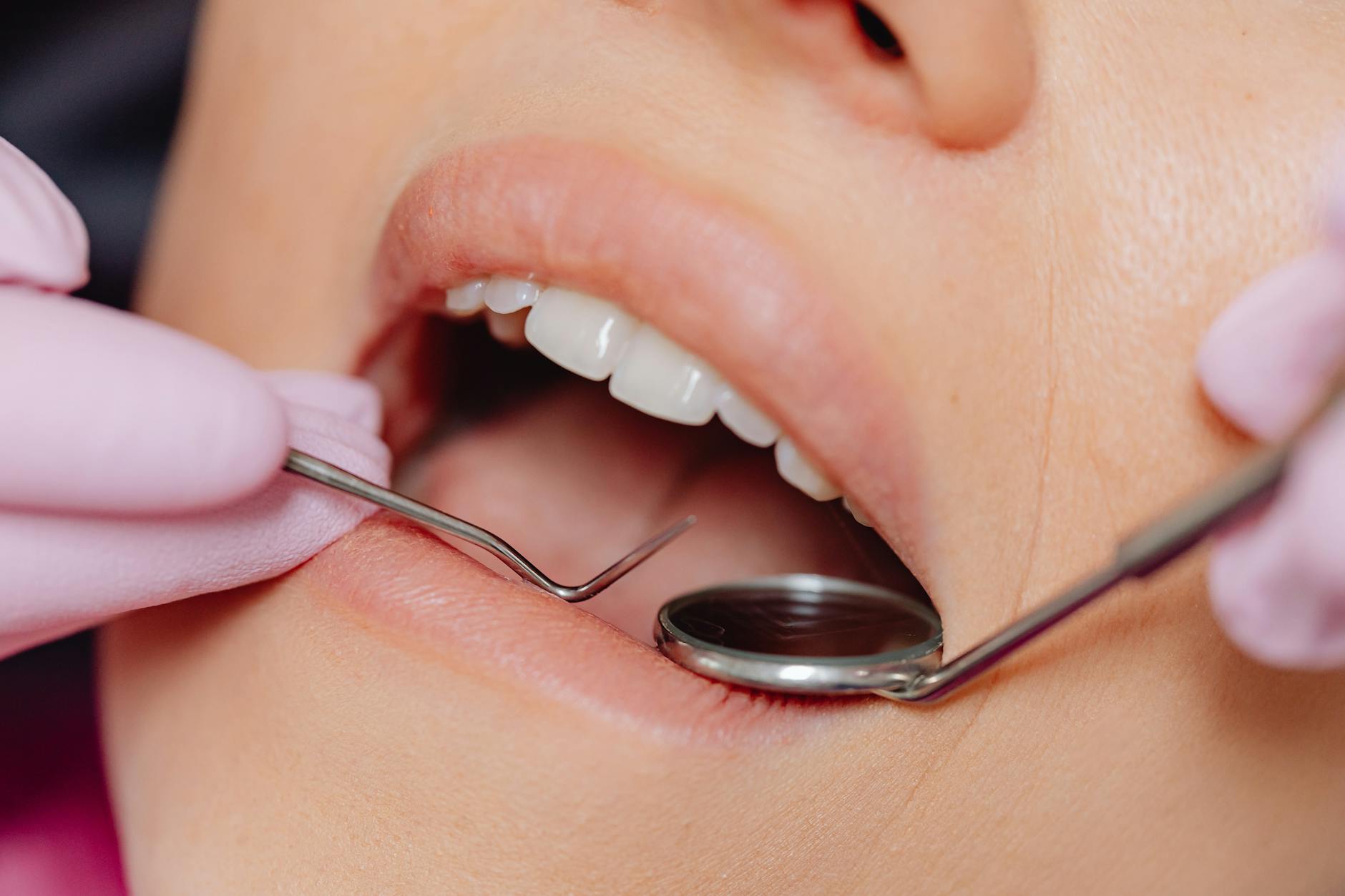
Frequent mouth ulcers, cold sores, inflamed gums, and oral thrush are signs that immune activity in the mucosal tissues is reduced. The mouth is a primary entry point for pathogens, and a healthy immune system actively works to prevent opportunistic infections there. Candida overgrowth, which causes oral thrush, is a common marker of immune suppression seen in both mild and severe cases. Gum disease that progresses rapidly or proves resistant to treatment may also reflect broader immune system weakness. Dentists and oral health professionals are sometimes the first to notice patterns that suggest systemic immune issues.
Hair Loss

