Navigating the healthcare system requires a level of informed vigilance that many patients are never taught to exercise. Unnecessary surgical procedures are more common than most people realize, driven by a complex mix of financial incentives, institutional pressures, and diagnostic habits that do not always center the patient’s best interest. Recognizing the warning signs that a surgical recommendation may not be in your best interest can protect your health, your finances, and your peace of mind. The following signs are not accusations but tools for awareness, designed to help you ask better questions and make more empowered decisions about your own body.
Second Opinion Avoidance

A physician who responds to your request for a second opinion with resistance, dismissal, or visible frustration is displaying a significant red flag. Confident and ethical surgeons welcome additional perspectives because they understand that informed patients make better surgical candidates. When a doctor frames a second opinion as a waste of time or implies it reflects a lack of trust, that reaction itself warrants scrutiny. Reputable medical institutions actively encourage patients to seek outside consultation before consenting to elective procedures. A doctor who discourages this process may have motivations that do not fully align with your wellbeing.
Rushed Diagnosis
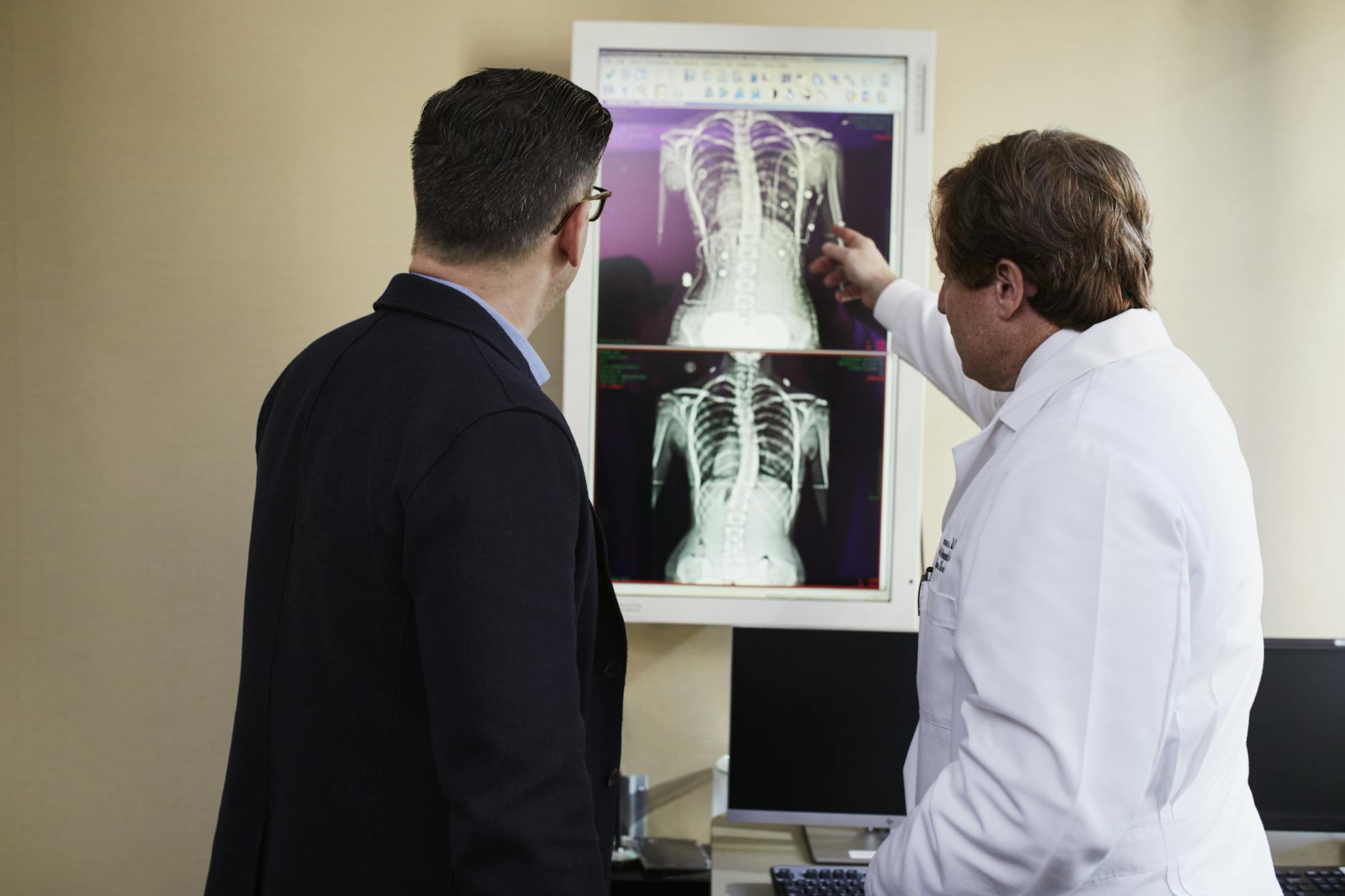
When a surgical recommendation follows an unusually brief examination or a single appointment, the diagnostic process may have been incomplete. Thorough surgical recommendations are typically supported by a comprehensive review of symptoms, medical history, imaging results, and other objective data gathered over time. A physician who arrives at a surgical conclusion without exhausting less invasive diagnostic options may be skipping essential steps. Patients who feel their concerns were not fully heard before a major recommendation was made should treat that feeling as meaningful information. A second opinion from a specialist in the relevant field can provide important clarity.
Vague Diagnosis

