The veterinary industry occupies a uniquely powerful position in consumer relationships because the emotional stakes of pet ownership make rational purchasing decisions extraordinarily difficult to maintain in a clinical setting. When a white coat explains a treatment option in medical language while a beloved animal sits on the examination table, the psychological conditions for overselling are close to perfect. Corporate consolidation of veterinary practices has introduced revenue targets, upselling protocols, and commission structures into clinical environments that were once governed almost entirely by independent professional judgment. This does not mean that every recommendation is unnecessary or that every veterinarian is operating in bad faith, but it does mean that pet owners who understand the specific mechanisms of veterinary overselling are significantly better equipped to make informed decisions about their animal’s care. Here are 23 ruthless ways that some vets and corporate veterinary practices push expensive treatments that many pets will never actually need, ordered from the most financially impactful to the quietly costly.
Dental Cleanings
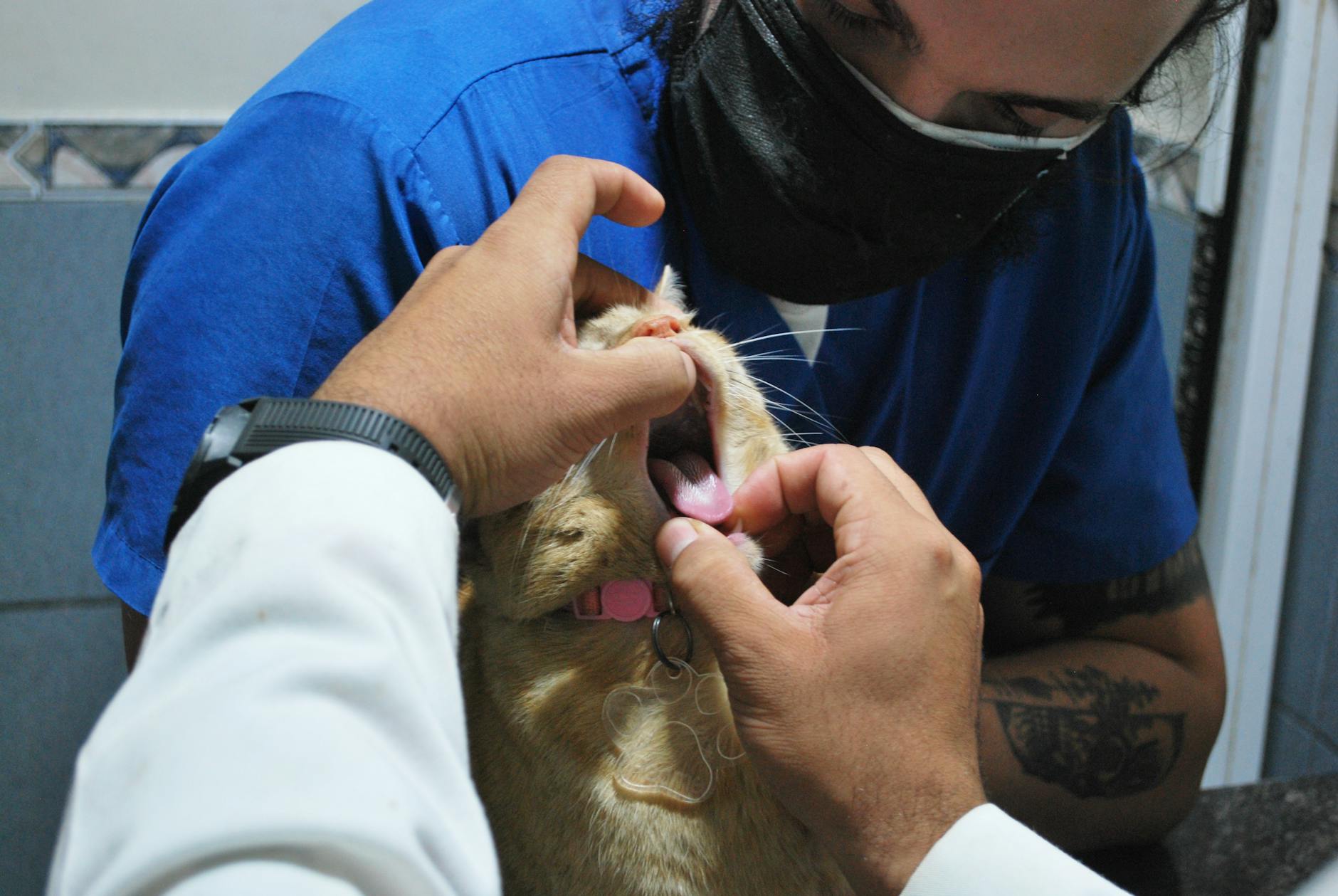
Annual or biannual prophylactic dental cleanings requiring full general anesthesia are recommended as a blanket protocol by many corporate veterinary practices regardless of the individual animal’s actual dental condition, breed-specific risk profile, or home dental care routine. General anesthesia carries real physiological risk particularly in older animals and the decision to anesthetize a healthy pet for a preventive procedure that may show no significant findings should be supported by a documented clinical justification rather than a calendar-based recall system. Independent veterinary dental specialists consistently note that cleaning frequency should be determined by individual oral health assessment rather than by a standardized schedule applied uniformly across all patients. The procedure cost including pre-anesthetic bloodwork, anesthesia monitoring, and post-procedure medications frequently reaches several hundred to over a thousand dollars per event. Pet owners are well within their rights to request a detailed clinical justification for why their specific animal requires anesthesia-based cleaning at the recommended interval rather than accepting the schedule as a given.
Vaccine Packages

