Walking into a medical office can feel nerve-wracking, and most patients have no idea that certain habits and behaviors quietly raise eyebrows among the nursing staff. Nurses are trained professionals who have seen it all, yet some patient behaviors stand out as particularly common sources of quiet frustration. From skipping basic hygiene to bending the truth about lifestyle choices, these habits make the experience harder for everyone involved. Understanding what nurses silently notice can help patients become more considerate and get better care. Here are twenty things patients do at the doctor that nurses are quietly judging.
Shaving Last Minute

Many patients scramble to shave their legs or other areas right before an appointment, as if nurses are evaluating their grooming standards. Nurses notice the fresh razor burn and nicks immediately, and it creates extra caution during any skin assessments. The rush often causes irritation that can complicate a basic physical examination. Nurses genuinely do not care about body hair, and no one on the medical team is forming opinions about it. Skipping the last-minute prep entirely would save patients unnecessary discomfort.
Cologne Overload

Arriving at a medical appointment drenched in perfume or cologne is one of the most immediately noticed habits among nursing staff. Medical environments require careful attention to smell as a diagnostic tool, and heavy fragrance can mask important clinical information. Many nurses and fellow patients suffer from fragrance sensitivities that cause headaches and respiratory irritation during a shift. The confined space of an exam room makes the situation significantly more uncomfortable for everyone present. A fragrance-free approach to medical visits is always the more considerate choice.
