The pharmacy counter is one of the most consequential points in the entire healthcare system and most patients approach it with a level of trust that does not always include curiosity about what is happening behind the scenes. Pharmacists and pharmacy technicians operate within a complex web of insurance formularies, manufacturer agreements, therapeutic equivalence databases, and dispensing regulations that creates significant latitude for substitution decisions the patient may never be explicitly informed about. Most of these substitutions are entirely legal, frequently beneficial, and often motivated by genuine efforts to reduce patient costs. Understanding the specific mechanisms through which your prescription can legally change between the doctor’s pen and your medicine cabinet is knowledge that every regular medication user should have.
Generic Substitution

The most frequently executed substitution in any retail pharmacy involves replacing a brand-name prescription with its generic bioequivalent, a practice that is legally mandated in many jurisdictions unless the prescribing physician has explicitly written instructions prohibiting substitution on the prescription itself. Generic medications contain the same active pharmaceutical ingredient at the same dosage as the brand-name product and are required by regulatory agencies including the FDA to demonstrate bioequivalence within an accepted range before approval. The financial difference between brand and generic pricing can be substantial with some medications costing ten to twenty times more in their branded form than their generic equivalent. Patients who want to ensure they receive a specific brand must ask their physician to write the prescription with explicit dispense-as-written notation and should expect that insurance coverage may not extend to the brand-name version when a generic is available.
Therapeutic Substitution

A pharmacist working within an institutional or insurance-directed protocol may substitute a medication from the same therapeutic class as the one prescribed rather than a direct chemical equivalent, replacing one drug with a different molecule that treats the same condition through a similar mechanism. This practice is more common in hospital and managed care settings than in independent retail pharmacies but occurs in retail contexts when insurance formulary restrictions make the prescribed medication unavailable for coverage and an alternative within the same drug class is preferred. Therapeutic substitution goes beyond generic equivalence because it involves replacing one drug with a genuinely different drug rather than a chemically identical one and requires pharmacist judgment about clinical equivalence. Patients who notice that the medication they received has a different name than the one their doctor prescribed and are uncertain whether they received a generic or a therapeutic substitute should ask the dispensing pharmacist for a specific explanation of the substitution rationale.
Formulary Tier Shifting

