We live in an era where a two-minute search can convince a perfectly healthy person that they are facing a rare tropical disease or an imminent medical emergency. The doctor’s office has quietly become the place where internet-fueled health anxiety meets clinical reality. Patients arrive clutching printed articles, screenshot galleries, and browser histories full of deeply specific symptom searches. The gap between what the algorithm suggests and what a trained physician actually finds has never been more entertainingly wide.
WebMD Diagnosis

Arriving at an appointment with a printed or screenshot diagnosis from a consumer health website is one of the most recognizable signs of pre-visit internet research. These platforms are designed to cover every possible condition associated with a symptom which inevitably steers readers toward alarming conclusions. Physicians report that a significant portion of their consultation time is now spent walking patients back from worst-case scenarios generated by symptom checkers. The tools themselves carry disclaimers advising users to seek professional advice rather than treat the output as a definitive answer. Doctors generally appreciate the engagement but spend considerable time recalibrating expectations formed before the appointment even begins.
Rare Disease
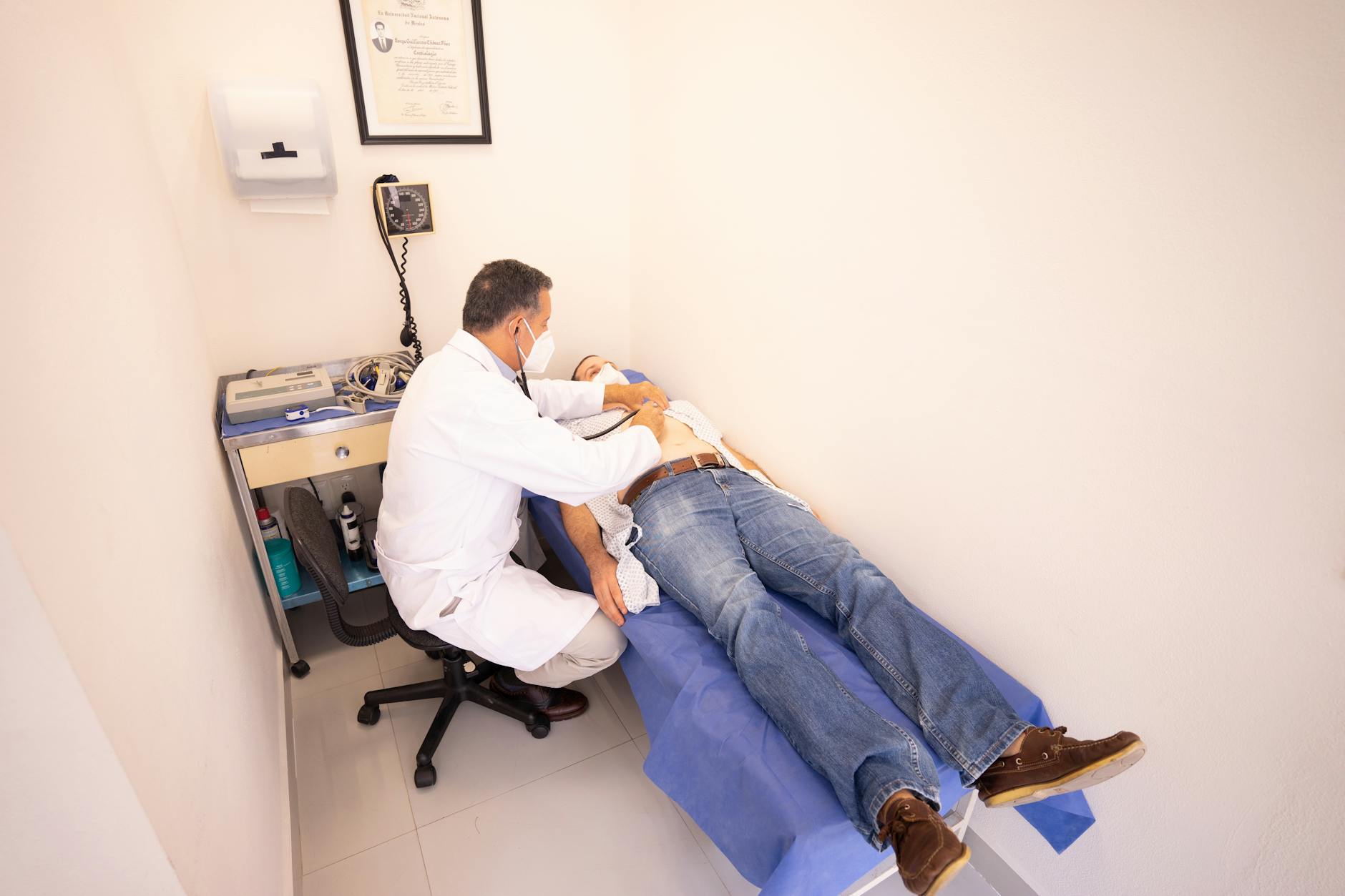
Asking a doctor whether a common headache might indicate a rare neurological condition affects a meaningful number of consultations every year. The internet gives equal visual weight to a condition affecting millions and one affecting fewer than a thousand people worldwide. Patients who encounter rare disease content often experience a phenomenon clinicians describe as symptom adoption where reading about a condition causes them to notice or exaggerate matching sensations. Most rare diseases have very specific diagnostic criteria that go far beyond the general symptoms listed in search results. A thorough clinical examination remains the only reliable way to distinguish between a common ailment and something genuinely unusual.
Cancer Concern

