The human body is remarkably communicative, sending out subtle and not-so-subtle warnings long before a food intolerance becomes fully established. Many people dismiss these early signals as stress, aging, or unrelated health issues, allowing the underlying sensitivity to go unaddressed for months or even years. Food intolerances differ from allergies in that they develop gradually and often produce a confusing constellation of symptoms that span multiple body systems. Recognizing the patterns early can lead to meaningful improvements in daily comfort, energy, and long-term digestive health. Here are 27 surprising signals your body may be sending when a food intolerance is quietly taking hold.
Brain Fog

A noticeable decline in mental clarity after eating is one of the most commonly overlooked indicators of a developing food intolerance. The connection between gut health and brain function is well established in scientific literature, with the gut-brain axis playing a central role in cognitive performance. Inflammatory responses triggered by problem foods can temporarily impair focus, memory retrieval, and processing speed. Many people attribute this haziness to poor sleep or work stress without considering a dietary link. Tracking mental clarity in relation to meals is a useful first step toward identifying a pattern.
Chronic Bloating

Persistent abdominal bloating that appears regularly after meals is a hallmark early signal of digestive sensitivity. Unlike occasional gas related to overeating, intolerance-related bloating tends to follow a consistent pattern tied to specific foods or food groups. The digestive system struggles to break down certain compounds, leading to fermentation in the gut and the production of excess gas. This bloating often occurs within thirty minutes to two hours of eating and may feel disproportionate to the amount consumed. Keeping a detailed food and symptom diary can help reveal which ingredients are responsible.
Skin Rashes

Unexplained skin reactions including hives, eczema flares, and general redness can be directly connected to food intolerances developing in the digestive system. The skin and the gut are deeply interconnected through immune system pathways, meaning internal inflammation often manifests externally. These reactions may appear on the face, arms, or torso and tend to be cyclical rather than constant. Many individuals spend considerable time and money on topical treatments without investigating a potential dietary trigger. Eliminating suspected foods temporarily and monitoring skin changes is a widely recommended investigative approach.
Fatigue After Eating

Feeling unusually tired or heavy after meals goes beyond the normal post-meal energy dip that most people experience. When the body is working harder than usual to process a problematic food, significant energy is diverted toward managing the inflammatory or digestive response. This kind of fatigue is typically disproportionate to the size of the meal and tends to recur with specific food types. It can interfere with afternoon productivity and is often mistaken for low iron levels or poor sleep quality. Noticing which meals consistently produce this response is a valuable diagnostic observation.
Joint Pain

Aching or stiffness in the joints following meals is a less intuitive symptom of food intolerance but one that is increasingly recognized in clinical practice. Certain foods can trigger systemic inflammation that settles into the joints, particularly in individuals with existing sensitivities. This pain is often reported in the fingers, knees, and lower back and may appear several hours after eating rather than immediately. People managing conditions like arthritis sometimes find that dietary adjustments significantly reduce joint discomfort. The delayed nature of this symptom makes it particularly difficult to connect to specific food consumption without careful tracking.
Mood Swings

Noticeable shifts in emotional state following meals can indicate that the gut microbiome is being disrupted by a food the body cannot tolerate well. The gut produces a significant proportion of the body’s serotonin, meaning digestive disturbances can directly affect mood regulation. Irritability, anxiety, and low mood appearing in the hours after eating are worth noting as potential intolerance signals. These emotional fluctuations are frequently attributed entirely to psychological causes without any dietary investigation. Examining the relationship between food consumption and emotional patterns can reveal unexpected connections.
Nasal Congestion

A stuffy or runny nose that appears consistently after eating is a recognized symptom of certain food intolerances, particularly those involving dairy or histamine-rich foods. This response is sometimes called gustatory rhinitis and involves an inflammatory reaction in the nasal passages triggered by food compounds. Many people assume this congestion is allergy-related or seasonal without ever connecting it to their diet. The symptom typically appears within an hour of eating and resolves on its own but recurs reliably with the offending food. Noting whether congestion correlates with specific meals can help narrow down the likely culprit.
Heart Palpitations