Insurance plan formularies organize covered medications into pricing tiers and pharmacy benefit managers who administer these formularies update their tier assignments periodically in ways that can shift a patient’s medication from a low-cost tier to a higher-cost one without any change to the prescription itself. When a newly preferred alternative enters the formulary at a lower tier the pharmacy system will frequently flag the dispensing opportunity and a pharmacist may initiate contact with the prescribing physician to request a prescription change that benefits the patient’s out-of-pocket cost. This process happens within the administrative infrastructure of the dispensing system and may result in a different medication appearing in the patient’s bag than the one the doctor originally specified. Patients who receive a different medication than prescribed and are told it is a formulary substitution are entitled to a full explanation of the cost comparison and the clinical equivalence basis for the change.
Manufacturer Switching
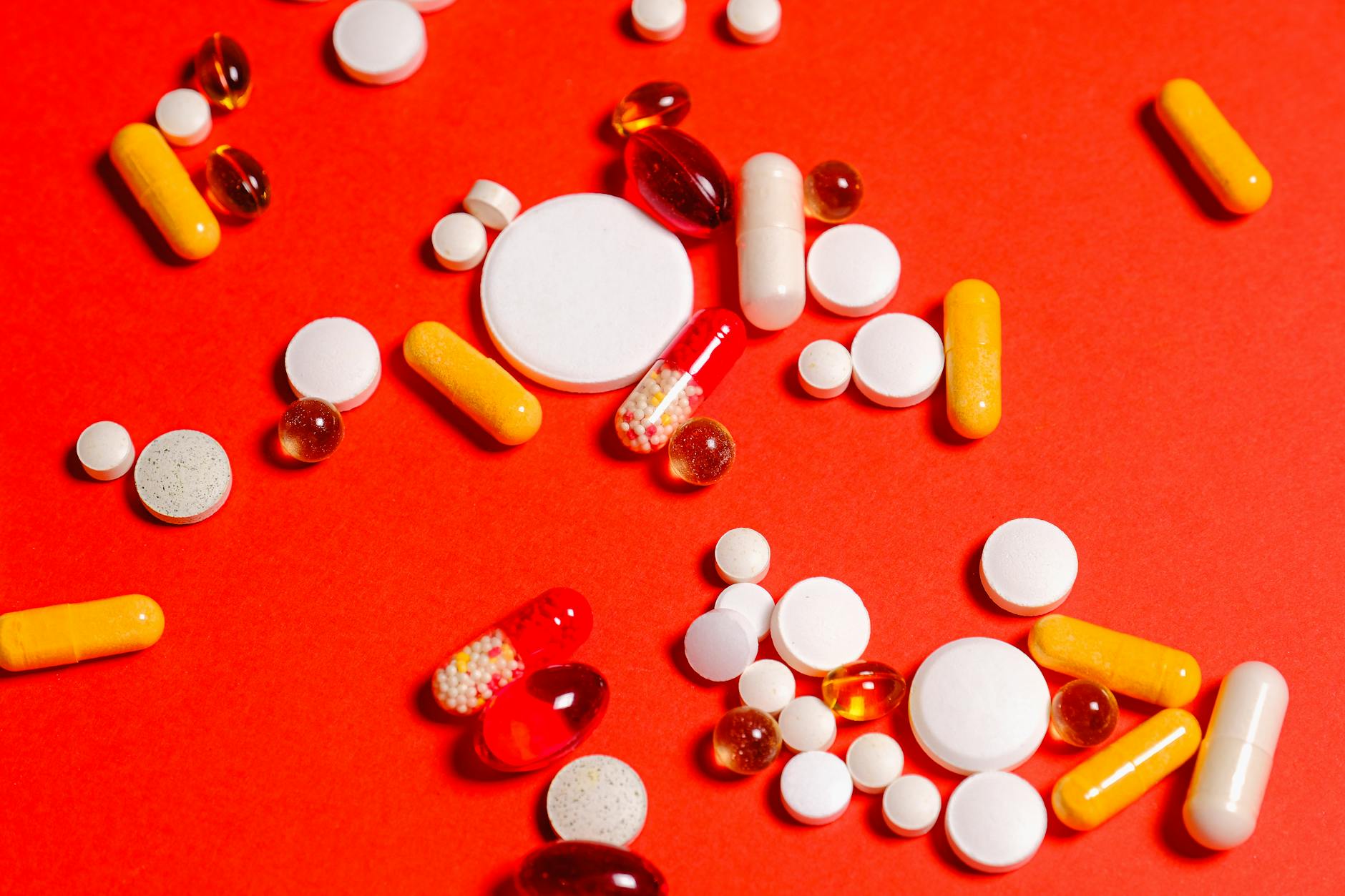
When a pharmacy’s wholesaler relationship changes or when supply chain disruptions affect one manufacturer’s version of a generic medication the dispensing pharmacy may switch to a generic produced by a different manufacturer that uses different inactive ingredients, different tablet coatings, and potentially different release characteristics while containing the same active compound. All approved generics for a given active ingredient are theoretically interchangeable under regulatory equivalence standards but patients who are sensitive to excipients or who have noticed response differences between