Sudden or accelerating hair loss beyond normal shedding can be connected to immune system dysregulation. Alopecia areata is a condition in which the immune system mistakenly attacks hair follicles, resulting in patchy or widespread hair loss. Nutritional deficiencies that impair immune function, such as low zinc or iron, simultaneously affect hair growth and density. Prolonged physical stress on the immune system from chronic illness can trigger telogen effluvium, a type of diffuse hair shedding. While hair loss has many potential causes, its appearance alongside other immune-related symptoms makes it a meaningful piece of the broader picture.
Eye Inflammation
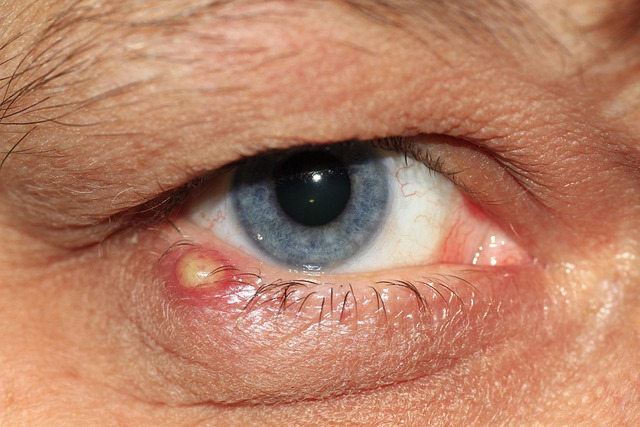
Recurring pink eye, blurry vision episodes, or chronic dry eye that resists standard treatment can all be linked to immune system irregularities. The eyes contain specialized immune cells and tissues that help defend against pathogens while minimizing inflammatory damage to sensitive structures. When systemic immune function is compromised, these local defences can become dysregulated, leading to visible inflammation and discomfort. Uveitis, an inflammation of the middle layer of the eye, is frequently associated with autoimmune and immune deficiency conditions. Persistent or unexplained eye inflammation should prompt a conversation with both an ophthalmologist and a general practitioner.
Joint Pain

Unexplained joint pain and swelling that migrates between locations or appears without obvious physical cause can indicate immune involvement. Inflammatory arthritis conditions, including rheumatoid arthritis, are driven by immune system activity that targets joint tissue in error. The immune system releases inflammatory molecules called cytokines that, when overproduced, cause pain, stiffness, and swelling in the joints. Morning stiffness lasting more than an hour and joint symptoms that improve with movement rather than rest are particularly characteristic of immune-driven inflammation. Tracking when and where joint pain occurs can provide valuable information for a rheumatologist assessing potential immune causes.
Autoimmune Flares
When the immune system turns against the body’s own healthy cells, it produces a category of conditions collectively known as autoimmune diseases. Flares involving unexplained inflammation in multiple organ systems simultaneously are a strong indicator of serious immune dysfunction. Conditions such as lupus, multiple sclerosis, and celiac disease all involve varying degrees of misdirected immune activity. The presence of one autoimmune condition significantly increases the statistical likelihood of developing another, suggesting a systemic regulatory breakdown. Any pattern of symptoms involving multiple body systems appearing and resolving unpredictably warrants urgent rheumatological or immunological assessment.
Blood Abnormalities

Routine blood tests can reveal important information about immune system status through white blood cell counts and differential analysis. A consistently low white blood cell count, a condition known as leukopenia, indicates reduced capacity to fight infection. Conversely, persistently elevated white blood cell counts without active infection suggest the immune system is in a state of chronic activation. Abnormal levels of specific immune cell types, such as neutrophils or lymphocytes, help clinicians identify the nature of any immune dysregulation present. Regular blood monitoring is especially important for people who notice multiple symptoms from this list appearing together.
Allergic Reactions