Surgery recommended for a condition described in broad or shifting terms rather than a specific, well-documented diagnosis deserves careful scrutiny. Legitimate surgical candidates are typically given a clear diagnosis supported by imaging, lab work, or documented clinical findings that a patient can research and verify. When a physician uses language that is difficult to pin down or changes the framing of the condition across appointments, the clinical picture may not yet justify an invasive intervention. Patients have the right to ask for the specific diagnosis in writing and to understand how it was confirmed. Ambiguity in medical reasoning is not a foundation on which to proceed with surgery.
Non-Surgical Options Ignored

A responsible physician will discuss the full range of treatment options before recommending surgery, including physical therapy, medication, lifestyle modification, and watchful waiting where appropriate. When a doctor moves directly to a surgical recommendation without meaningfully presenting conservative alternatives, it suggests that a less invasive path was not seriously considered. Many conditions that are frequently treated surgically respond well to non-surgical interventions, particularly when caught early and managed carefully. Patients should ask explicitly whether surgery is the only viable option and what the expected outcomes of non-surgical approaches would be. The absence of this conversation is a meaningful omission.
Urgency Without Emergency

Artificial urgency is one of the most commonly reported tactics associated with unnecessary surgical recommendations. When a physician insists a procedure must be scheduled immediately despite the absence of an acute medical emergency, that pressure deserves examination. Many elective and semi-elective surgeries carry no meaningful risk from a brief delay of several weeks, which is typically enough time to gather a second opinion. Conditions that genuinely require emergency surgery are accompanied by clear clinical signs that other providers can independently confirm. Urgency that cannot be explained by objective medical criteria may be motivated by scheduling, financial, or institutional factors rather than patient need.
Financial Incentives

Surgeons who own stakes in surgical centers or who operate within healthcare systems that financially reward high procedure volumes face structural pressures that can influence their clinical recommendations. Research consistently shows that physician ownership of surgical facilities is associated with higher rates of elective procedures. This does not mean that every surgeon in such a system is acting unethically, but patients deserve to understand the economic environment in which their care is being delivered. Asking your physician directly whether they have a financial relationship with the facility where the surgery would be performed is a reasonable and appropriate question. Transparency in this area is both an ethical obligation and a patient right.
Poor Communication

A physician who becomes evasive, dismissive, or impatient when asked detailed questions about a surgical recommendation is not meeting a basic standard of patient-centered care. Patients preparing for surgery are entitled to clear, complete answers about the procedure’s risks, benefits, recovery timeline, success rates, and alternatives. When a doctor deflects these questions or frames them as obstacles rather than legitimate concerns, the therapeutic relationship has broken down in a way that matters. Good surgeons expect and welcome detailed questions because they understand that informed consent is not a formality but a meaningful process. Difficulty getting straight answers is a sign to proceed with significant caution.
Symptom Mismatch