manufacturers have legitimate clinical grounds for requesting consistency in their supply source. Pharmacy staff are not always proactive about informing patients when the manufacturer of their generic medication has changed because the substitution is considered clinically equivalent under standard dispensing practice. Patients who notice a change in the appearance, taste, or physical characteristics of their medication from one refill to the next and want to understand the cause should ask specifically whether the manufacturing source has changed.
Split Tablet Dispensing
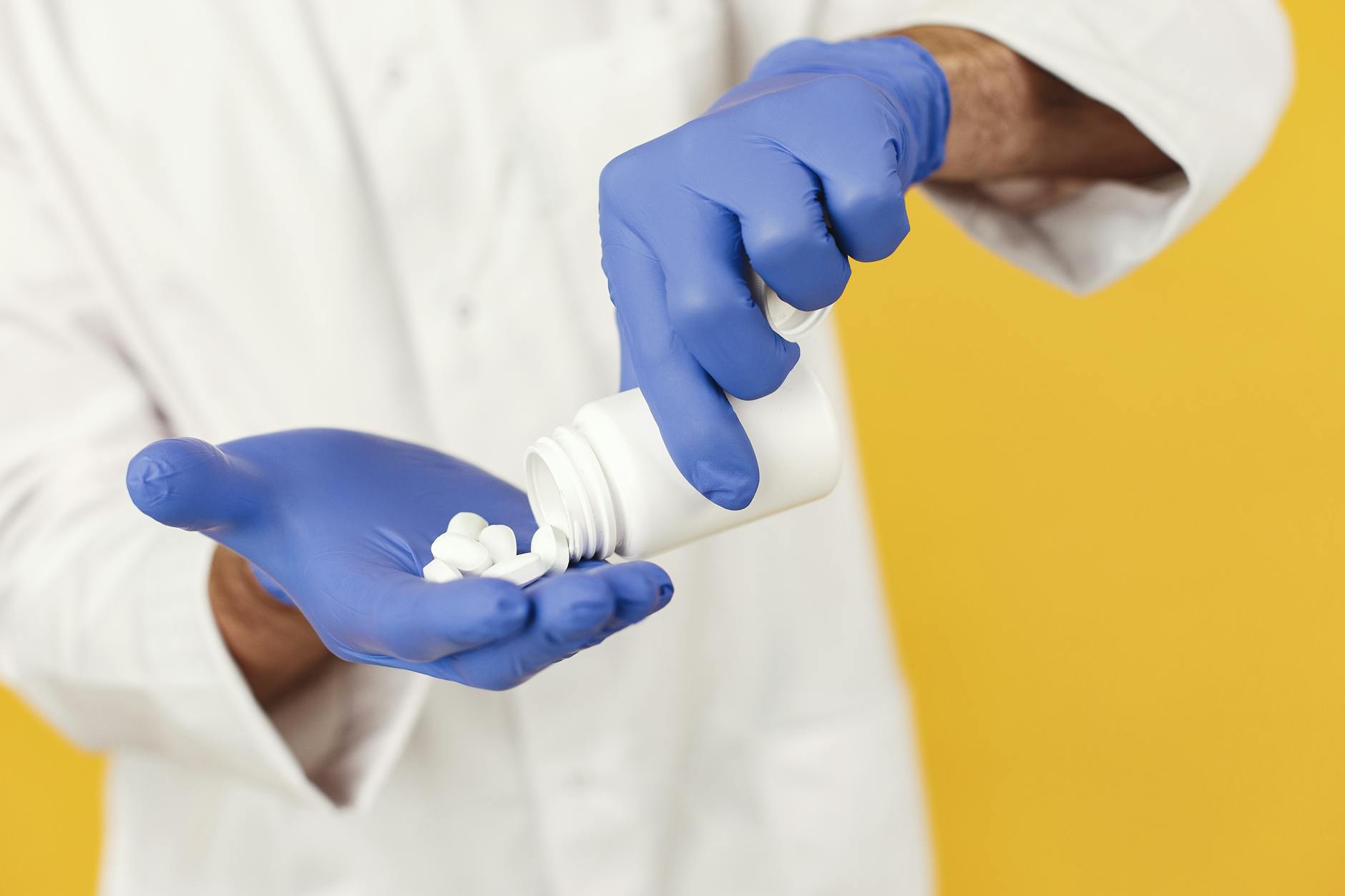
Pharmacists and prescribing physicians sometimes collaborate to dispense a higher dosage tablet with instructions for the patient to split each tablet to achieve the prescribed dose, a practice that can reduce medication costs significantly when higher dosage tablets are priced only modestly above lower dosage versions of the same medication. This tablet splitting approach is mathematically straightforward and can halve the effective cost of certain medications but it requires that the specific tablet is physically and pharmacologically suitable for splitting which not all medications are. Extended-release formulations, enteric-coated tablets, and capsules cannot be split without compromising their release mechanism and any splitting recommendation should be explicitly confirmed as appropriate for the specific formulation being dispensed. Patients who are offered split-tablet dispensing should ask the pharmacist to confirm in specific terms that their medication format is safe and effective when divided before implementing the cost-saving approach.
Dosage Form Switching