Presenting a doctor with a list of symptoms and asking directly whether cancer is the explanation is now one of the most frequently reported patient behaviors in general practice. Search engines tend to surface cancer-related content prominently because of the volume of existing medical literature on the subject. The visibility of cancer content online does not reflect its statistical likelihood as the cause of any given set of symptoms. Physicians are trained to rule out serious conditions systematically but note that patient anxiety driven by online research often requires its own management within the consultation. Reassurance backed by professional assessment carries considerably more clinical weight than any search result.
Supplement Interaction

Bringing a handwritten or photographed list of supplements to ask about potential drug interactions is a growing feature of modern medical appointments. The wellness industry produces an enormous volume of content promoting supplement combinations that have limited or no peer-reviewed safety data behind them. Patients frequently discover conflicting information across different health blogs and arrive at consultations hoping for a definitive answer. Doctors and pharmacists are the appropriate professionals to consult on interactions as they have access to validated clinical databases. Many interactions flagged by patients turn out to be either negligible or based on theoretical rather than documented risk.
Parasite Fear
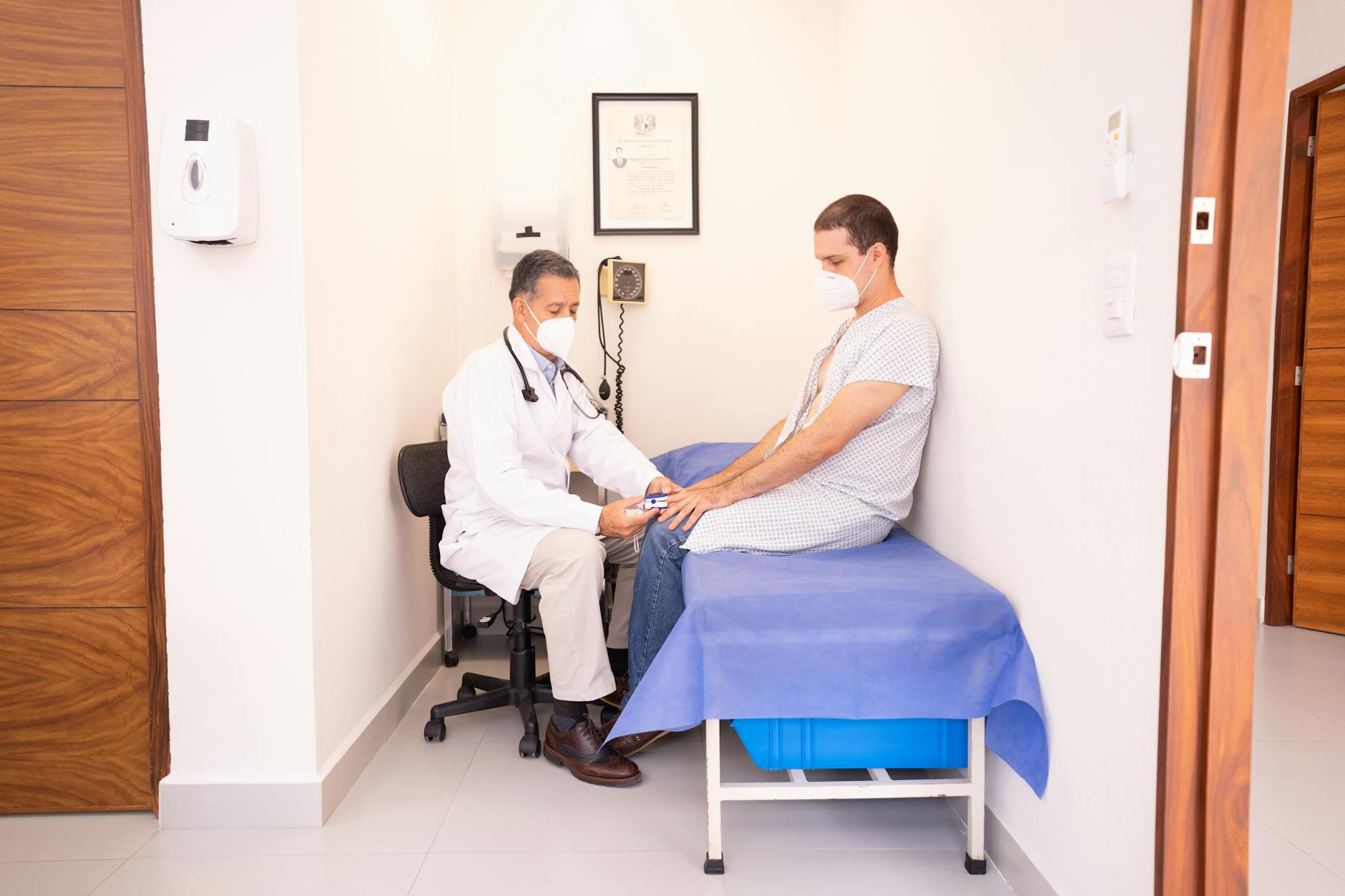
Asking a doctor to test for parasites based on general fatigue, bloating, or digestive symptoms is a consultation pattern that has grown substantially alongside alternative health content online. A specific genre of wellness influencer content promotes parasite cleansing protocols and presents vague symptoms as near-certain evidence of infestation. Clinical testing for parasites requires specific indicators and exposure history rather than symptom matching alone. The majority of patients who request parasite testing return results that show no evidence of infection. Gastrointestinal symptoms have a wide range of far more common explanations that a physician will investigate before considering parasitic causes.
Hormone Imbalance

