Protein is one of the most essential macronutrients the human body relies on to function properly every single day. It supports muscle repair, immune defense, hormone production and the structural integrity of nearly every tissue in the body. When intake falls short, the body begins sending clear physical signals that something is off. Recognizing these signs early can help prevent longer-term health consequences and guide meaningful dietary adjustments. The following 25 signs are ordered from the least critical to the most telling indicators of protein deficiency.
Brittle Nails

Nails are made largely from a protein called keratin, which gives them their structure and strength. When dietary protein is insufficient, the body redirects available amino acids toward more vital functions, leaving nails without adequate building material. This results in nails that chip, crack or peel with very little pressure. The condition tends to worsen progressively the longer protein intake remains low. Brittle nails are often one of the earliest cosmetic signals of a nutritional imbalance.
Dry Skin

The skin relies on collagen and elastin, both of which are protein-based structures that maintain its firmness and moisture barrier. A shortfall in dietary protein reduces the body’s ability to produce and repair these structural components. As a result, the skin may become dry, flaky or rough to the touch even with regular moisturizing. Areas like the elbows, shins and heeks are often the first to show visible signs of this dryness. Persistent dry skin unrelated to climate or topical products can point to an underlying nutritional gap.
Slow Wound Healing
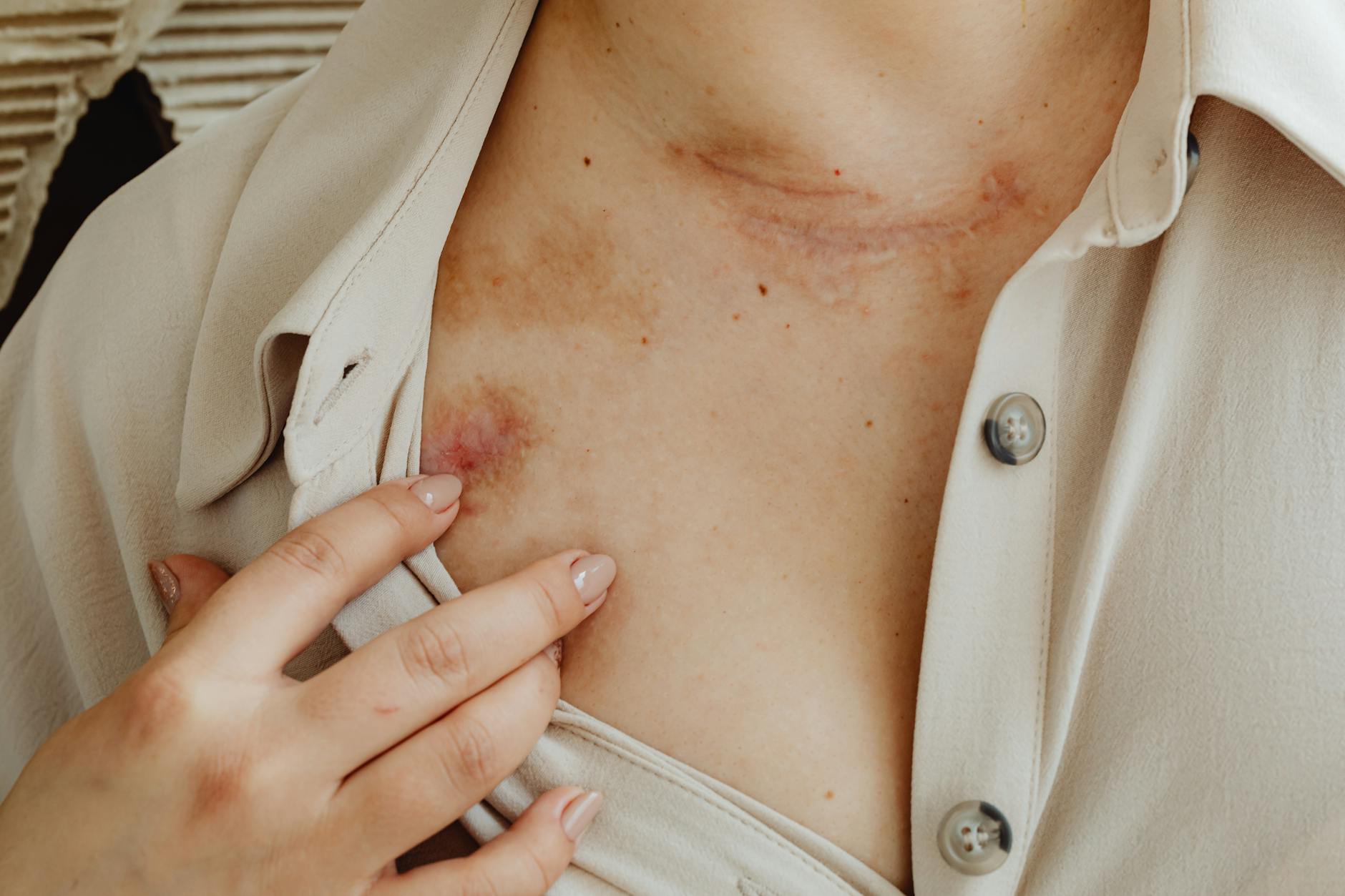
The body depends heavily on protein to rebuild damaged tissue following cuts, bruises or surgical wounds. Amino acids are the raw material used to form new skin cells and support the inflammatory response that initiates healing. When protein is scarce, each stage of the healing process takes considerably longer than normal. Minor wounds that would ordinarily close within days may linger for weeks. This delayed recovery is a meaningful clinical indicator that protein intake needs attention.
Thinning Hair