A prescription written for one physical form of a medication such as a capsule may be filled with a tablet formulation of the same active ingredient at the same dose if the capsule version is unavailable, significantly more expensive, or not covered under the patient’s insurance while the tablet version is accessible. Dosage form switches within the same active ingredient and dose are generally considered clinically equivalent for most medications but the absorption characteristics of tablets and capsules can differ in ways that are relevant for certain drugs and certain patient populations. Patients with swallowing difficulties, specific absorption considerations, or documented responses to one formulation over another have clinical grounds to request consistency in their dispensing format. The substitution of one dosage form for another is typically handled at the pharmacy level without automatic physician notification and patients who want their doctor involved in this decision should request it explicitly.
Extended Supply Dispensing

Pharmacy benefit programs and mail-order dispensing services frequently encourage or automatically implement a switch from monthly thirty-day supplies to quarterly ninety-day supplies for maintenance medications, a change that reduces dispensing fees, changes the dispensing location, and may alter the manufacturer source of the medication received. The transition from retail monthly dispensing to mail-order quarterly dispensing is presented as a cost-saving convenience but represents a meaningful change in the patient’s relationship with their medication supply that includes reduced pharmacist contact and a different physical handling chain for the product. Insurance plans that impose cost penalties on retail dispensing of maintenance medications after a specified number of fills are effectively mandating a channel substitution that patients may not fully understand when they first encounter the pricing difference. Patients who prefer to maintain a relationship with a local pharmacist for their maintenance medications should understand their plan’s dispensing channel rules before their first fill to avoid being surprised by cost differentials on subsequent refills.
Compound Substitution
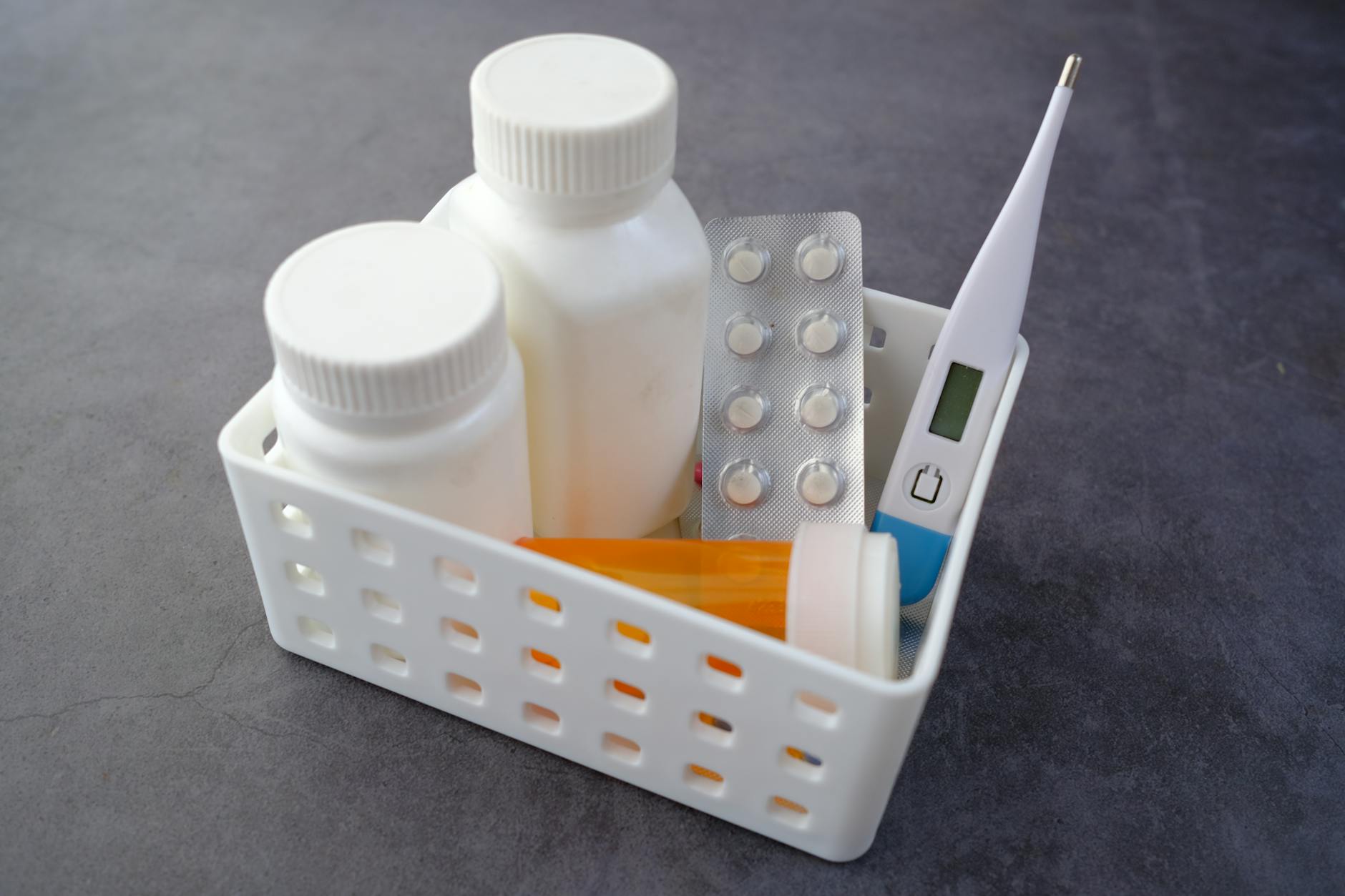
When a commercially manufactured medication is unavailable due to shortage, discontinuation, or supply disruption a compounding pharmacy can prepare a custom version of the same active ingredient to the prescribed dose specification, substituting a compounded preparation for the commercial product the physician originally intended. Compounded medications are prepared individually rather than manufactured at scale and while they contain the same active pharmaceutical ingredient they are not subject to the same regulatory review and quality assurance infrastructure as commercially manufactured products. The clinical implications of switching from a commercial to a compounded preparation are not trivial for all medications and patients who are moved to compounded versions of their regular medications during shortage periods should understand that they are receiving a different product class rather than simply a different brand. Pharmacies that offer compounding as a substitution solution during shortage periods are required to disclose the compounded nature of the dispensed preparation but are not always proactive about explaining the regulatory distinction between compounded and commercially manufactured products.
Biosimilar Substitution