Arriving at a doctor’s appointment convinced that a hormone imbalance is responsible for tiredness, mood changes, or weight fluctuation reflects the dominance of hormonal health content across social media platforms. Influencers and wellness brands frequently present hormone imbalance as a catch-all explanation for symptoms that have multiple possible causes. Actual hormonal disorders are diagnosed through blood panels interpreted against validated reference ranges rather than symptom lists found online. Many patients request specific hormone tests by name having encountered them in content that promotes expensive private testing packages. A general practitioner will typically conduct a broad assessment before ordering targeted endocrine investigations.
Microbiome Issues

Questioning whether gut microbiome disruption is behind symptoms ranging from brain fog to skin problems reflects the explosion of microbiome-related content in mainstream health media. The science of the gut microbiome is genuinely evolving but popular content frequently outpaces what clinical evidence currently supports. Patients arrive requesting probiotic prescriptions or specialist referrals based on articles that present microbiome research in overly simplified or commercially motivated terms. Most gastrointestinal symptoms are assessed through standard diagnostic pathways before microbiome-specific investigations are considered. Physicians welcome the growing public interest in gut health but note that the gap between research and ready clinical application remains significant.
Adrenal Fatigue

Asking about adrenal fatigue as a diagnosis is a consultation scenario that frustrates many clinicians because the condition does not exist as a recognized medical diagnosis in any major clinical framework. The term was popularized through alternative health content and describes a collection of symptoms attributed to overworked adrenal glands without a physiological basis accepted by endocrinology. Patients who arrive with this concern are typically experiencing real symptoms that have legitimate diagnosable causes including thyroid dysfunction, sleep disorders, or depression. A doctor will investigate the actual underlying cause rather than validate a framework unsupported by clinical evidence. The widespread circulation of adrenal fatigue content online has made it one of the more time-consuming misconceptions for practitioners to address.
Mold Toxicity