Experiencing a racing or irregular heartbeat after eating can occasionally be linked to food intolerance rather than a cardiovascular issue. Certain food compounds including histamines, sulfites, and artificial additives are known to trigger this response in sensitive individuals. The palpitations are typically short-lived but can be alarming enough to prompt unnecessary cardiac investigations. Doctors increasingly recognize that ruling out dietary triggers is a valuable step before pursuing more extensive cardiac testing. Recording when palpitations occur in relation to meals provides useful information for healthcare providers.
Mouth Ulcers

Recurring sores inside the mouth that appear without an obvious cause are sometimes connected to developing sensitivities to gluten or other food proteins. The immune response triggered by these foods can manifest in the soft tissues of the mouth as a visible inflammatory reaction. These ulcers tend to be small, painful, and recurrent rather than isolated incidents. Individuals who experience frequent mouth sores alongside digestive discomfort may benefit from exploring a potential dietary connection. A healthcare provider can help determine whether an elimination protocol is appropriate.
Dark Under-Eye Circles

Persistent dark circles beneath the eyes that are not explained by sleep deprivation are sometimes referred to as allergic shiners and can indicate chronic low-level inflammation linked to food intolerance. The inflammation causes blood to pool in the small vessels beneath the thin skin under the eyes, creating a shadowed appearance. This signal is more commonly discussed in the context of environmental allergies but dietary triggers are also recognized as a contributing factor. Improving gut health through dietary adjustments has been reported to reduce this discoloration in some individuals. Consulting a nutritionist or allergist can help explore this connection further.
Headaches

Recurring headaches that appear after meals or at consistent times of day are worth examining through a dietary lens. Certain food compounds including tyramine, nitrates, MSG, and histamines are well-documented headache triggers in sensitive individuals. Unlike migraine disorders driven purely by neurological factors, food intolerance headaches tend to follow a predictable dietary pattern. Individuals who experience frequent headaches without a clear neurological cause are increasingly being advised to explore elimination diets. Identifying and removing the offending food can produce a significant reduction in headache frequency.
Insomnia

Difficulty falling or staying asleep can be connected to food intolerances through the disruption of gut-produced neurotransmitters that regulate sleep cycles. Foods that trigger an inflammatory response can elevate cortisol and disrupt melatonin production, making restful sleep harder to achieve. This symptom is particularly puzzling because the connection between a meal earlier in the day and poor sleep several hours later is not intuitive. Many individuals invest in sleep aids or behavioral interventions without considering that a dietary adjustment might be more effective. Tracking both food intake and sleep quality together can reveal meaningful correlations.
Excessive Thirst