Hair strands are composed almost entirely of keratin, making adequate protein intake critical for their growth and integrity. When the body experiences a protein shortage, it enters a conservation mode and reduces energy allocated to non-essential functions like hair production. This can cause existing strands to thin, weaken and fall out at a higher rate than usual. A noticeable increase in hair found on pillows, brushes or in the shower drain is a common early observation. Thinning hair related to diet typically appears across the entire scalp rather than in isolated patches.
Hair Loss

Beyond general thinning, pronounced hair loss can occur when protein deficiency becomes more severe or prolonged. The hair growth cycle depends on a consistent supply of amino acids during the active growth phase known as anagen. Without sufficient protein, follicles may prematurely enter the resting phase, triggering a condition called telogen effluvium. This results in diffuse shedding that can be alarming in its volume. Nutritional hair loss is reversible in most cases once protein intake is restored to adequate levels.
Muscle Cramps

Muscle tissue requires protein for both structural maintenance and the regulation of electrolyte balance that governs muscle contractions. A deficiency can leave muscle fibers more vulnerable to involuntary contractions and spasms. Cramps may occur more frequently during physical activity or even at rest, particularly in the legs and feet. The connection between low protein and cramping is also linked to reduced levels of albumin, a protein that helps transport nutrients through the bloodstream. Recurring cramps without an obvious cause such as dehydration or overexertion may warrant a closer look at dietary protein intake.
Poor Concentration

Protein plays a direct role in the synthesis of neurotransmitters such as dopamine and serotonin, which regulate focus, mood and cognitive performance. Amino acids like tyrosine and tryptophan serve as precursors to these brain chemicals and must be obtained through diet. When protein is lacking, neurotransmitter production can become disrupted, leading to difficulty concentrating on tasks. Mental fog, forgetfulness and reduced alertness are commonly reported in individuals with consistently low protein consumption. These cognitive effects can significantly impact daily productivity and overall quality of life.
Mood Changes

The brain’s emotional regulation systems are closely tied to the availability of amino acids from dietary protein. Serotonin in particular, which depends on tryptophan for its production, influences feelings of wellbeing and emotional stability. A reduction in these neurotransmitter precursors can contribute to irritability, low mood and heightened sensitivity to stress. Mood fluctuations that appear without a clear psychological cause may have a nutritional explanation. Addressing protein intake has been observed to support more stable emotional functioning in individuals with identified deficiencies.
Sleep Disturbances