Presenting a doctor with a theory about chronic mold toxicity as the source of persistent symptoms is a consultation pattern that has grown alongside a specific community of environmental illness content creators. While certain molds do cause documented respiratory and allergic reactions the broader concept of systemic mold toxicity as described in alternative health spaces lacks consistent clinical validation. Patients sometimes arrive having already purchased home testing kits and detox protocols based on content that presents the condition as widely underdiagnosed. Physicians approach these concerns by investigating symptoms through established diagnostic routes rather than beginning with environmental toxin assumptions. Genuine mold-related illness is taken seriously by allergists and pulmonologists when specific clinical criteria are met.
Lyme Disease
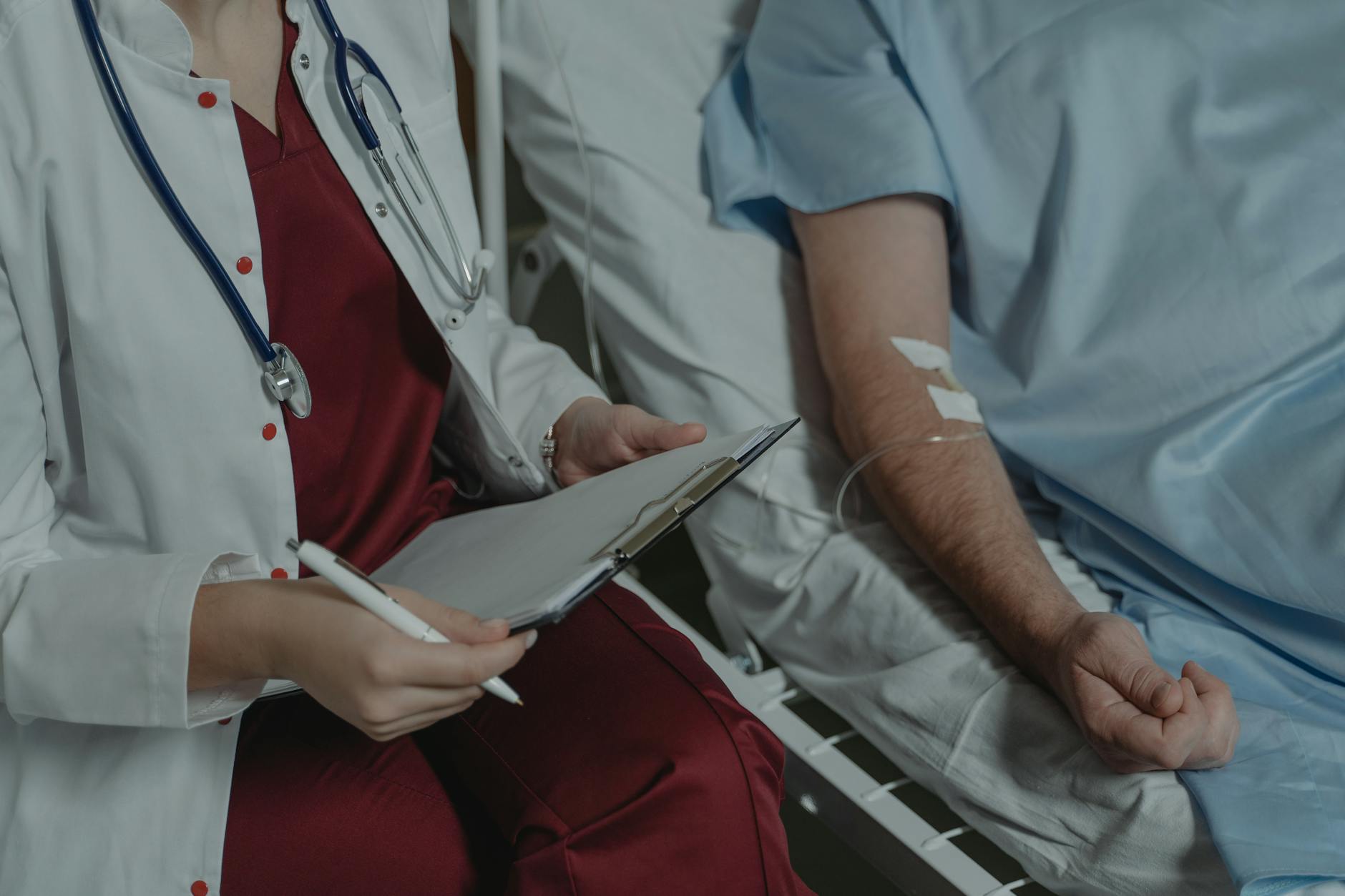
Requesting a Lyme disease test based on fatigue and joint pain without a documented tick exposure or geographic risk factor is a scenario general practitioners encounter with notable frequency. A significant online community advocates for the existence of a chronic form of Lyme disease that mainstream medicine does not currently recognize as a distinct condition. Patients who have spent time in online illness communities may arrive with deeply held convictions about their diagnosis that require careful and respectful clinical navigation. Standard Lyme testing follows a two-tier protocol and results are interpreted alongside exposure history and clinical presentation. Doctors are careful to take tick-borne illness seriously while also communicating clearly about the boundaries of current diagnostic evidence.
Heavy Metal Poisoning