Downplaying Symptoms
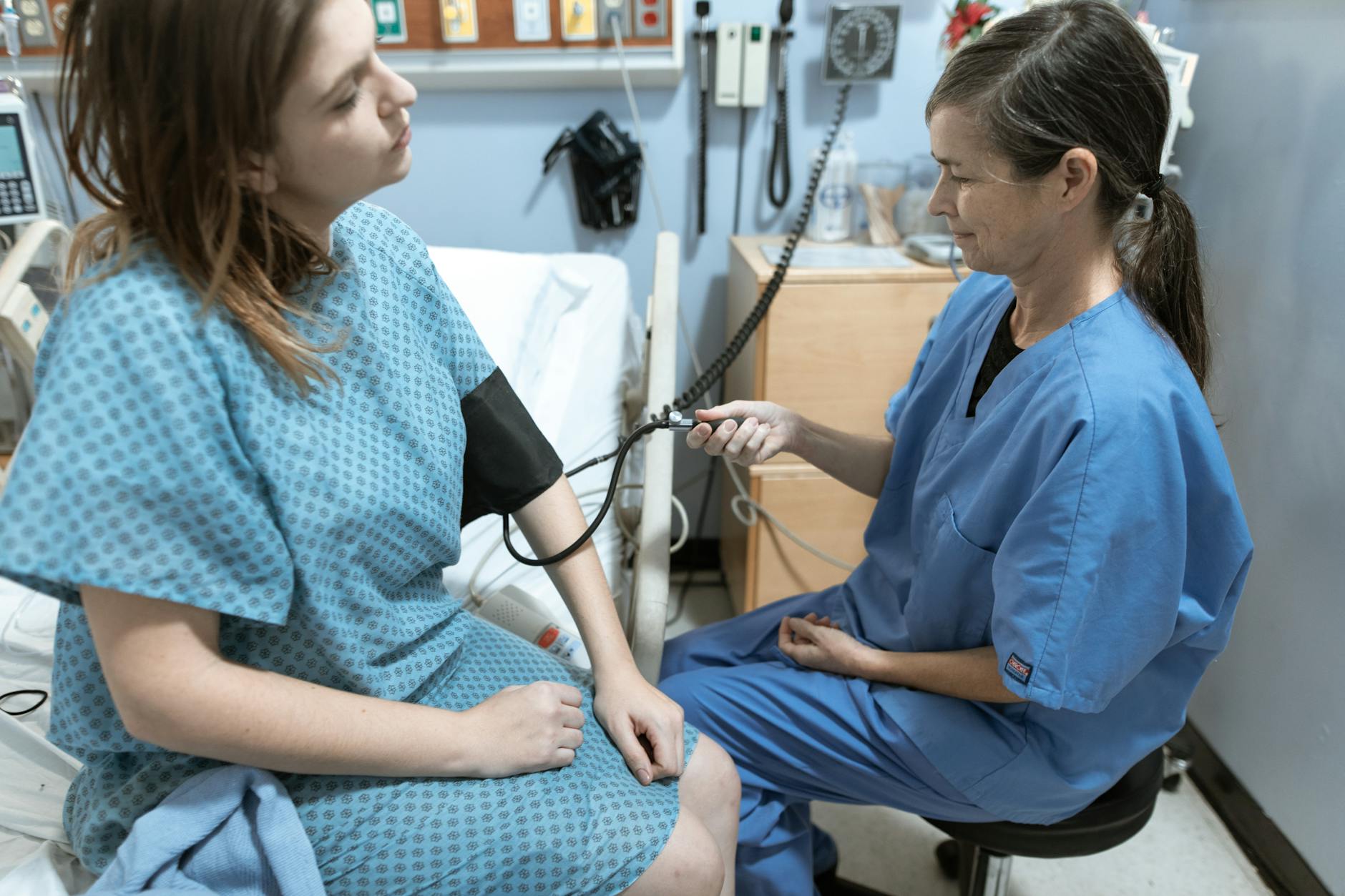
Patients frequently minimize what they are experiencing in order to avoid seeming dramatic or wasting the doctor’s time. Nurses are trained to read between the lines, and they can often tell when someone is holding back important details about their condition. This habit can lead to incomplete assessments and missed diagnoses that affect long-term health outcomes. The medical team needs accurate information to provide the best possible care, and downplaying symptoms works directly against that goal. Honest and thorough descriptions of what a patient is feeling are always the most helpful approach.
Googling Before Visiting
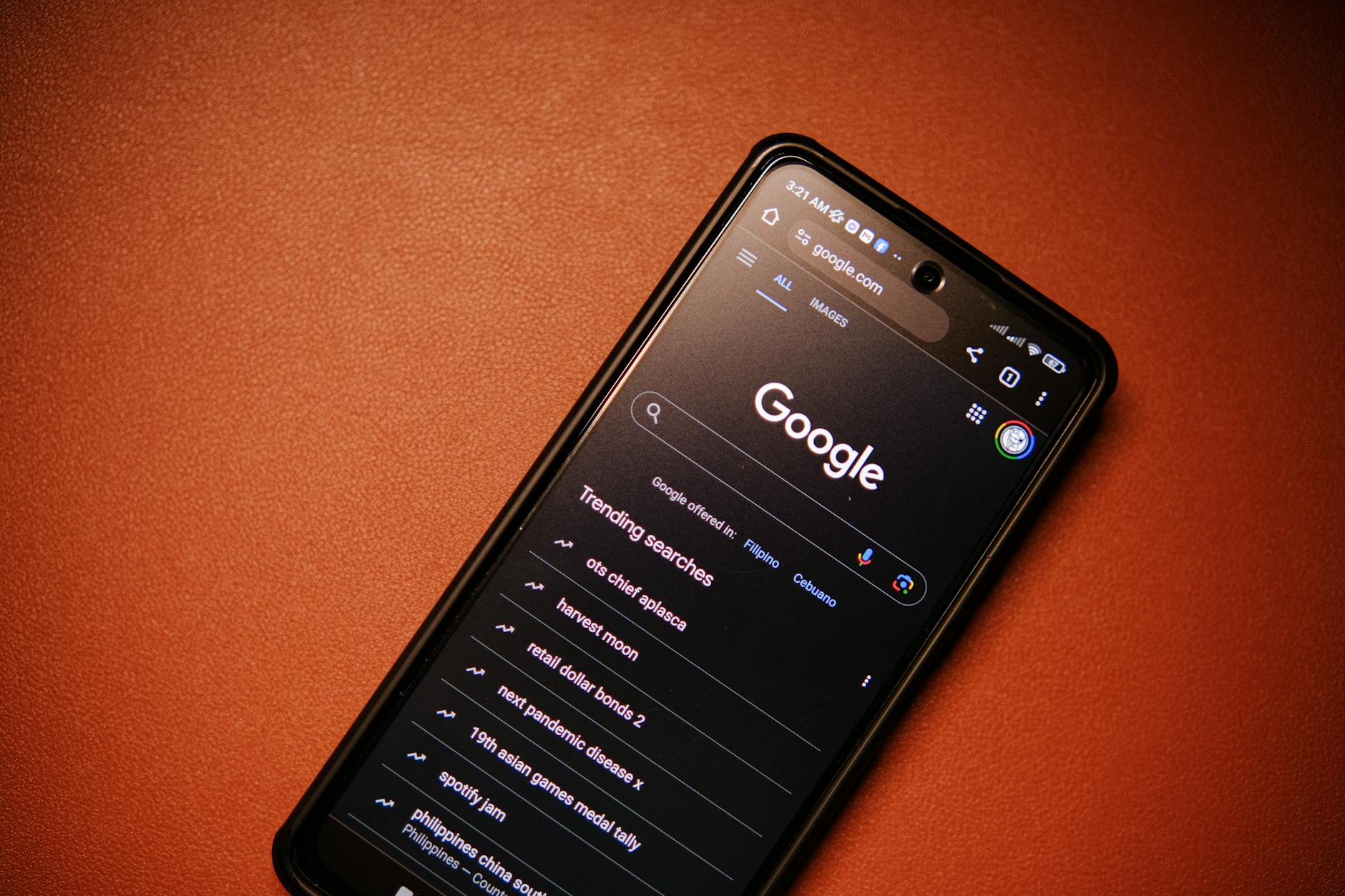
Arriving at an appointment armed with a self-diagnosis from an internet search is one of the most common habits nurses encounter. Patients who have already decided what is wrong with them tend to resist examination findings that contradict their online conclusions. This creates longer appointments and can derail the clinical process before it even begins. Medical websites are helpful for general awareness, but they cannot replicate the diagnostic process of a trained professional. Entering appointments with an open mind allows nurses and doctors to do their jobs far more effectively.
Lying About Drinking