When the severity of a surgical recommendation appears disproportionate to the symptoms a patient is actually experiencing, it is worth pausing to ask whether the intervention matches the clinical reality. Some surgical procedures are commonly recommended for conditions that cause mild or intermittent discomfort rather than significant functional impairment. Patients who feel broadly well but are being told they urgently require surgery should ask how the recommended procedure will improve their daily functioning and quality of life in specific, measurable terms. The threshold for recommending surgery should scale with the severity of the condition and its impact on the patient’s life. A mismatch between symptoms and surgical recommendation is a prompt for deeper inquiry.
Imaging Over-Reliance
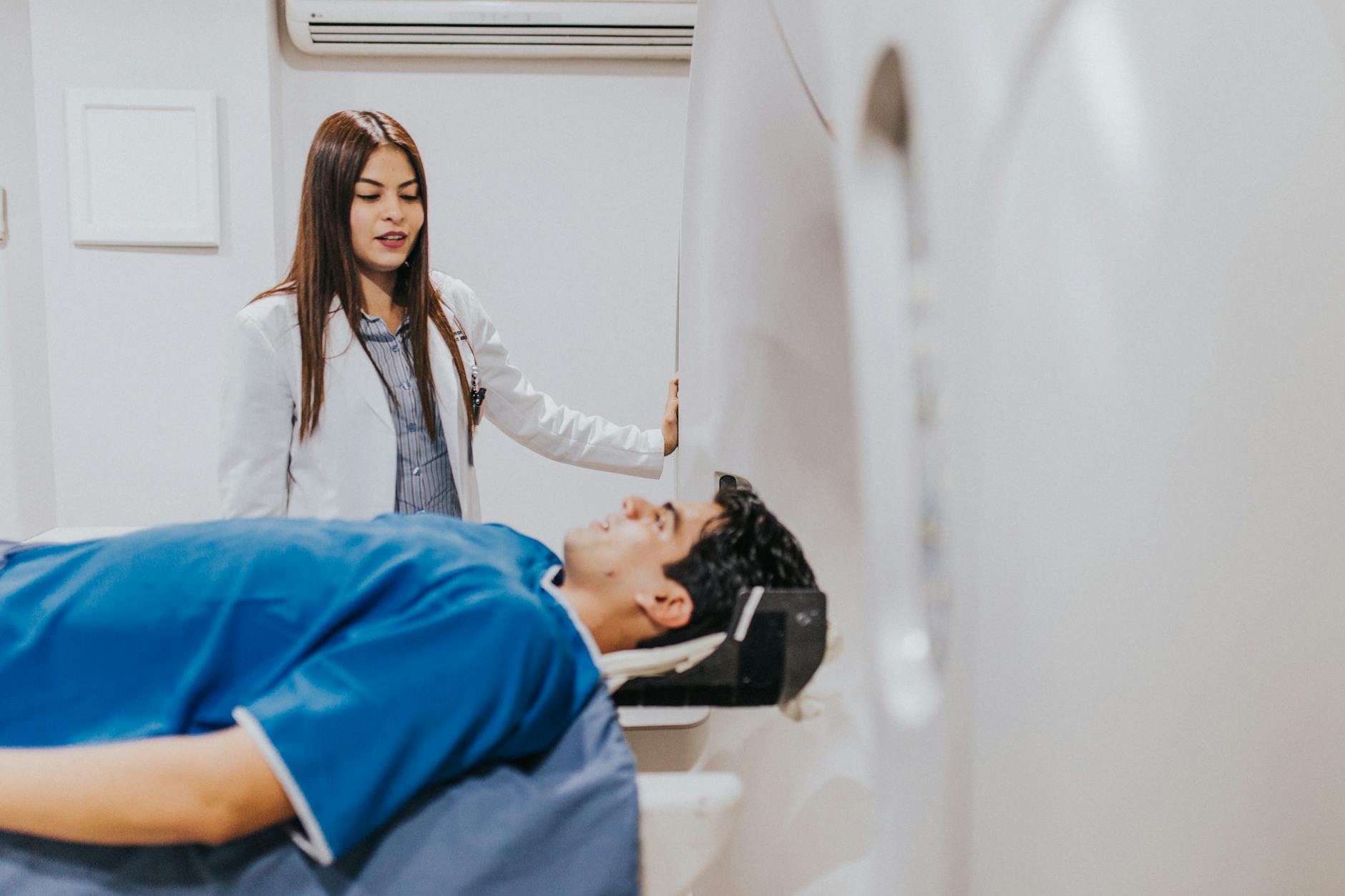
Ordering extensive imaging before a thorough physical examination or clinical history review is a pattern sometimes associated with over-medicalization. Imaging findings such as herniated discs, bone spurs, or minor structural irregularities are extremely common in the general population and frequently cause no symptoms at all. A physician who points to an imaging result as