Asking to be tested for heavy metal toxicity based on neurological symptoms or fatigue discovered through a health forum or detox-focused content is an increasingly common appointment scenario. Heavy metal poisoning is a genuine medical condition but it requires specific and documented exposure to toxic levels through occupational contact or environmental contamination. Consumer content in the detox space frequently presents heavy metals as a widespread hidden threat driving a broad range of unexplained symptoms. Clinical testing for heavy metals is targeted and exposure-driven rather than used as a general screening tool for fatigue or cognitive complaints. A physician will explore far more statistically likely explanations before ordering heavy metal panels.
Leaky Gut

Bringing up leaky gut syndrome as a suspected diagnosis reflects the influence of functional medicine content that has reached mainstream audiences through podcasts and social media. The concept of intestinal permeability is a real area of scientific inquiry but leaky gut as a standalone diagnosis driving systemic disease is not an accepted framework in conventional gastroenterology. Patients who raise it are often experiencing genuine gastrointestinal discomfort that warrants proper clinical investigation through established diagnostic tools. Conditions such as irritable bowel syndrome, celiac disease, or inflammatory bowel disease share many of the symptoms attributed to leaky gut in online content. A gastroenterologist working through validated diagnostic criteria is the appropriate resource for persistent digestive concerns.
Thyroid Problems
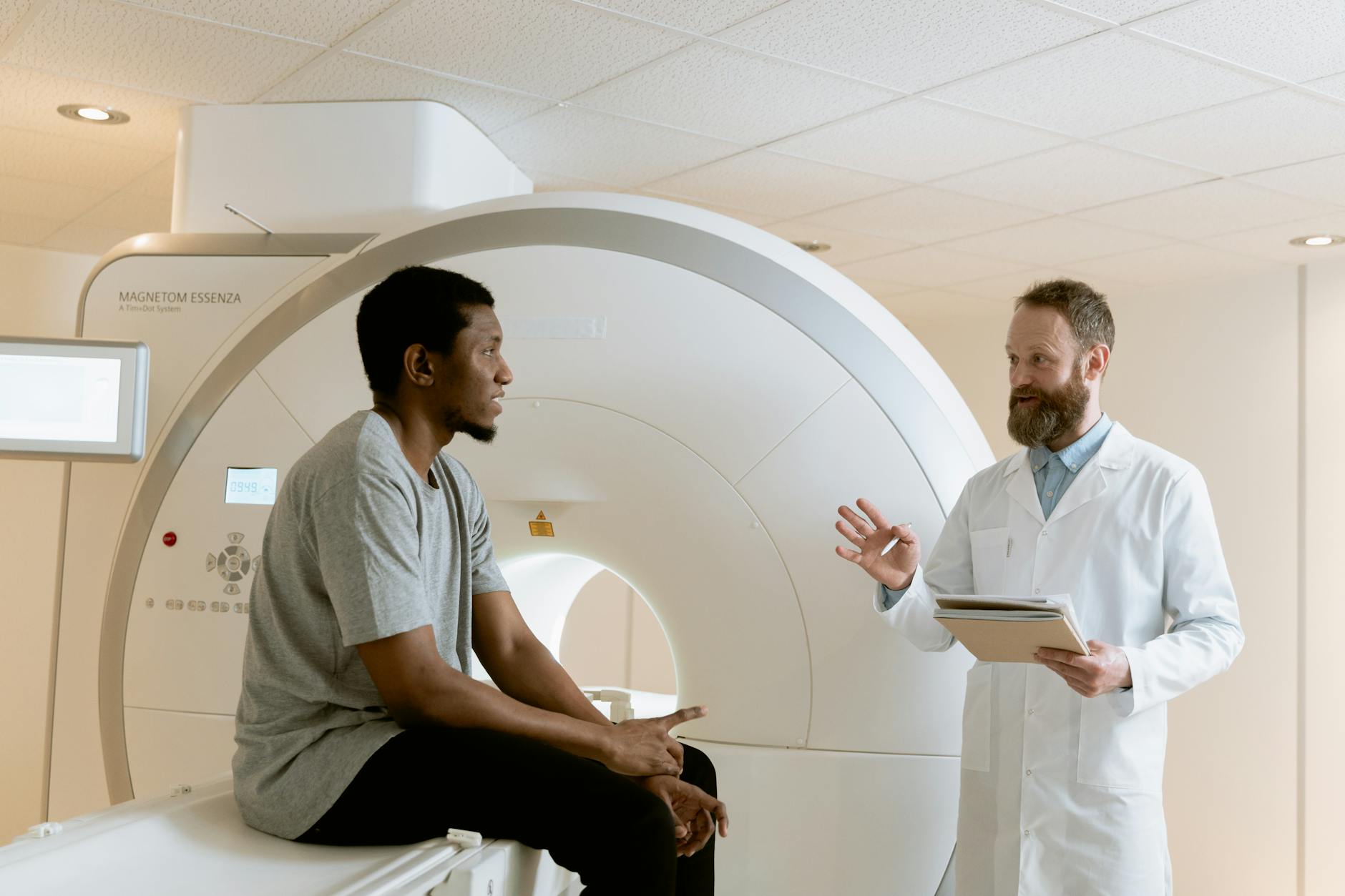
Presenting a doctor with a self-assembled list of symptoms and asking specifically whether the thyroid is responsible is one of the most consistent patterns in symptom-driven internet research. Thyroid dysfunction produces symptoms including fatigue, weight changes, temperature sensitivity, and mood shifts that overlap significantly with many other common conditions. Health content platforms frequently feature thyroid-related articles because the symptoms are relatable and the topic generates high engagement. A simple blood test measuring TSH levels is the standard first step in assessing thyroid function and is straightforward to arrange through a general practitioner. Many patients who arrive convinced of a thyroid explanation receive results within the normal reference range and require investigation of alternative causes.
Vitamin Deficiency