An immune system that is dysregulated may become hypersensitive, producing exaggerated allergic responses to substances it previously tolerated. New allergies developing in adulthood, or existing allergies worsening significantly, can point to a shift in immune system calibration. Anaphylactic reactions and severe food intolerances that appear without prior history are particularly notable warning signs. The immune system in these cases misidentifies harmless substances as dangerous threats and mounts a disproportionate defensive response. Understanding whether allergic symptoms are increasing in frequency or severity is a useful gauge of how well the immune system is regulating itself.
Sleep Disruption

The immune system performs critical repair and regulatory functions during sleep, making poor or disrupted sleep both a cause and a consequence of immune weakness. Research consistently shows that individuals sleeping fewer than six hours per night produce significantly fewer immune cells and antibodies. Chronic insomnia or fragmented sleep prevents the body from completing the overnight immune maintenance processes it depends on. Elevated inflammatory markers in the blood have been directly linked to prolonged sleep deprivation in clinical studies. Addressing sleep quality is therefore not merely a lifestyle recommendation but a genuine medical intervention for immune support.
Vitamin Deficiencies

Deficiencies in key micronutrients directly impair the immune system’s ability to function at a basic biological level. Vitamin D plays a central role in activating immune cells and regulating the inflammatory response, and its deficiency is strongly correlated with increased susceptibility to infection. Low levels of zinc, selenium, vitamin C, and B vitamins each affect different components of the immune cascade in documented and measurable ways. Many deficiencies are asymptomatic in the early stages, making regular blood testing the only reliable way to identify them. Correcting nutritional deficiencies through diet and medically supervised supplementation is one of the most effective routes to restoring immune function.
Lymph Node Swelling
Lymph nodes are central hubs of immune activity and their behaviour provides direct insight into how the immune system is responding to perceived threats. Swollen lymph nodes that appear and disappear frequently, without any accompanying obvious infection, suggest the immune system is continuously activating. Nodes that remain enlarged for more than two weeks, feel hard, or appear in multiple locations simultaneously require prompt medical evaluation. Persistent swelling can indicate that the immune system is fighting an ongoing infection it cannot resolve, or that more serious conditions are affecting lymphatic tissue. Paying attention to recurring or prolonged lymph node activity is an important and often overlooked aspect of immune self-monitoring.
Chronic Inflammation

Inflammation is a natural and essential part of the immune response but chronic low-level inflammation indicates the system is stuck in a permanent state of alert. Elevated levels of C-reactive protein and other inflammatory markers found in blood tests are associated with long-term immune dysregulation. Conditions driven by chronic inflammation include cardiovascular disease, type 2 diabetes, and certain cancers, all of which have documented links to immune system dysfunction. Physical signs of chronic inflammation can include persistent puffiness, redness, warmth in tissues, and general bodily discomfort without an identifiable source. Lifestyle interventions such as dietary changes, stress reduction, and improved sleep have measurable impacts on reducing systemic inflammation.
Temperature Sensitivity

An unusual sensitivity to cold or difficulty maintaining normal body temperature can sometimes reflect thyroid involvement linked to immune dysfunction. Autoimmune thyroid conditions such as Hashimoto’s thyroiditis cause the immune system to attack thyroid tissue, disrupting temperature regulation and metabolic function. People with poor circulation resulting from immune-related vascular inflammation may also experience unusual coldness in the extremities. Feeling consistently colder than others in the same environment, or experiencing unexplained temperature fluctuations, is worth discussing with a doctor. When combined with fatigue, hair changes, and mood shifts, temperature dysregulation forms part of a recognizable cluster of immune and endocrine warning signs.
Mood Changes

Emerging research in psychoneuroimmunology has established meaningful biological links between immune system activity and mental health. Elevated inflammatory cytokines produced during immune activation have been shown to directly affect brain chemistry and contribute to depressive symptoms. Anxiety, brain fog, and cognitive slowdown are increasingly recognized as potential manifestations of chronic immune dysregulation rather than purely psychological phenomena. People experiencing persistent low mood or mental fatigue alongside physical symptoms may be dealing with an immune component that conventional mental health treatments alone will not resolve. Addressing inflammation and immune function as part of a comprehensive mental health approach is a growing area of clinical interest and practice.
If any of these warning signs feel familiar to you, share your experience and questions in the comments.