Feeling unusually thirsty after specific meals or throughout the day without a clear cause can be a sign that the body is managing an inflammatory response driven by food sensitivity. Inflammation requires increased fluid to support cellular repair and immune function, which the body signals through thirst. This symptom is particularly associated with intolerances to high-sodium processed foods and certain food additives. It is frequently misinterpreted as a general hydration issue rather than a food-specific response. Paying attention to whether thirst spikes after particular types of meals adds a useful layer of observation.
Nausea
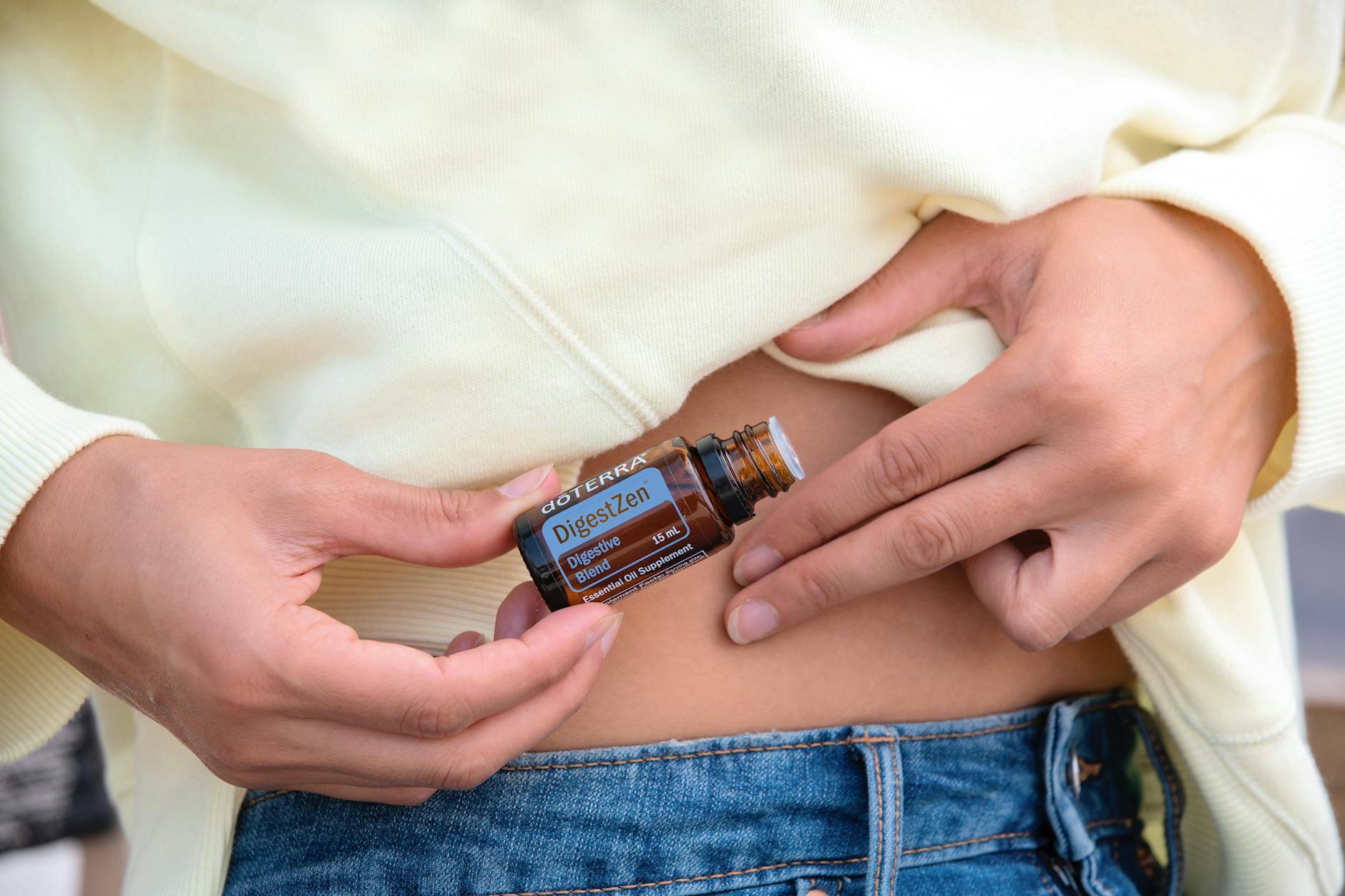
Mild but recurring nausea in the hours following a meal is a signal that the digestive system is under stress from a food it struggles to process. This nausea is typically not severe enough to indicate food poisoning but is persistent and reproducible with the same food. It often appears alongside other digestive symptoms like bloating or cramping, forming part of a broader pattern of intolerance. Many people normalize this feeling over time, assuming it is simply how their body responds to eating. Recognizing it as a potential warning sign is an important step toward investigating the underlying cause.
Hair Thinning