the primary justification for surgery without correlating it to the patient’s actual symptoms may be treating a scan rather than a person. Radiological findings must be interpreted in the context of the patient’s lived experience and clinical presentation. Imaging is a tool to confirm clinical suspicion, not a standalone mandate for surgical intervention.
Specialty Mismatch
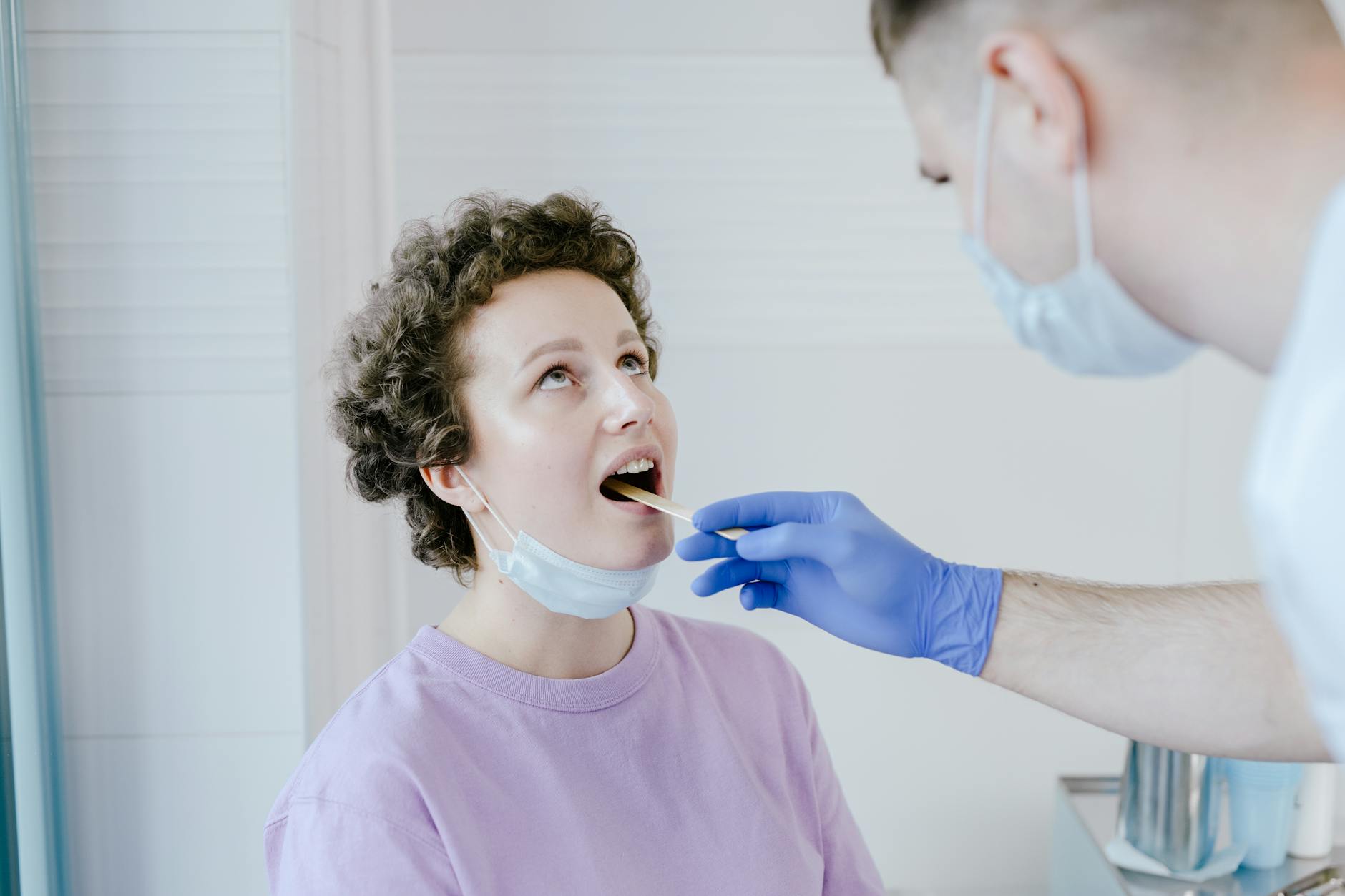
Receiving a surgical recommendation from a physician whose specialty does not precisely align with the condition being treated can be a meaningful warning sign. A general practitioner recommending a complex orthopedic surgery, or a specialist outside the relevant field suggesting an invasive procedure, may not have the depth of expertise to fully evaluate whether surgery is the most appropriate course. Surgical recommendations carry the most weight when they come from a physician who has devoted their training and practice to the specific condition in question. Seeking consultation from a board-certified specialist in the exact area of concern is always appropriate before consenting to a procedure. Expertise specificity matters enormously when the stakes are this high.
Conflicting Test Results