Asking a doctor to run a full vitamin panel after attributing tiredness or low mood to a likely deficiency is a consultation request shaped heavily by the supplement industry’s content marketing. Vitamin deficiency content is widely distributed across wellness platforms and is often framed around symptoms so general that most readers find themselves relating to at least several. Genuine deficiencies in vitamins such as B12 and D are clinically significant and do require testing when specific risk factors are present. However broad untargeted vitamin screening is not standard clinical practice and is unlikely to be ordered without supporting indicators. A focused conversation about diet, lifestyle, and specific symptoms helps a physician determine whether targeted testing is appropriate.
Autoimmune Condition

Arriving at an appointment convinced of an autoimmune diagnosis after hours spent in online patient communities is a scenario that requires careful handling by clinicians. Autoimmune conditions are genuinely complex to diagnose and many share overlapping symptom profiles that make self-identification through online research particularly unreliable. Patient forums and social media groups can create a powerful sense of recognition that feels like confirmation even in the absence of clinical evidence. Rheumatologists and immunologists use a combination of bloodwork, physical examination, and documented symptom history to work toward a formal diagnosis. A general practitioner will conduct an initial assessment and refer to a specialist when the clinical picture genuinely warrants further investigation.
Anxiety Disorder

Asking a doctor whether symptoms like chest tightness, dizziness, and fatigue might be anxiety after reading about it online reflects a pattern where internet research occasionally leads patients toward accurate self-identification. Anxiety disorders are among the most common conditions seen in general practice and the symptoms do overlap extensively with several physical health conditions. Physicians always rule out physiological causes before attributing symptoms to a psychological origin regardless of how convincing a patient’s self-assessment may appear. A formal mental health screening conducted by a qualified clinician provides far more diagnostic value than a symptom checklist completed alone at midnight. When anxiety is confirmed as the underlying cause a doctor is well positioned to discuss evidence-based treatment pathways including therapy and medication options.
Sleep Apnea