Biologic medications derived from living cell systems have a specific category of approved substitute called a biosimilar which is not chemically identical to the reference product in the way a small-molecule generic is identical to its brand equivalent but is demonstrated to have no clinically meaningful differences in safety and effectiveness. Regulatory approval of biosimilars includes interchangeability designations that in many jurisdictions permit automatic pharmacy substitution without requiring a new prescription from the physician, a relatively recent regulatory development that patients taking biologic medications should be aware of. The financial implications of biosimilar substitution can be significant because biologic medications are among the most expensive in any formulary and biosimilar alternatives often represent substantial cost reductions. Patients taking biologic medications for conditions including inflammatory diseases, diabetes, and certain cancers should ask their pharmacist and physician specifically about the biosimilar substitution policies that apply to their specific product under their current insurance arrangement.
Over-the-Counter Redirection

Pharmacists who identify that a prescribed medication has a direct over-the-counter equivalent at the same active ingredient and dose may suggest or facilitate a switch to the non-prescription version particularly when the patient’s insurance does not cover the prescription version or when the out-of-pocket cost of the prescribed version exceeds the retail price of the over-the-counter equivalent. Medications that exist in both prescription and over-the-counter formulations at different dosage levels create a specific opportunity for this redirection when the prescribed dose matches what is available without prescription. This form of substitution places the purchase outside the insurance claim system entirely and while it can save money it also removes the prescription record and the pharmacist verification step that the insurance dispensing process includes. Patients who are redirected to over-the-counter alternatives for medications they expected to receive by prescription should confirm that the active ingredient, dosage, and formulation are equivalent to what their physician prescribed before accepting the substitution.