When diagnostic test results are inconsistent with one another or fail to clearly support the stated diagnosis, proceeding with surgery on that basis is premature. Sound surgical decisions rest on a convergence of clinical findings, patient history, and objective diagnostic data that all point in the same direction. A single positive test result in the absence of corroborating evidence is rarely sufficient grounds for an invasive intervention. Patients should ask how each piece of diagnostic information contributes to the overall clinical picture and whether any results contradict the surgical recommendation. Inconsistency in the diagnostic foundation is a reason to gather more information before moving forward.
One-Sided Risk Discussion

A physician who emphasizes the risks of not having surgery while minimizing or avoiding discussion of the risks inherent in the surgical procedure itself is presenting an incomplete picture. Every surgery carries risks including infection, anesthesia complications, blood clots, nerve damage, and the possibility of a poor outcome that leaves the patient worse off than before. Balanced informed consent requires that both the risks of the procedure and the risks of non-intervention be presented honestly and in comparable detail. When a doctor’s risk framing consistently steers toward surgery without acknowledging procedural hazards, the information environment has been shaped in a way that undermines genuine patient autonomy. Patients should specifically ask for the complication rate associated with their proposed procedure.
Dismissive Follow-Up

When a patient raises concerns, reports new symptoms, or questions a surgical plan and the physician responds with brief dismissal rather than genuine engagement, that dynamic is clinically problematic. Follow-up appointments that feel perfunctory or that consistently end with reinforcement of the same surgical recommendation without new information are a sign that the clinical process may have stalled. A physician who listens carefully, revisits the diagnosis in light of new information, and remains open to revising a treatment plan is demonstrating the kind of practice that genuinely serves patient welfare. Dismissiveness is not just an interpersonal failure but a clinical one, since important patient-reported information is being filtered out of the decision-making process. Patients who feel consistently unheard are entitled to seek care elsewhere.
Procedure Frequency
Surgical recommendations for procedures that are known to be performed at unusually high rates in a given region, hospital, or by a specific physician warrant additional scrutiny. Research in health policy has consistently documented wide geographic variation in surgical rates for conditions where clinical evidence does not justify such differences. High-volume surgical practices are not inherently suspect, but when a physician recommends a procedure that is statistically overused in their practice environment, an independent evaluation adds valuable context. Patients can research national and regional benchmarks for the frequency of their proposed procedure and compare them to what they are being told. Pattern-level information is a useful complement to individual clinical judgment.
Informed Consent Gaps