Presenting a sleep tracking app report as evidence of suspected sleep apnea is a modern consultation scenario that doctors are encountering with growing regularity. Consumer wearable devices measure movement and heart rate variability as proxies for sleep quality but they do not constitute clinical diagnostic tools for respiratory sleep disorders. Sleep apnea is diagnosed through polysomnography or a validated home sleep study conducted under medical guidance. Patients who arrive with app data are not wrong to flag their concerns but the data itself cannot confirm or rule out a clinical diagnosis. A physician will take sleep-related concerns seriously and refer to a sleep specialist when symptoms such as witnessed apneas, excessive daytime sleepiness, or oxygen desaturation indicators are present.
Genetic Testing

Asking a doctor to act on results from a direct-to-consumer genetic testing kit is a consultation scenario that places clinicians in a challenging interpretive position. Consumer kits from platforms that analyze DNA for health predispositions use different methodologies and population datasets than clinical genetic testing. Variants flagged as elevated risk by consumer reports may not meet the threshold for clinical significance or may have already been superseded by more current research. Genetic counselors rather than general practitioners are the appropriate professionals to interpret complex hereditary risk information in a clinical context. Doctors welcome patient engagement with genetic health but emphasize that consumer test results require professional interpretation before any clinical action is taken.
Electromagnetic Sensitivity
Asking a doctor to investigate symptoms attributed to electromagnetic field exposure from devices, routers, or mobile towers is a consultation request that sits outside the current boundaries of clinical evidence. Major health organizations including the World Health Organization have reviewed the available research and do not recognize electromagnetic hypersensitivity as a condition with a verified physiological mechanism. Patients who hold this belief are often experiencing real symptoms that have diagnosable explanations unrelated to electromagnetic exposure. Physicians are encouraged to take the distress caused by these beliefs seriously while guiding patients toward evidence-based investigation of their actual symptoms. The volume of online content promoting electromagnetic sensitivity has contributed to a growing number of appointments centered on the concern.
Gluten Intolerance

Arriving at an appointment having already eliminated gluten from the diet and asking for a celiac diagnosis reflects a common sequencing problem created by online health advice. Celiac disease testing requires active gluten consumption for accurate results meaning patients who have already self-treated render standard blood panels unreliable. Non-celiac gluten sensitivity is a recognized but less clearly defined condition that does not show up on celiac antibody tests. Many patients who attribute digestive symptoms to gluten through online research turn out to have other conditions including irritable bowel syndrome or fructose malabsorption. A gastroenterologist can guide patients through the correct diagnostic process including the necessary dietary preparation before testing begins.
Chronic Fatigue

Asking a doctor to confirm a chronic fatigue syndrome diagnosis after extensive online research about persistent tiredness is a consultation scenario requiring careful clinical navigation. The condition is real and recognized but it is a diagnosis of exclusion meaning many other potential causes must be ruled out before it can be formally established. Online chronic fatigue communities provide genuine support but can also lead members toward premature diagnostic conclusions before a thorough clinical workup has been completed. Physicians assess fatigue through a systematic process that includes bloodwork, sleep assessment, mental health screening, and physical examination. A formal diagnosis of chronic fatigue syndrome carries implications for treatment planning that make professional assessment essential rather than optional.
Blood Type Diet
Asking a doctor whether eating according to blood type could explain persistent health issues or improve specific symptoms is a question that reflects the remarkable longevity of a nutritional theory without scientific support. The blood type diet concept was popularized decades ago and continues to circulate through wellness content despite repeated failure to demonstrate clinical efficacy in peer-reviewed research. Blood type is determined by antigens on red blood cells and has no established relationship to how the digestive system processes food groups. Nutritional guidance in clinical practice is based on individual health status, metabolic markers, and validated dietary science rather than blood group categorization. A registered dietitian working alongside a physician is the appropriate resource for evidence-based personalized nutrition advice.
Detox Cleanse

Asking a doctor to support or supervise a commercial detox cleanse based on content promising to flush toxins from the liver or digestive system is a request that arrives in consultations with considerable regularity. The human body operates a continuous and sophisticated detoxification system through the liver, kidneys, lymphatic system, and skin without requiring supplemental intervention. Commercial cleanse products are classified as food supplements rather than medical treatments meaning they are not subject to the same regulatory scrutiny as pharmaceuticals. Physicians note that many cleanse protocols are nutritionally restrictive and can interfere with medication absorption or exacerbate existing health conditions. Genuine concerns about liver or kidney function are investigated through standard blood panels ordered and interpreted by a qualified clinician.
Have you ever walked into a doctor’s office armed with an internet diagnosis that turned out to be completely wrong? Share your experience in the comments.