Pill Pack Reformatting
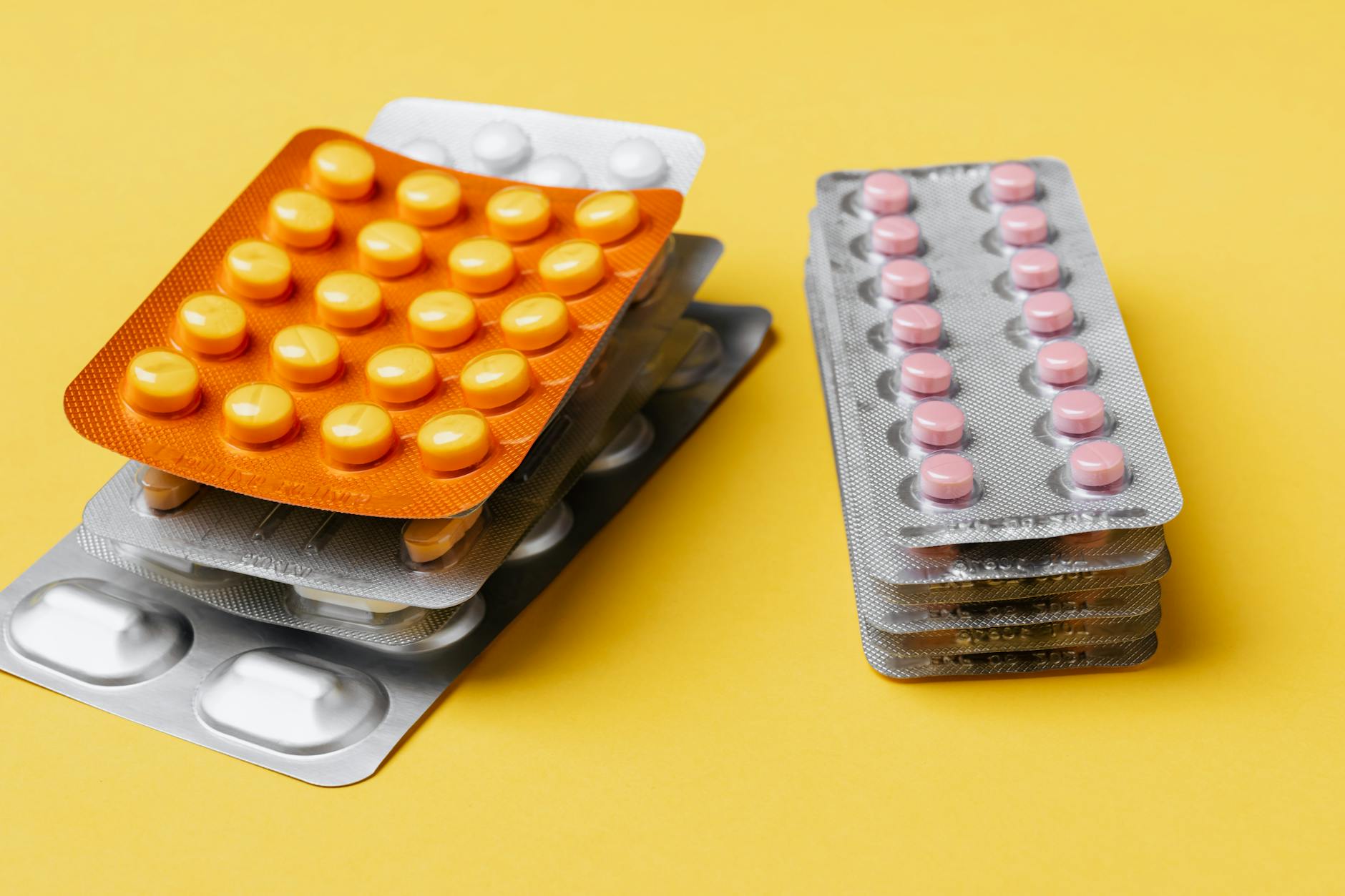
Medication synchronization programs that consolidate multiple prescriptions into blister pack or pouch dispensing formats may substitute certain medications for alternatives that are compatible with automated packaging systems when the originally prescribed version cannot be processed by the dispensing machinery. The operational requirements of automated blister pack systems create specific constraints around tablet and capsule dimensions, fragility, and coating characteristics that exclude certain medication formats from the synchronized dispensing program. Patients who enroll in medication synchronization services to improve adherence through simplified packaging should ask specifically whether any of their current medications will be substituted as a consequence of the format requirements of the dispensing system. The adherence benefits of synchronized packaging programs are well-documented but they should be understood as potentially involving secondary substitutions beyond the primary consolidation service being offered.
Prior Authorization Bypass
When a prescribed medication requires prior authorization from the insurance company before it will be covered the pharmacy may initiate a substitution to a formulary-preferred alternative that does not require prior authorization as a way of providing immediate medication access while the authorization process for the original prescription proceeds in the background. This bypass approach is frequently in the patient’s practical interest because prior authorization processes can take days or weeks during which the patient is without their prescribed medication. The substitution made during the authorization gap may or may not be discontinued when authorization for the original prescription is eventually approved depending on the clinical outcome during the trial period. Patients who receive a substitute during a prior authorization process should ask explicitly whether they will be automatically returned to their originally prescribed medication when authorization is granted or whether active steps are required to reinitiate the original prescription.
Sample Pack Bridging