Gradual hair thinning or increased shedding can be an unexpected downstream effect of a developing food intolerance. When the gut is consistently inflamed, the absorption of key nutrients including iron, zinc, and biotin is compromised, and hair follicles are among the first structures to feel the impact. This symptom typically develops slowly and is therefore rarely connected to diet without professional guidance. Individuals experiencing hair changes alongside digestive symptoms may benefit from investigating whether nutrient malabsorption linked to intolerance is a contributing factor. Addressing the underlying intolerance often supports improvement in hair health over time.
Muscle Cramps

Recurring muscle cramps that occur without excessive physical exertion can be linked to the malabsorption of key minerals caused by gut inflammation associated with food intolerance. Magnesium, calcium, and potassium are particularly vulnerable to poor absorption in an inflamed digestive environment. These cramps often appear in the legs, feet, and hands and tend to be dismissed as dehydration or overexertion. When dietary changes lead to improvements in gut health, mineral absorption often normalizes and cramping frequency decreases. A healthcare provider can test for mineral deficiencies to help determine whether gut-related malabsorption is involved.
Itchy Ears

An itching sensation deep inside the ears after eating certain foods is a lesser-known but recognized symptom of food sensitivity. The mucous membranes of the ear canal are connected to the same immune pathways that respond to food intolerances, particularly those involving oral allergy syndrome. This symptom is more commonly reported in connection with intolerances to certain fruits, nuts, and raw vegetables. It tends to be transient, resolving within an hour, which makes it easy to dismiss. Noting whether the sensation occurs consistently after specific foods can help pinpoint the trigger.
Reflux

Acid reflux or heartburn that appears frequently and does not respond well to standard antacid treatment may indicate that a food intolerance is contributing to lower esophageal sphincter dysfunction. Certain foods that trigger sensitivity can increase gastric acid production or affect the muscular valve that prevents stomach acid from rising. This symptom is extremely common and therefore frequently treated in isolation without exploring potential dietary intolerances as an underlying driver. Research suggests that eliminating trigger foods can produce more sustained relief than medication alone in intolerance-related cases. Working with a gastroenterologist to investigate dietary contributors is a productive approach.
Acne Breakouts
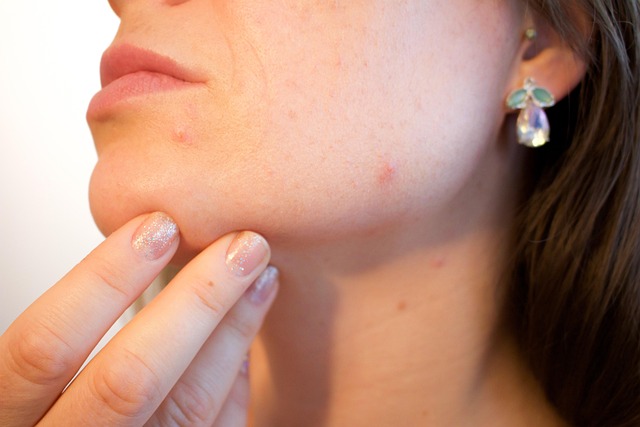
Persistent acne in adults that does not respond to topical treatments or standard skincare adjustments may be connected to systemic inflammation driven by food intolerance. The relationship between diet and skin health is well documented, with dairy and high-glycemic foods among the most studied triggers. Intolerance-driven inflammation affects hormone regulation and sebum production, creating conditions that contribute to breakouts. Adults who have managed acne for years without resolution are increasingly being directed toward dietary investigation as part of a holistic treatment approach. Eliminating suspected foods for four to six weeks and monitoring skin changes is a commonly recommended protocol.
Anxiety Spikes

Heightened feelings of anxiety or nervousness that appear after eating and are not explained by psychological stressors may reflect the gut-brain axis responding to a food the body cannot tolerate. Inflammatory compounds released during an intolerance response can cross into the nervous system and elevate stress hormones. This connection is particularly pronounced in individuals with sensitivities to gluten, dairy, or high-histamine foods. The symptom is challenging to attribute to diet because anxiety has so many potential causes. Keeping a mood and food journal with timestamps can help identify whether a dietary pattern is contributing.
Frequent Yawning