Understating alcohol consumption is so common that medical professionals have developed specific questioning techniques designed to get more accurate answers. Nurses and doctors use standardized screening tools precisely because patients routinely report drinking far less than they actually do. Alcohol intake has direct implications for medication dosing, surgical risk, and overall treatment planning. The information shared in a medical setting is confidential and exists solely to improve patient care. Accurate reporting always leads to safer and more appropriate treatment decisions.
Phone Ignoring

Continuing to scroll through a phone while a nurse is taking vitals, asking intake questions, or explaining procedures is noticed every single time. It slows down the appointment and forces the nurse to repeat important instructions that the patient missed while distracted. Medical information shared during intake is clinically relevant and often determines the course of the entire visit. Nurses are working efficiently through a full schedule, and divided attention creates delays that affect every patient afterward. Putting the phone away during the clinical interaction is a simple habit that makes a significant difference.
Pretending to Exercise

Claiming a regular exercise routine that clearly does not match physical indicators is something nurses encounter constantly during health assessments. Resting heart rate, blood pressure, and other basic measurements often tell a different story than the one a patient presents verbally. Fitness history affects recommendations for everything from weight management to cardiac monitoring and surgical preparation. The nursing staff is not there to pass judgment on lifestyle choices but to gather accurate data for effective care. Honest answers about activity levels result in more realistic and helpful health guidance.
Skipping the Shower

Showing up to a medical appointment without basic hygiene preparation is one of the habits nurses find most difficult to navigate professionally. Physical examinations require close contact, and strong body odor makes the process uncomfortable for the clinical team performing the assessment. It also creates a lingering effect in the exam room that affects appointments scheduled afterward. Most patients would not meet a new colleague or attend an important meeting without freshening up beforehand. Treating a medical appointment with the same basic courtesy makes the experience more comfortable for everyone involved.
WebMD Panicking