Physician office samples provided by pharmaceutical manufacturers create an opportunity for pharmacists and physicians working in coordinated care settings to bridge a patient onto a different medication than originally prescribed when samples of the prescribed product are unavailable but samples of a therapeutically similar alternative are on hand. Sample-based medication bridging is common in specialist practices managing expensive medications and while it serves the immediate goal of initiating treatment it can create downstream dispensing patterns that favor the sampled product over the originally prescribed one. The relationship between sample availability and subsequent prescribing patterns is a documented feature of pharmaceutical marketing strategy and patients who receive samples as a starting point for long-term medication should ask their physician whether the sampled product was selected on pure clinical grounds. Understanding whether a sample-initiated prescription reflects the physician’s independent clinical preference or a sample availability convenience is information that patients are entitled to request.
Quantity Limit Adjustment

Insurance plans impose quantity limits on many medications that specify the maximum units dispensable within a defined period and when a prescription exceeds these limits the pharmacy may dispense an adjusted quantity accompanied by a reformulation of the dosing instructions rather than pursuing an override authorization. The practical effect of quantity limit adjustment is that the patient receives a different amount of medication than prescribed and may be instructed to take it differently to stretch the supply to the coverage boundary. Patients whose conditions require dosing at levels that regularly exceed insurance quantity limits should work with their physician to pursue formal limit override authorization rather than accepting repeated quantity adjustments that may not provide adequate therapeutic coverage. The quantity limit adjustment process at the pharmacy level is a compliance response to insurance constraints rather than a clinical judgment and should not be confused with a physician-directed dosing change.
Store Brand Nutraceuticals

Pharmacies that dispense prescribed nutritional supplements, vitamins, and nutraceuticals may substitute their own store-brand versions for name-brand products specified in the prescription when both contain the stated active nutrient at the same dose and the generic substitution regulations in the jurisdiction extend to supplement-format products. The quality consistency of nutraceutical manufacturing is regulated less stringently than pharmaceutical manufacturing and the equivalence of store-brand supplements to name-brand versions is less rigorously demonstrated than the equivalence required for pharmaceutical generic approval. Patients who have been prescribed specific branded supplement formulations by physicians who have clinical reasons for preferring particular products should discuss the substitution implications with both the dispensing pharmacist and the prescribing physician before accepting a store-brand alternative. The price differential between branded and store-brand nutraceuticals can be significant but the lesser regulatory oversight of supplement manufacturing means that brand consistency carries more potential clinical significance in this category than in standard pharmaceutical generics.
Delivery Format Substitution

Medications available in both standard and specialty delivery formats such as auto-injector versus vial-and-syringe configurations for injectable drugs may be substituted between formats when one delivery system is unavailable or when the insurance plan covers one format but not the other. The clinical content of the medication is identical between formats but the usability implications for patients who self-administer are significant because auto-injector and manual injection techniques require different training, different storage considerations, and create different adherence experiences. Patients who are switched between delivery formats for injectable medications should receive specific training on the substitute format before leaving the pharmacy and should not assume that proficiency with one injection system transfers automatically to a different mechanical design. The substitution of delivery format for an injectable medication should trigger a pharmacist consultation rather than a simple bag handover and patients who do not receive this proactively should request it.
Specialty Pharmacy Redirection

Insurance plans that designate specific specialty pharmacies as the exclusive or preferred dispensing channel for high-cost medications create a mandatory substitution of dispensing source that transfers the patient from their established retail pharmacy relationship to a mail-order or specialty facility they have not previously used. The clinical content of the medication received through a specialty pharmacy channel is not changed by the redirection but the pharmacist relationship, communication format, and monitoring infrastructure are all substantially different from a retail dispensing environment. Patients managing complex conditions with specialty medications who are redirected to specialty pharmacy channels should establish a proactive communication relationship with the new dispensing pharmacist rather than treating the specialty pharmacy as a simple fulfillment service. The clinical support services offered by specialty pharmacies for complex medications are often more comprehensive than retail pharmacy equivalents but they require patient engagement to access and do not operate automatically in the absence of patient-initiated contact.
Therapeutic Duplication Elimination
Pharmacists who perform medication reconciliation during dispensing may identify therapeutic duplication where a patient is receiving two medications from the same class prescribed by different physicians and may initiate a substitution that eliminates one in favor of a single agent rather than dispensing both as prescribed. This intervention is clinically appropriate when genuine duplication creates safety risk but the pharmacist’s determination of therapeutic duplication requires access to complete prescribing history that may not always be fully available in the dispensing record. Patients who are told that one of their medications is being withheld or substituted due to therapeutic duplication should ask the pharmacist to initiate direct communication with all relevant prescribing physicians before the change is implemented rather than accepting the pharmacist’s unilateral assessment. The therapeutic duplication elimination process at the pharmacy level is a safety intervention but it intersects with clinical judgment that appropriately involves the prescribing physicians.
Cash Pay Substitution