Protein contributes to the production of melatonin, the hormone responsible for regulating the sleep-wake cycle. Tryptophan, an essential amino acid found in protein-rich foods, is converted into serotonin and then into melatonin within the body. When tryptophan availability is low due to insufficient protein intake, melatonin synthesis may be compromised. This can manifest as difficulty falling asleep, frequent nighttime waking or a general sense of unrefreshing sleep. Improving dietary protein has been associated with better sleep quality in nutritional research.
Food Cravings

The body uses appetite signals to communicate unmet nutritional needs, and protein deficiency is known to trigger persistent cravings. When meals lack sufficient protein, satiety hormones such as peptide YY and GLP-1 are not adequately stimulated. This leaves individuals feeling hungry shortly after eating and often reaching for high-carbohydrate or sugary foods. These cravings are the body’s attempt to find quick energy in the absence of the sustained fuel that protein provides. Recognizing this pattern as a potential protein signal rather than a habit or willpower issue is an important distinction.
Constant Hunger

Protein is the most satiating of the three macronutrients, with a well-documented ability to reduce appetite and prolong feelings of fullness. When meals are consistently low in protein, hunger hormones such as ghrelin remain elevated, keeping appetite signals active. This results in a near-constant desire to eat regardless of caloric intake from fats and carbohydrates. The body is not simply seeking more food but is specifically seeking the amino acids it requires for ongoing biological processes. Persistent hunger despite regular meals is one of the more telling behavioral signs of inadequate protein consumption.
Frequent Illness

The immune system relies on protein to produce antibodies, immune cells and signaling molecules that defend the body against pathogens. A deficiency in dietary protein can impair the production and function of these protective components. Individuals with low protein intake may find themselves catching colds, infections or viruses more frequently than others. Recovery from illness may also take longer as the immune response is unable to mobilize effectively. A pattern of frequent illness without an obvious medical explanation is a recognized indicator of potential nutritional deficiency.
Swollen Feet

A condition known as edema, characterized by swelling in the feet and ankles, can develop when blood protein levels fall too low. Albumin and other plasma proteins are responsible for maintaining osmotic pressure, which keeps fluid within blood vessels rather than leaking into surrounding tissues. When these proteins are depleted, fluid accumulates in the lower extremities due to gravity. The swelling is typically soft and leaves an indentation when pressed with a finger. This form of edema is a more advanced sign of protein deficiency and warrants medical evaluation.
Puffy Face

Similar to the swelling observed in the feet, the face can also retain excess fluid when plasma protein levels are insufficient. This is particularly noticeable in the area around the eyes and cheeks upon waking in the morning. Facial puffiness caused by protein deficiency is distinct from normal morning swelling and tends to persist or worsen over time. It reflects the same mechanism of osmotic imbalance that drives edema in other parts of the body. Recognizing this as a potential nutritional symptom rather than simply a cosmetic concern is important for proper assessment.
Flaky Scalp

The scalp, like all skin tissue, requires protein-derived nutrients to maintain its cellular turnover and protective function. When protein availability decreases, the scalp may produce dead skin cells at an irregular rate, leading to visible flaking. This condition can resemble dandruff but is rooted in nutritional deficiency rather than fungal activity or scalp sensitivity. The scalp may also feel tighter or itchier than usual as its moisture barrier deteriorates. Dietary improvements that restore adequate protein have been reported to reduce scalp flaking in nutritionally deficient individuals.
Muscle Weakness