Patients who arrive visibly convinced they have a rare or terminal condition based on a symptom search are a familiar presence in medical waiting rooms. The anxiety this creates can elevate blood pressure and heart rate in ways that complicate accurate baseline readings. Nurses spend time managing the emotional fallout of internet-driven health panic before any real clinical work can begin. Most symptoms have multiple possible explanations, and the vast majority of presentations have straightforward and treatable causes. Arriving at appointments without a predetermined catastrophic conclusion allows the clinical process to unfold more calmly.
Forgetting Medications
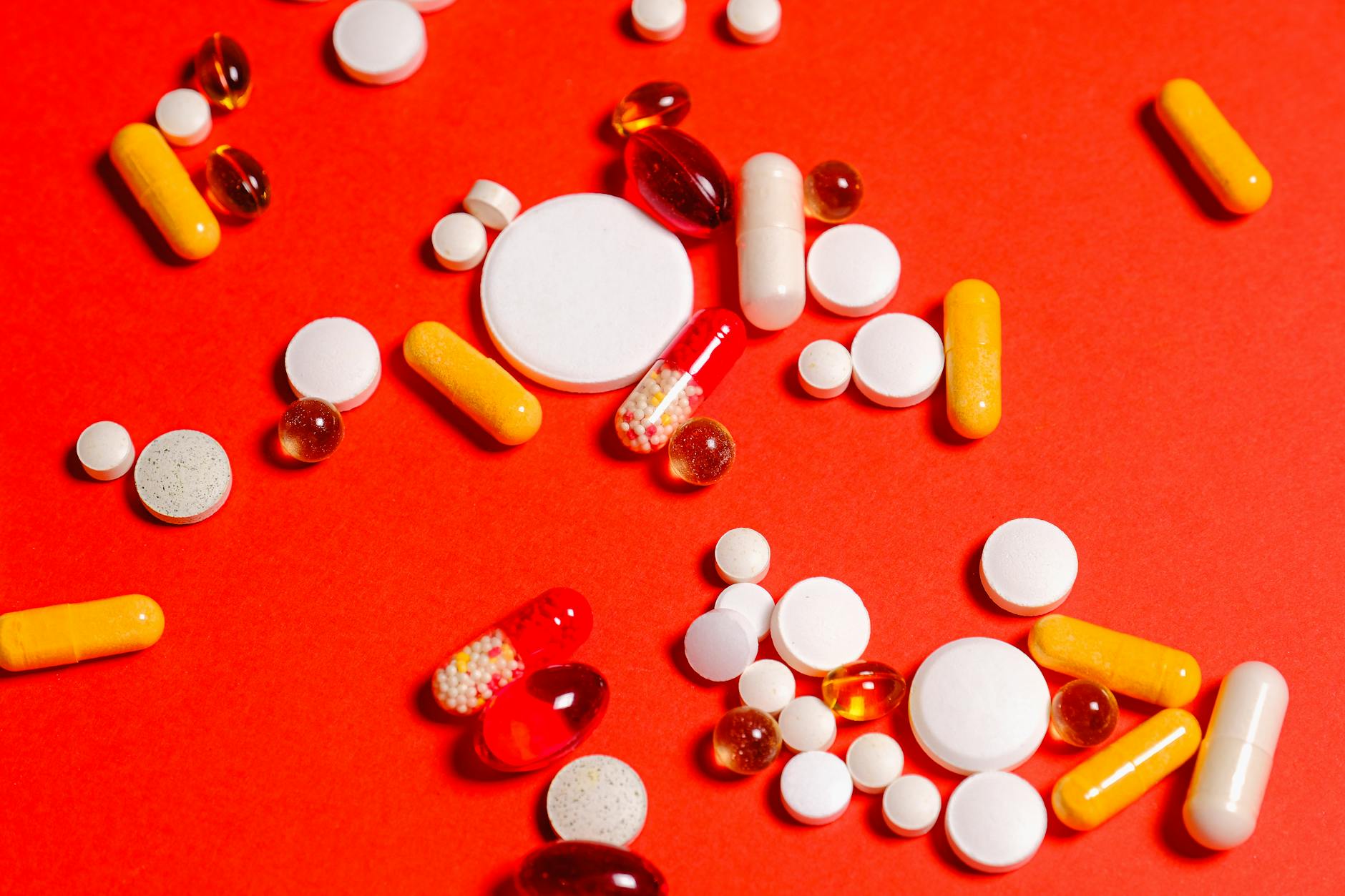
Coming to an appointment without a list of current medications is a habit that creates unnecessary complications during intake. Nurses need to know exactly what a patient is taking, including supplements and over-the-counter products, to avoid dangerous interactions. Vague responses like “some kind of blood pressure pill” or “a small white tablet” are not clinically useful and slow the entire process down. Most pharmacies can provide a printed medication list with a simple request made before the appointment. Keeping an updated record on a phone or in a wallet takes minimal effort and has a significant impact on care quality.
Waiting Room Oversharing

Loudly discussing personal medical details in the waiting room is a habit that nurses and administrative staff quietly observe with discomfort. Medical histories and symptoms are private information that other patients and staff did not consent to hearing in a shared space. This is particularly common with phone calls taken in waiting areas, where full symptom descriptions are broadcast to an entire room. Most facilities have private check-in options or quiet areas designed specifically for patient conversations. Saving detailed medical discussions for the exam room protects both patient privacy and the comfort of others nearby.
Arguing the Prescription