Bundled vaccine packages that include every available vaccine regardless of the individual animal’s actual exposure risk are a standard revenue structure at many general practice clinics, sold as comprehensive protection without differentiation between core vaccines that every animal genuinely needs and non-core vaccines whose benefit depends entirely on lifestyle and geographic exposure factors. The rabies vaccine and a small number of core combination vaccines are genuinely indicated for most pets but a significant portion of the vaccines offered in standard packages including leptospirosis, bordetella, lyme, canine influenza, and feline leukemia have meaningful benefit only for animals with specific exposure profiles. Veterinary immunology guidelines published by professional bodies including the American Animal Hospital Association explicitly distinguish core from non-core vaccines and recommend non-core vaccines only when lifestyle assessment supports a genuine exposure risk. A pet that lives entirely indoors, does not board, does not visit dog parks, and does not have contact with wildlife has a fundamentally different vaccine risk profile than one with regular outdoor exposure and the two animals do not require identical vaccine packages. Requesting an itemized lifestyle-based vaccine assessment rather than accepting a bundled package is a reasonable and clinically supported request.
Pre-Anesthetic Bloodwork

Pre-anesthetic bloodwork is presented at most practices as a mandatory safety requirement before any procedure involving sedation, but the clinical evidence supporting universal pre-anesthetic screening in young and apparently healthy animals is considerably weaker than the confident manner of its recommendation suggests. Major veterinary anesthesia guidelines indicate that pre-anesthetic screening is most clinically justified in animals over a certain age threshold, those with known health conditions, or those showing clinical signs that warrant investigation and that routine screening in young healthy animals has a low yield for detecting actionable abnormalities. The practice of requiring pre-anesthetic bloodwork as a non-negotiable add-on to every procedure including routine spays, neuters, and dental cleanings in young healthy patients generates significant additional revenue while providing marginal clinical benefit in the majority of cases. Pet owners can ask their veterinarian to specify which clinical findings or risk factors in their particular animal make pre-anesthetic bloodwork specifically indicated rather than accepting the universal requirement without justification. This conversation will quickly distinguish practices that apply screening based on individual clinical assessment from those applying it as a standard revenue line item.
Specialty Diets
Prescription and veterinary-exclusive diet recommendations made at the point of a routine wellness visit without a documented diagnosis of a condition that the diet specifically addresses represent one of the most profitable and least scrutinized upselling opportunities in general veterinary practice. Veterinary prescription diets carry significant price premiums over equivalent commercial foods and are legally sold only through veterinary channels, creating a captive market and a direct financial relationship between the recommending practice and the product sale. Many of the conditions for which prescription diets are marketed including joint support, weight management, urinary health, and cognitive support can be addressed through dietary adjustments achievable with high-quality commercial foods at a fraction of the prescription cost. Veterinary nutritionists who operate independently of product relationships frequently note that the clinical justification for prescription diets is strong for specific documented medical conditions and weak to absent as a preventive measure in healthy animals. Asking for a specific diagnostic basis for a prescription diet recommendation and exploring whether the condition can be managed with evidence-based dietary modifications outside the prescription channel are legitimate and productive questions for any pet owner facing this recommendation.
Joint Supplements