Skeletal muscle is composed predominantly of protein, and its maintenance requires a continuous supply of amino acids from dietary sources. When intake is insufficient, the body begins breaking down existing muscle tissue to source the amino acids needed for critical organ functions. This process, known as catabolism, results in progressive muscle weakness and reduced physical strength. Tasks that were previously manageable may begin to feel difficult or tiring. Muscle weakness unrelated to injury or neurological conditions is a well-established consequence of sustained protein deficiency.
Joint Pain
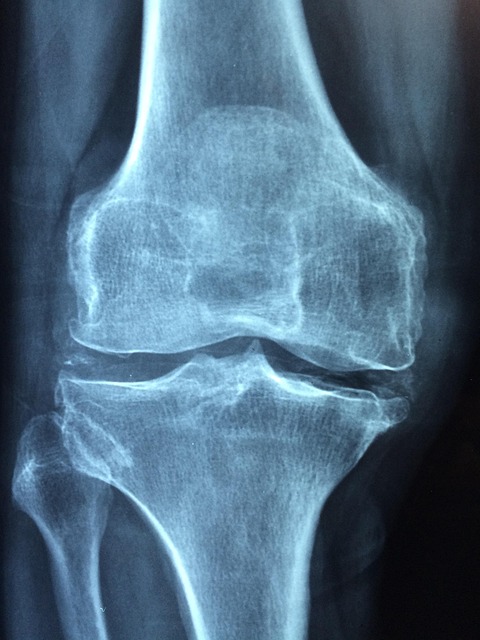
Cartilage, the connective tissue that cushions joints, is built largely from collagen, which is a structural protein. Adequate dietary protein supports the ongoing repair and maintenance of cartilage in weight-bearing and frequently used joints. When protein intake is consistently low, this maintenance process slows and existing cartilage may degrade more rapidly. The result can be aching, stiffness or discomfort in the knees, hips and other joints during movement. While joint pain has many potential causes, nutritional factors including protein status are a valid part of any comprehensive assessment.
Slow Metabolism

Protein has a higher thermic effect than carbohydrates or fats, meaning the body burns more calories digesting and processing it. When dietary protein is low, this metabolic advantage is lost and overall calorie burning can slow as a result. Additionally, the loss of muscle mass that accompanies protein deficiency further reduces the body’s resting metabolic rate. Individuals may notice unexplained weight gain or difficulty maintaining their usual weight despite consistent eating habits. This metabolic shift is a downstream consequence of chronic protein inadequacy rather than a primary cause of deficiency.
Low Energy

Protein contributes to energy regulation not only through its structural roles but also through its involvement in enzyme production and blood sugar stability. Enzymes that power cellular energy production depend on amino acids for their synthesis and function. A lack of dietary protein can therefore leave the body’s energy systems working less efficiently than normal. Fatigue that is not explained by poor sleep or overexertion may reflect this underlying metabolic disruption. Persistent low energy is among the more commonly reported and disruptive symptoms in individuals with inadequate protein intake.
Hormonal Imbalance

Many hormones are either made from protein or depend on protein-derived enzymes for their production and regulation. Insulin, growth hormone and thyroid hormones are among those influenced by the availability of dietary amino acids. When protein is lacking, hormonal signaling can become disrupted across multiple systems in the body. Symptoms may include irregular menstrual cycles, changes in body composition, temperature sensitivity and mood instability. A comprehensive nutritional review is often warranted when hormonal irregularities appear without an identifiable medical cause.
Poor Posture

Muscle strength and tone are essential for maintaining proper posture throughout the day, and both depend on adequate protein intake. As the body breaks down muscle in response to protein shortfall, the deep stabilizing muscles of the spine and core weaken first. This can lead to slouching, rounded shoulders and difficulty maintaining an upright position for extended periods. Poor posture arising from muscular insufficiency also increases the risk of back and neck discomfort over time. Addressing nutritional deficiencies is a foundational step in any effort to improve postural alignment and stability.
Anemia