Patients who arrive expecting a specific medication and become visibly frustrated when the provider recommends something different create a tense dynamic for the entire clinical team. Nurses are often positioned between the patient’s expectations and the doctor’s clinical reasoning, which puts them in an uncomfortable intermediary role. Prescription decisions are based on current clinical guidelines, patient history, and medical judgment rather than personal preference. Requesting an explanation for a treatment decision is entirely appropriate, but demanding a specific drug is a different matter entirely. Trusting the clinical team’s expertise leads to better outcomes and more productive appointments.
Dirty Feet Surprise

Presenting with unwashed or notably unkempt feet during a visit that does not involve foot-related concerns is something nurses notice immediately. Podiatric health can reveal important information about circulation, diabetes, and overall hygiene habits, which means nurses pay attention to feet even during routine checkups. General cleanliness from head to toe reflects a patient’s awareness of basic personal care, which factors into broader health conversations. Basic foot hygiene before any appointment requires minimal effort and makes physical examinations far more manageable. Treating all areas of the body as potentially relevant to the visit is always a sound approach.
Constant Self-Diagnosing
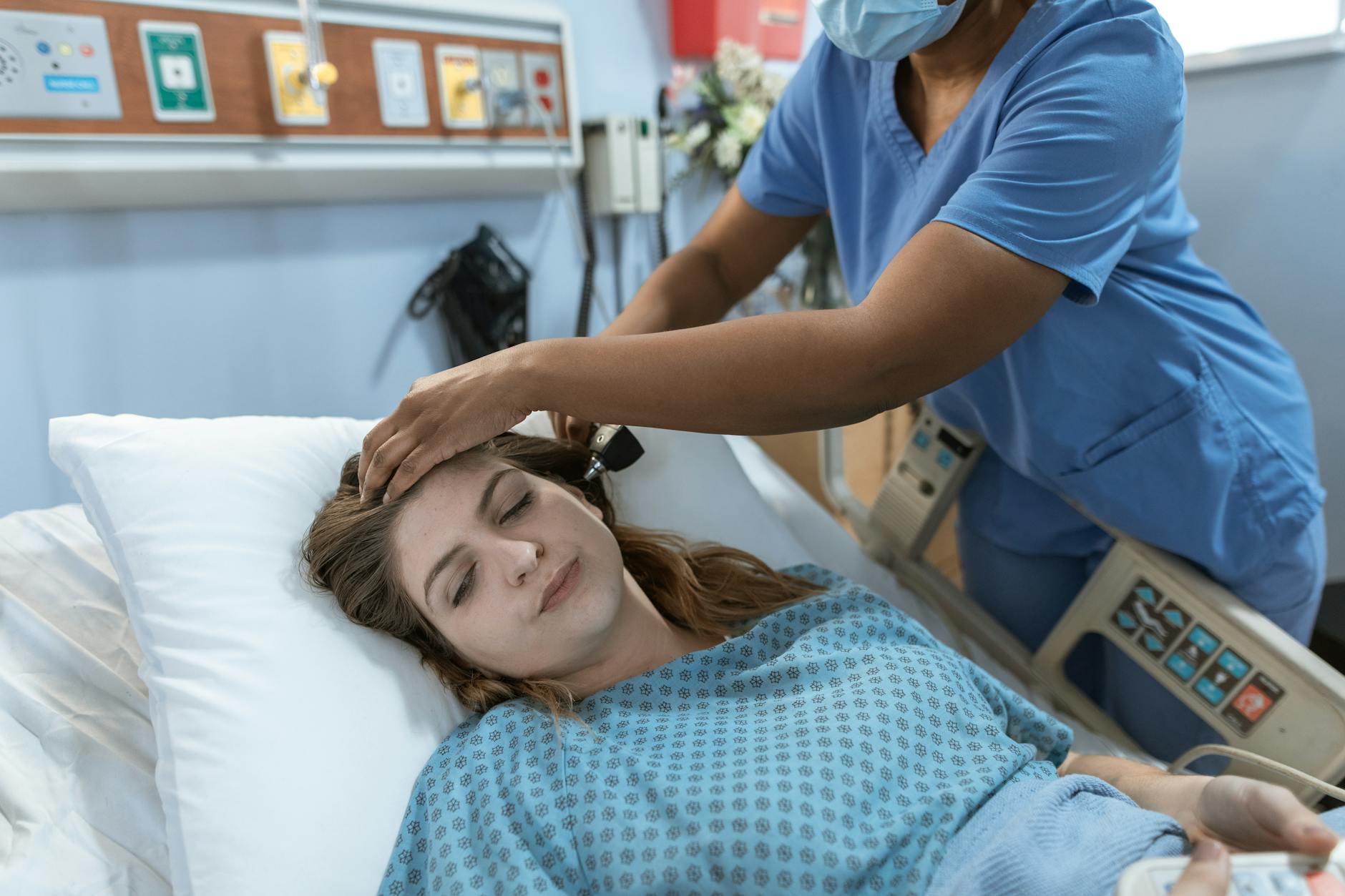
Patients who interrupt clinical explanations with their own diagnostic theories make it significantly harder for nurses to complete accurate assessments. Every counter-explanation requires additional time and patience from a team that is already working through a full schedule of patients. Clinical training involves years of education and hands-on experience that cannot be replicated through reading health articles online. Nurses respect patients who ask questions and engage thoughtfully with their care, which is a very different dynamic from dismissing professional findings outright. Listening first and asking questions second creates a far more productive clinical interaction.
Appointment Lateness