Recommending glucosamine, chondroitin, omega-3, and joint support supplements as a routine addition to the care plan of any middle-aged or senior pet regardless of clinical signs of joint disease or breed-specific risk factors is a widespread practice whose revenue benefit to the practice substantially exceeds its documented clinical benefit to the average animal receiving it. The evidence base for joint supplements in companion animals is mixed with some studies showing modest benefits in animals with documented osteoarthritis and much weaker evidence supporting prophylactic use in animals with no clinical or radiographic evidence of joint pathology. Veterinary supplement sales represent a significant revenue stream at general practices because supplements are unregulated, carry high margins, require no prescription infrastructure, and can be recommended without a specific diagnosis to justify the recommendation. An owner whose young healthy pet is sent home with a joint supplement regimen following a routine wellness visit is in a reasonable position to ask for the specific clinical evidence supporting that recommendation for their animal’s age, breed, and body condition. Independent veterinary internal medicine specialists are a more reliable source of supplement guidance than a general practice with a financial relationship to specific supplement brands.
Allergy Testing
Comprehensive intradermal or serum-based allergy testing panels costing several hundred to over a thousand dollars are sometimes recommended for pets presenting with mild or intermittent skin irritation, itching, or digestive upset before basic and inexpensive diagnostic steps including dietary elimination trials and environmental modification have been systematically attempted. Veterinary dermatologists, who are the specialists most qualified to interpret allergy testing results, consistently indicate that serum allergy tests in particular have poor specificity in companion animals meaning they generate a high rate of positive results that do not correspond to clinically relevant sensitivities. The recommendation of comprehensive allergy testing as a first-line response to minor dermatological symptoms, rather than as a referral-level investigation after basic measures have been exhausted, frequently reflects the diagnostic revenue opportunity the testing represents rather than a stepwise clinical approach. A dietary elimination trial using a truly novel protein or hydrolyzed protein diet conducted over eight to twelve weeks costs a fraction of a comprehensive allergy panel and resolves the diagnostic question for food allergy with greater clinical reliability than serum testing. Pet owners whose animals are referred for comprehensive allergy panels at a first or second visit for mild symptoms are entitled to ask why less expensive diagnostic steps have been bypassed.
Cancer Screening

Routine cancer screening panels for pets marketed as annual wellness add-ons, typically involving blood biomarker tests with names suggesting comprehensive oncological surveillance, are a relatively new and rapidly growing revenue category whose clinical utility in asymptomatic animals is not supported by the current evidence base in veterinary oncology. Veterinary oncologists distinguish between diagnostic testing in animals presenting with clinical signs suggestive of neoplasia and population-level screening in asymptomatic animals, noting that the latter generates a high rate of false positives that lead to additional costly investigation without improving outcomes in the majority of cases. The emotional leverage of cancer screening is exceptionally high in the veterinary context because pet owners understandably respond strongly to the proposition of catching cancer early and practices that offer these panels without contextualizing the evidence limitations are using that emotional leverage commercially. The positive predictive value of a cancer screening test depends on the prevalence of the cancer being screened for in the specific animal being tested and blanket annual screening in young healthy animals of non-predisposed breeds has a very poor positive predictive value by mathematical necessity. Asking specifically about the evidence base for cancer screening in your pet’s specific breed, age, and risk category is the appropriate response to this recommendation.
Microchipping Packages

Microchipping is a genuinely useful and low-cost procedure whose value is well established and whose basic implementation is straightforward, but the packaging of microchipping with activation fees, annual registry subscription services, lost pet alert systems, and GPS monitoring add-ons converts a twenty-dollar procedure into a recurring revenue product that generates ongoing charges for services that are largely duplicative of free registry options. A microchip is a passive RFID device that requires no subscription, no battery, and no ongoing service to function for its core purpose of enabling identification of a found animal by any scanner-equipped shelter or veterinary practice. The national and international pet recovery databases that read standard ISO microchip frequencies are free to register with and do not require the annual subscription fees charged by proprietary registry services. Practices that present microchipping as a bundled package with mandatory service subscriptions are converting a welfare tool into a subscription product and the subscription component is never clinically necessary for the microchip to function. Registering a microchip with a free universal registry and declining proprietary service subscriptions provides equivalent practical recovery benefit at no ongoing cost.
Behavioral Medications