Patients who present prescriptions without insurance coverage or who choose to pay out of pocket may be offered a cash-pay substitution to a generic or alternative formulation that qualifies for significant discount program pricing through platforms that operate outside the insurance billing system. Discount programs available through pharmacy benefit platforms can make certain generic medications dramatically less expensive than their insurance copay equivalent creating genuine financial benefit for patients who understand and utilize them. The cash-pay substitution pathway operates entirely outside insurance claim processing which means it does not contribute to deductible accumulation and does not appear in insurance medication records in the same way that insurance-billed dispensing does. Patients managing medications across multiple prescribers and insurance plans should be aware that cash-pay dispensing creates a documentation gap in their insurance medication history that could affect continuity of care if prescribers rely on insurance records for medication reconciliation.
Inactive Ingredient Variation

Generic medications from different manufacturers are permitted to use entirely different inactive ingredients including fillers, binders, colorants, and coating materials while containing the same active pharmaceutical compound and all approved generics for a given active ingredient are legally interchangeable under standard dispensing practice regardless of their inactive ingredient composition. Patients with documented allergies or intolerances to specific inactive ingredients such as lactose, gluten-containing starches, certain dyes, or particular preservatives may receive a generic substitution that contains their problematic excipient even when the brand-name version they previously used did not. Pharmacists have access to inactive ingredient databases that can be used to screen substitutions for known excipient sensitivities but this screening does not happen automatically and requires a patient-initiated conversation about their specific sensitivities before the dispensing decision is made. Patients with known inactive ingredient sensitivities should proactively inform their pharmacist of these at the time of each new prescription fill and specifically ask for confirmation that the dispensed product does not contain the problematic component.
Refill Timing Optimization
Pharmacy management systems that monitor refill patterns may implement automatic early refill processing that shifts a patient’s dispensing cycle in ways that change the calendar timing of their medication supply and potentially the specific lot number and manufacturing batch of the product they receive. Lot number and manufacturing batch variations within a single approved generic product can represent minor formulation differences that are within regulatory tolerance but that sensitive patients may notice as subtle changes in their medication experience. The refill timing optimization process is designed to improve adherence through supply continuity but its implementation is largely invisible to patients who interact only with the dispensing counter rather than the dispensing system behind it. Patients who want to maintain consistency in their medication supply source and batch history should establish a relationship with a specific pharmacist rather than treating their pharmacy as an interchangeable fulfillment service and should ask about lot consistency when refilling critical medications.
Combination Product Splitting
A prescribed fixed-dose combination medication that packages two active ingredients in a single tablet may be substituted with the two component medications dispensed separately when the combination product is unavailable, not covered, or significantly more expensive than the individual components. The clinical outcome of receiving two separate tablets that together provide the same active ingredients as a single combination tablet is theoretically equivalent but the practical adherence implications are meaningful because separate dispensing introduces an additional daily pill and an additional source of potential confusion about the medication regimen. Patients who are switched from combination products to separate component dispensing should receive explicit written instructions about how the two medications relate to their previous single-tablet regimen and should confirm with their pharmacist that the combined dose of the separate products matches the combination product they were previously taking.
Patient Assistance Substitution

Pharmacists with knowledge of manufacturer patient assistance programs may redirect patients who cannot afford their prescribed medication toward a program that provides a different product from the same manufacturer or therapeutic class rather than the specific medication originally prescribed. Patient assistance programs are administered by individual manufacturers for their own product portfolios and the medication available through a given program is determined by the manufacturer’s portfolio rather than by the prescribing physician’s clinical preference. Patients who are redirected to manufacturer assistance programs should understand that the available product is determined by program eligibility and manufacturer portfolio rather than representing an independent clinical recommendation from either the pharmacist or the prescribing physician. The financial benefit of manufacturer assistance programs can be transformative for patients who qualify but the clinical implications of receiving a program-determined alternative rather than the originally prescribed medication warrant a confirming conversation with the prescribing physician before the substitution is accepted.
Share your own experiences with pharmacy substitutions and the questions you wish you had asked at the counter in the comments.