Iron-deficiency anemia is well known, but protein deficiency can also contribute to reduced red blood cell production through a different mechanism. Hemoglobin, the protein within red blood cells that carries oxygen, requires both iron and adequate amino acid availability for its synthesis. When dietary protein is insufficient, the body may struggle to produce enough healthy red blood cells regardless of iron intake. Symptoms include persistent fatigue, pallor and shortness of breath during physical activity. Nutritional anemia of this type is often identified through blood work and a thorough dietary assessment.
Muscle Loss
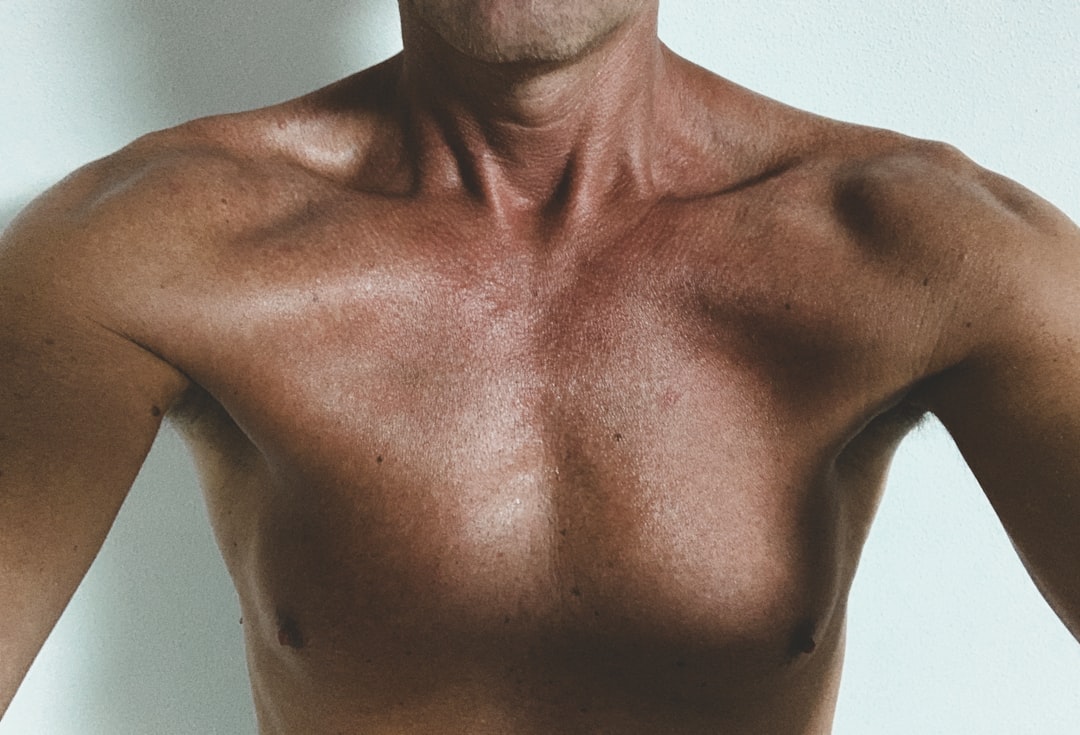
Visible reduction in muscle mass, often described as appearing thinner or less defined, is one of the most direct physical manifestations of protein deficiency. The body prioritizes the needs of vital organs and will sacrifice peripheral muscle tissue to source amino acids when dietary supply is inadequate. This process accelerates with age, making older adults particularly vulnerable to protein-related muscle wasting. Loss of muscle mass also compounds other deficiency symptoms such as weakness, fatigue and metabolic slowdown. Maintaining adequate protein intake is widely recognized as a primary strategy for preserving muscle mass across all age groups.
Stunted Growth

In children and adolescents, protein deficiency carries particularly serious consequences for physical development. Growth hormone activity and the cellular processes that drive bone elongation and tissue expansion all depend on a consistent supply of amino acids. Insufficient protein during critical developmental windows can lead to measurable delays in height gain and overall physical maturation. This is among the most severe outcomes of dietary protein inadequacy and is most commonly observed in regions with widespread food insecurity. Regular monitoring of growth alongside dietary evaluation is essential for ensuring adequate development in young individuals.
Kwashiorkor

Kwashiorkor is a severe form of protein deficiency most commonly seen in young children in regions where food security is critically compromised. It is characterized by a distinctive combination of symptoms including extreme muscle wasting alongside a paradoxically swollen abdomen caused by fluid accumulation. The skin may develop discolored patches and the hair often loses its natural pigment, turning reddish or yellowish. Children with kwashiorkor typically display profound fatigue, irritability and impaired immune function. It represents the most critical end of the protein deficiency spectrum and requires urgent medical and nutritional intervention.
If any of these signs feel familiar to you, share your experience and questions in the comments.