Recommending pharmaceutical behavioral intervention including anti-anxiety medications, antidepressants, and situational sedatives for pets presenting with normal stress responses to common triggers including veterinary visits, car travel, fireworks, and separation without first completing a structured behavioral modification protocol represents a clinical shortcut that benefits practice revenue more than animal welfare in many cases. Board-certified veterinary behaviorists, who represent the specialist standard for companion animal behavioral medicine, consistently place behavioral modification protocols as the primary intervention for most anxiety presentations with pharmacological support used as a complement to behavior work rather than a substitute for it. General practice vets who prescribe behavioral medications without a behavioral modification plan, a follow-up structure, or a referral pathway to behavioral expertise are managing a complex clinical domain with a tool that addresses symptoms rather than causes. The long-term use of behavioral medications in companion animals without concurrent behavioral work frequently produces animals who are pharmacologically managed but no less distressed in their underlying behavioral state. Pet owners presented with a behavioral medication recommendation at a general wellness visit are well served by asking specifically what behavioral modification protocol should accompany the medication and whether a referral to a veterinary behaviorist is appropriate.
Acupuncture Services
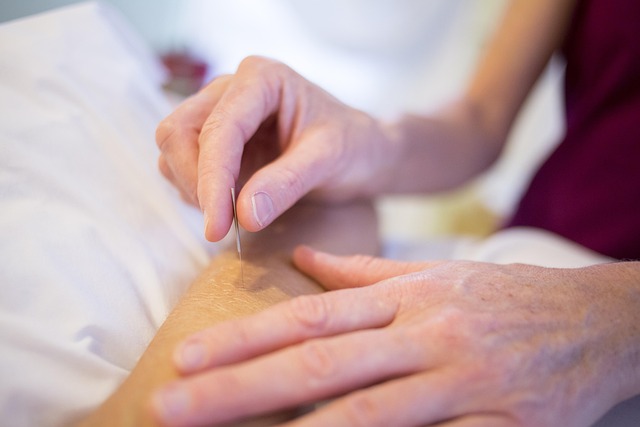
Veterinary acupuncture offered at general and specialty practices as an evidence-based therapeutic option for chronic pain, neurological conditions, and internal medicine cases is frequently presented with a confidence and clinical equivalence to conventional medicine that the current evidence base in veterinary species does not consistently support. The human acupuncture literature itself contains significant methodological controversy regarding placebo-controlled trial design and the challenges of blinding that apply with even greater force to veterinary research where patient reporting of subjective benefit is unavailable. The cost of veterinary acupuncture sessions is typically structured as a series of weekly or biweekly appointments each carrying a consultation fee that accumulates rapidly into a treatment investment comparable to or exceeding conventional therapeutic alternatives. Pet owners considering acupuncture for a companion animal are reasonably entitled to ask their veterinarian to specify which peer-reviewed veterinary studies support its use for their animal’s specific condition and to compare that evidence quality against the evidence supporting conventional alternatives. The recommendation of acupuncture alongside conventional medicine as an integrative option is defensible in specific contexts but its presentation as an equivalent or primary therapeutic option for conditions with established conventional treatments requires a higher evidentiary justification than it typically receives.
Genetic Testing