Excessive yawning after meals beyond what is explained by tiredness can indicate that blood oxygen regulation is being affected by a food-related inflammatory response. Some researchers connect post-meal yawning to the body’s attempt to regulate internal temperature and neural activity during a digestive stress response. This symptom is subtle enough that most people never consider it as a potential signal worth investigating. When it appears consistently after specific foods alongside other intolerance symptoms, it adds to a broader pattern worth discussing with a healthcare provider. Tracking frequency and timing in relation to meals is a low-effort first step.
Swollen Lips

Mild swelling or a tingling sensation in the lips after eating certain foods can indicate an early-stage sensitivity that has not yet escalated to a more pronounced allergic response. This symptom is frequently observed with intolerances to certain raw fruits, vegetables, and food additives containing sulfites or preservatives. Unlike anaphylactic reactions, intolerance-related lip swelling is mild and resolves relatively quickly. It is still worth taking seriously as a signal that the immune system is reacting to a food compound in a way that may intensify over time. A healthcare provider or allergist should be consulted if this symptom occurs repeatedly.
Irregular Bowel Movements

Changes in bowel regularity including alternating constipation and diarrhea without a diagnosed condition are among the clearest digestive signals of a developing food intolerance. The gut motility system is highly sensitive to inflammatory triggers, and problem foods can either accelerate or slow transit time unpredictably. This irregularity is often mistaken for irritable bowel syndrome, which itself shares significant overlap with food intolerance presentations. Identifying and removing the offending food frequently produces a rapid and noticeable improvement in bowel regularity. A registered dietitian can provide structured guidance for navigating an elimination and reintroduction protocol.
Brittle Nails

Nails that break, peel, or grow slowly despite adequate hydration can reflect the nutrient malabsorption that accompanies chronic gut inflammation linked to food intolerance. Keratin production depends on a consistent supply of protein, biotin, and silica, all of which are absorbed less efficiently in a compromised digestive environment. This signal develops gradually and is often attributed to environmental factors or cosmetic product use. When brittle nails appear alongside other digestive or systemic symptoms, the possibility of an underlying intolerance is worth exploring. Addressing gut health through dietary adjustments often produces visible improvements in nail strength over several months.
Eye Twitching

Involuntary eye twitching or muscle spasms around the eye area can be connected to magnesium deficiency resulting from poor gut absorption associated with food intolerance. Magnesium plays a critical role in nerve and muscle function, and chronically low levels produce these kinds of involuntary muscular responses. While eye twitching has multiple potential causes including fatigue and caffeine, recurrence alongside other intolerance symptoms adds diagnostic significance. Correcting the underlying gut issue through dietary changes and magnesium replenishment often resolves this symptom. A blood test can confirm whether magnesium levels are below the optimal range.
Body Odor Changes

A noticeable shift in body odor that is not explained by hygiene changes or increased physical activity can reflect changes in gut microbiome composition linked to food intolerance. When certain foods ferment abnormally in the digestive tract, the byproducts can be absorbed into the bloodstream and eventually excreted through the skin. This symptom is one of the most unexpected and least discussed signals of developing intolerance. It tends to appear alongside other digestive complaints and typically improves once the offending food is removed. Discussing this kind of change openly with a healthcare provider can help accelerate the diagnostic process.
Temperature Sensitivity

An increased sensitivity to cold or heat that develops without a thyroid diagnosis may reflect the metabolic disruption caused by chronic low-grade inflammation linked to food intolerance. When the body is consistently managing an immune response, thermoregulation can become less efficient. Individuals may notice they feel cold in environments that others find comfortable or that they overheat easily after specific meals. This symptom is rarely connected to diet without professional guidance because its causes appear entirely unrelated to food. Tracking whether temperature sensitivity correlates with dietary patterns adds a useful dimension to the overall picture.
If any of these signals sound familiar, share your experiences and any dietary discoveries you have made in the comments.