Informed consent is a legal and ethical requirement, not a brief form signed at the door of a procedure room. When a physician fails to clearly explain what the surgery involves, what will happen during recovery, what the realistic success rate is, and what alternatives exist, the consent process has not been completed in any meaningful sense. Patients who feel they were not adequately informed before a procedure are among the most common reporters of unnecessary surgery in medical literature. Every patient has the right to take as much time as they need to review consent materials and to ask questions until they feel genuinely informed. Pressure to sign quickly or an assumption that the patient does not need full details is a warning sign worth acting on.
Recovery Underestimation

A physician who significantly downplays the difficulty, duration, or impact of a surgical recovery may be presenting the procedure as more straightforward than it actually is. Recovery from surgery involves real physical, financial, and emotional costs that must factor into any reasonable cost-benefit analysis. When a doctor describes a complex procedure as a simple fix with minimal downtime in ways that do not align with published clinical data, patients are not receiving accurate information. Asking for written resources about expected recovery timelines and speaking with patients who have undergone the same procedure can provide a more grounded perspective. Accurate recovery information is essential to making a genuinely informed decision.
Symptom Timeline Pressure
A physician who accelerates a surgical recommendation without allowing adequate time to observe whether symptoms resolve, improve, or worsen on their own may be moving faster than the clinical situation requires. Many conditions that initially appear to warrant surgery improve significantly with time and conservative management. Watchful waiting is a legitimate and evidence-based clinical strategy for a wide range of conditions, and its absence from a treatment discussion should prompt questions. The decision to pursue surgery should follow a period of careful monitoring in all but the most urgent cases. A timeline that is driven by scheduling convenience rather than symptom trajectory is worth questioning directly.
Peer Disagreement

When a patient discovers that other physicians within the same specialty would not recommend surgery for the same condition under the same circumstances, that disagreement is clinically meaningful. Medicine involves genuine variation in clinical judgment, but systematic disagreement among specialists about a specific recommendation suggests the evidence base may not clearly support the procedure. Patients who receive a conflicting opinion from a second or third specialist are not obligated to defer to the first physician simply because they were seen first. Comparative consultation is a powerful tool for separating evidence-based recommendations from practice-pattern preferences. The weight of specialist consensus matters when the stakes involve an irreversible physical intervention.
Patient History Gaps
A surgical recommendation made without a thorough review of a patient’s full medical history, including previous surgeries, chronic conditions, medications, and lifestyle factors, is built on an incomplete clinical foundation. Surgical risk profiles are highly individualized, and what may be appropriate for one patient can carry elevated danger for another. Physicians who rely primarily on a presenting complaint without integrating a broader health picture may be operating with insufficient information to make a sound recommendation. Patients should ensure that their complete medical records have been reviewed before any surgical decision is finalized. An incomplete history is not a sufficient basis for an invasive intervention.
Outcome Data Avoidance

A physician who cannot or will not provide specific data about the expected outcomes of a recommended procedure may not have a strong evidentiary foundation for the recommendation. Patients are entitled to ask what percentage of patients who undergo this surgery experience significant improvement, what the complication rate is, and how outcomes compare to non-surgical alternatives. Surgeons who have performed a procedure extensively and are confident in its appropriateness for a given patient will generally be able to provide this information clearly. Evasion or vague reassurances in response to outcome questions suggest either a lack of familiarity with the evidence or an awareness that the evidence is not particularly compelling. Outcome data transparency is a reasonable standard to hold any surgical recommendation to.
Gut Instinct

Patient intuition is a documented and undervalued component of medical decision-making, and research consistently shows that patients who report feeling uncertain or pressured about a surgical recommendation are more likely to later describe the procedure as unnecessary. A persistent sense that something is not quite right about a recommendation, a physician’s manner, or the overall clinical process deserves to be taken seriously rather than dismissed as anxiety. The discomfort patients feel when a major decision is being rushed, oversimplified, or inadequately explained often reflects a genuine gap in the quality of care they are receiving. Listening to that internal signal and using it as a prompt to gather more information is not irrational but deeply practical. Patients who trust their instincts enough to ask harder questions are consistently better protected from avoidable harm.
If any of these signs resonate with your own healthcare experiences, share your thoughts in the comments.