Breed-specific genetic testing panels marketed as essential tools for anticipating and preventing future health conditions in mixed-breed or purebred pets are frequently recommended at general wellness visits with an implied clinical utility that exceeds what the current state of veterinary genetic medicine can actually deliver for most conditions identified. The identification of a genetic variant associated with a condition does not in most cases change the clinical management of a currently healthy animal and the psychological burden of a positive result for a condition that may never manifest, or that would be managed identically whether identified genetically or clinically, can harm owner wellbeing without producing any benefit to the animal. Veterinary geneticists distinguish between genetic tests with actionable clinical consequences, such as MDR1 mutation testing in herding breeds before prescribing specific medications, and broad wellness panel testing whose results generate worry rather than management changes. The commercially available consumer-facing genetic panels marketed through veterinary practices frequently bundle genuinely actionable tests with a much larger number of variants whose clinical significance in the individual animal is speculative or negligible. Asking specifically which results from a proposed genetic panel would change the clinical management of your animal is the most useful filter for assessing whether a genetic testing recommendation serves your pet’s interests.
Orthopedic Supplements
Recommending therapeutic laser treatment, hydrotherapy, and rehabilitation physiotherapy packages as preventive wellness services for pets with no diagnosed musculoskeletal condition or documented functional deficit represents a wellness upsell category whose clinical justification requires individual assessment rather than general recommendation. These services have genuine and well-documented benefit for animals recovering from orthopedic surgery, managing degenerative joint disease, or rehabilitating from neurological injury and their value in those clinical contexts is not in question. The extension of these services into preventive wellness recommendations for healthy animals without specific risk factors or clinical signs introduces a cost burden on owners without a proportionate clinical rationale. Therapeutic laser in particular is a rapidly growing veterinary revenue category marketed with impressive-sounding technology while its evidence base for preventive use in healthy animals remains preliminary. Asking a practice to specify the clinical finding or documented risk factor that makes any rehabilitation or physical therapy service specifically indicated for your currently healthy animal is a reasonable and clinically defensible request.
Urinalysis Add-Ons
Routine urinalysis added to every wellness visit as a standard panel item regardless of the animal’s age, health history, clinical signs, or documented risk factors for urinary tract conditions is a low-cost-to-perform, moderate-cost-to-charge diagnostic add-on whose universal application generates consistent revenue while delivering clinical value primarily to the subset of animals with age-related or breed-specific urinary risk profiles. Veterinary internal medicine guidelines recommend urinalysis frequency based on individual patient risk assessment with senior animals, animals with known kidney disease, diabetes, or urinary history, and certain predisposed breeds representing the population where routine screening has clear clinical rationale. The universal application of urinalysis to every wellness visit for every patient regardless of individual risk profile is a revenue-driven standardization of a clinically individualized decision. The additional recommendation to send routine urinalysis for culture regardless of sediment findings, which increases cost significantly, requires specific sediment findings or clinical signs to justify rather than being applied as an automatic second step. Pet owners can ask their veterinarian to explain why their specific animal’s age, breed, and health history makes urinalysis indicated at this particular visit.
Prescription Parasite Medications

The recommendation of prescription-only parasite prevention products at significant price premiums over equivalent over-the-counter formulations containing the same or similar active ingredients at equivalent concentrations is a widespread practice whose financial benefit to the prescribing practice is embedded in the prescription infrastructure rather than in the clinical differentiation of the product. Several active ingredients including permethrin, pyrethrins, and certain isoxazolines are available in both prescription-required and over-the-counter formulations with different brand architectures but comparable efficacy profiles at equivalent doses. The parasiticide market is one of the highest-revenue product categories in companion animal medicine and the prescription channel creates a captive purchasing relationship that the over-the-counter market does not. Independent veterinary parasitology guidelines focus on matching the parasite prevention product to the animal’s specific geographic exposure risk and parasite species profile rather than on recommending proprietary prescription formulations universally across all patients. Pet owners who ask specifically which parasites are clinically relevant in their geographic area and their pet’s lifestyle and which active ingredients address those parasites most effectively are positioned to make an evidence-based product selection rather than a brand-driven one.
Imaging Packages

Recommending comprehensive radiographic or ultrasound imaging packages as routine wellness screening for apparently healthy adult animals without clinical signs, palpation findings, or age-related risk factors that would support diagnostic imaging represents a significant revenue opportunity dressed as preventive medicine. Radiology and ultrasound generate high per-procedure revenue and their recommendation in a wellness context leverages the owner’s desire for comprehensive information about their animal’s internal health without the requirement of a clinical finding to justify the investigation. Veterinary radiologists who provide independent interpretation services frequently note that incidental findings on wellness imaging in healthy animals generate a cascade of follow-up investigations and owner anxiety that produces more clinical activity than clinical benefit. The principle of diagnostic imaging in veterinary medicine, as in human medicine, is that imaging should follow clinical suspicion based on examination findings, history, or documented risk factors rather than precede it as a population-level screening tool in healthy patients. Asking specifically what clinical finding from today’s examination or what documented risk factor in your animal’s history is motivating an imaging recommendation is the appropriate response before consenting to any radiographic or ultrasound procedure.
Therapeutic Foods