Arriving significantly late to a scheduled appointment and then expecting to receive the full allotted time is one of the habits that nurses find most professionally challenging. Medical schedules are structured tightly, and a late patient creates a ripple effect that delays care for everyone else on the roster. Nurses are responsible for managing patient flow and must absorb the stress of schedule disruptions across an entire clinic day. Most facilities have clear policies about late arrivals that exist specifically to protect all patients’ access to timely care. Building in extra travel time for medical appointments is a straightforward habit that demonstrates respect for everyone’s time.
Vague Pain Descriptions

Answering pain assessment questions with “I don’t know, it just hurts” gives nurses almost nothing clinically useful to document or act on. Location, intensity, duration, triggers, and the nature of the sensation are all pieces of information that shape diagnosis and treatment decisions significantly. Nurses are trained to ask follow-up questions, but the back-and-forth takes additional time that delays care for the patient and others. Thinking about pain characteristics before an appointment and being prepared to describe them clearly is a habit that dramatically improves the clinical visit. The more specific the description, the more targeted and effective the medical response can be.
Bringing an Audience

Arriving with multiple family members or friends who crowd into the exam room creates logistical and privacy challenges that nurses must navigate carefully. Clinical conversations about sensitive health topics are more complicated when an uninvited audience is present and offering their own commentary. Medical decisions belong to the patient, and the presence of strong-willed companions can sometimes override patient preferences in ways that concern clinical staff. Most exam rooms are designed for a provider, a nurse, and one patient, with limited physical and emotional space beyond that. Discussing beforehand who will genuinely support the visit rather than overwhelm it makes the experience smoother for everyone involved.
Skipping Follow-Ups
Patients who repeatedly fail to attend scheduled follow-up appointments and then return with worsened conditions place a significant burden on the clinical team. Nurses document care plans and follow-up instructions carefully, knowing that continuity is essential to effective treatment. Skipping these appointments often leads to more intensive interventions later that could have been avoided with consistent monitoring. The frustration within the nursing team is not directed at the patient personally but at a system where preventable deterioration becomes the norm. Prioritizing scheduled follow-ups is one of the most impactful habits a patient can adopt for long-term health.
Undressing Too Soon

Stripping down completely before being asked or instructed to do so catches nurses off guard during intake and preparation. Clinical undressing protocols exist to protect patient dignity and ensure that examinations proceed in a structured and appropriate sequence. Jumping ahead of the process creates awkward moments and sometimes means a patient must be re-draped entirely before the actual examination can begin. Nurses will always provide clear instructions about what to remove and when, which removes any need to guess or act preemptively. Waiting for guidance before disrobing is a simple habit that keeps the clinical process running smoothly.
Hiding the Real Reason

Mentioning the actual reason for a visit as an afterthought right at the end of the appointment is something nurses recognize immediately as the classic “doorknob moment.” Patients often spend the entire appointment discussing secondary concerns before finally revealing the issue that prompted the visit in the first place. This habit leaves no clinical time to properly address the most pressing concern and forces rushed assessments that compromise care quality. Nurses understand that embarrassment or anxiety often causes patients to bury the real issue beneath safer topics. Stating the primary concern at the very beginning of the appointment ensures it receives the attention and time it deserves.
Have you experienced any of these moments from either side of the exam table? Share your thoughts in the comments.