Therapeutic food topper products, probiotic formulations, digestive enzyme supplements, and organ support nutraceuticals sold through veterinary practices as adjunctive wellness support for healthy animals represent a rapidly growing product category whose retail margins are high, whose regulatory oversight is minimal, and whose clinical evidence base for use in healthy animals without documented deficiencies or conditions is largely absent. The veterinary nutraceutical category operates in a regulatory environment that does not require proof of efficacy before sale, which means products can be marketed with compelling wellness language and presented with clinical authority in a veterinary setting without the evidentiary standard that pharmaceutical products must meet. Practices that sell these products directly generate retail revenue from every recommendation and the absence of a required diagnosis or clinical finding for their recommendation removes the primary friction that limits pharmaceutical upselling. Independent veterinary nutritionists consistently note that healthy animals eating a complete and balanced diet have no documented need for the majority of supplementary wellness products sold through veterinary channels. Requesting the specific clinical or nutritional finding that makes a recommended supplement necessary for your healthy animal, and asking whether a dietary adjustment would address the same concern, are productive responses to this category of recommendation.
Pain Management Protocols

Multimodal pain management protocols including combinations of NSAIDs, gabapentin, tramadol, and adjunctive analgesics recommended for routine low-complexity procedures such as spays, neuters, and dental cleanings in young healthy animals at doses and durations extending well beyond the expected tissue trauma and recovery window represent a prescribing pattern whose pharmaceutical cost to the owner significantly exceeds what minimally necessary analgesic coverage for the procedure would require. Veterinary anesthesia specialists support appropriate multimodal analgesia for all surgical procedures and perioperative pain management is a genuine welfare priority that should not be dismissed. The distinction between appropriate perioperative analgesia and extended multimodal protocols whose duration and complexity exceed the clinical demands of routine low-morbidity procedures is a legitimate clinical conversation that many general practice clients are never invited to have. Take-home pain medication packages for routine procedures can accumulate into a significant post-operative pharmaceutical cost that an honest clinical conversation about expected recovery trajectory might reduce without compromising animal welfare. Asking specifically how many days of post-operative pain medication clinical experience suggests is necessary for a specific procedure in a healthy young animal of your pet’s size is a reasonable question with a defensible clinical answer.
Stem Cell Therapy

Veterinary stem cell therapy marketed for osteoarthritis, tendon injury, and inflammatory conditions in companion animals is offered at some specialty and regenerative medicine practices at costs frequently exceeding two thousand dollars per treatment course and is presented with a clinical confidence that the current peer-reviewed veterinary evidence base does not uniformly support. Veterinary regenerative medicine is a genuinely developing field with legitimate scientific foundations and some promising early research, but the translation of early-phase research findings into clinical recommendations for individual patients at significant financial cost requires a transparency about evidence quality that many marketing materials and some clinical presentations omit. The regulatory environment for veterinary stem cell products is evolving and the consistency of cell preparation quality, viability, and dose standardization across providers varies in ways that affect clinical outcomes but are difficult for pet owners to assess independently. Requesting a specific review of peer-reviewed evidence supporting stem cell therapy for your animal’s specific condition, the expected magnitude and duration of benefit, and how outcomes are monitored and assessed after treatment are reasonable prerequisites before committing to this investment. Second opinions from board-certified veterinary specialists in the relevant clinical domain are particularly valuable before proceeding with any regenerative medicine recommendation.
Ophthalmology Screenings

Annual comprehensive ophthalmological screenings including tonometry, slit lamp examination, and electroretinography recommended for breeds with no documented elevated intraocular pressure, no family history of hereditary eye disease, and no clinical signs of visual disturbance represent a preventive screening category whose revenue benefit is embedded in the specialist referral and equipment cost structure rather than in demonstrated outcome improvement for the screened population. Veterinary ophthalmology screening has clear and well-supported clinical rationale for breeds with documented high prevalence of progressive retinal atrophy, hereditary cataracts, and glaucoma and for individual animals with clinical signs suggesting ocular pathology. The extension of annual specialist ophthalmology screening to the general pet population without specific clinical or breed-based risk factors converts a targeted diagnostic tool into a revenue-generating wellness service. Breed-specific eye disease prevalence data is publicly available through veterinary ophthalmology registries and provides the basis for an evidence-based assessment of whether annual specialist screening is genuinely indicated for any specific animal. Pet owners can assess whether their breed’s documented ophthalmological risk profile supports the screening frequency being recommended or whether a basic ocular assessment during routine wellness examination is sufficient for their animal’s actual risk level.
Microbiome Testing

Fecal microbiome testing marketed as a window into comprehensive gut health assessment for companion animals is an emerging diagnostic product category whose clinical utility for guiding treatment decisions in healthy animals is not established by the current veterinary gastroenterology evidence base. Human microbiome research has identified associations between microbial composition and various health outcomes but translating those population-level associations into actionable individual clinical decisions remains methodologically challenging even in human medicine and even more so in veterinary species where reference range databases are less developed. The recommendation of microbiome testing followed by probiotic or dietary modification based on the results creates a clinically plausible narrative that is commercially effective but frequently lacks a specific clinical finding that would change management independent of the test. Veterinary internal medicine specialists note that probiotic recommendations in companion animals are best guided by clinical diagnosis rather than by microbiome composition analysis whose interpretation lacks standardized clinical decision thresholds. Asking what specific management decision will be made differently based on the microbiome test result compared to empirical probiotic or dietary guidance is the most useful question before agreeing to this investigation.
Hormone Testing

Comprehensive hormone panels including thyroid, adrenal, reproductive, and metabolic hormone testing recommended for healthy middle-aged pets without clinical signs or physical examination findings suggestive of endocrine disease represent a screening application of endocrine diagnostics whose positive predictive value in asymptomatic animals is low and whose false positive rate generates costly and sometimes invasive follow-up investigation. Veterinary endocrinology guidelines support hormone testing when clinical signs including weight change, coat changes, polyuria, polydipsia, exercise intolerance, or behavioral change are present and document a clinical rationale for the investigation. The recommendation of comprehensive hormone screening as a routine wellness addition for clinically normal animals uses the diagnostic infrastructure of endocrinology to generate revenue without the clinical trigger that endocrine guidelines require before testing is initiated. The detection of a borderline hormone value in an asymptomatic animal frequently initiates a management and monitoring pathway whose cumulative cost over the animal’s life significantly exceeds the cost of a single screening panel. Asking whether your animal’s physical examination findings or clinical history provides a specific clinical rationale for endocrine testing is the appropriate first response to a routine hormone panel recommendation.
Rehabilitation Packages

Structured multi-session rehabilitation packages sold at the point of a post-surgical or injury discharge as prepaid treatment bundles require careful scrutiny because the prepayment structure commits the owner financially before the animal’s actual recovery trajectory and genuine rehabilitation needs have been established. Veterinary rehabilitation therapy has genuine clinical value for specific post-operative and neurological recovery scenarios and the discipline of companion animal physiotherapy is a legitimate and growing specialty. The commercial packaging of rehabilitation into prepaid session bundles whose total cost is agreed before outcomes are observed creates a financial structure that serves practice revenue predictability more than it serves the clinical flexibility of responding to how a specific animal’s recovery actually progresses. Animals recover from orthopedic and neurological events at highly variable rates and a rehabilitation plan that is clinically appropriate is one that is reassessed at each session rather than prescribed in full at discharge. Requesting a pay-per-session structure that allows rehabilitation intensity and duration to be calibrated to your animal’s actual recovery response rather than a prepaid bundle is a clinically reasonable request that any reputable rehabilitation practice should be able to accommodate.
Nutritional Counseling Fees

Standalone nutritional counseling consultation fees charged on top of wellness examination fees for dietary advice delivered during a routine visit without a documented nutritional disorder, weight problem, or specific medical condition requiring dietary management represent a fee-unbundling practice that converts advice historically included within the examination consultation into a separately billable service item. Nutritional assessment is a component of a comprehensive wellness examination and guidance about maintaining a healthy diet for a healthy animal is part of the clinical value the examination fee is intended to cover. The separation of nutritional discussion into a distinct billable service line with its own fee is a revenue expansion practice that is becoming more common in corporate veterinary settings where every clinical activity is evaluated for individual billing potential. Pet owners who receive a nutritional counseling fee on their invoice for a wellness visit during which basic dietary questions were addressed are in a reasonable position to request clarification of what specific nutritional service was delivered that was not part of the examination they were already paying for. Independent veterinary nutritionists who charge transparently for specialist nutritional consultation deliver a genuinely differentiated service that justifies a separate fee in a way that generalist dietary commentary during a routine wellness visit does not.
If any of these situations sound familiar from your own experience with veterinary care, share your thoughts in the comments.





