Many patients leave medical appointments feeling unheard or uncertain about their care, often without fully understanding why. Rushed consultations are more common than most people realize, and they can have real consequences for diagnosis accuracy, treatment adherence, and overall health outcomes. Recognizing the subtle behavioral cues that signal a hurried provider can help patients advocate more effectively for the thorough attention they deserve. The following signs are worth watching for during any clinical visit.
Eye Contact

A doctor who rarely looks up from their screen or notepad during a consultation may be prioritizing documentation over patient connection. Sustained eye contact is a foundational element of attentive clinical communication and plays a significant role in how well patients feel understood. Research in patient experience consistently links poor eye contact with lower satisfaction and reduced trust in the provider-patient relationship. When a physician’s gaze remains fixed on a computer monitor throughout most of the visit, it often reflects time pressure rather than indifference. This behavioral pattern is one of the earliest and most telling indicators that a consultation is being compressed.
Interruptions

Studies have found that physicians interrupt patients within seconds of them beginning to describe their symptoms, often before the full picture has been presented. Frequent interruptions prevent patients from sharing context that could be medically significant and redirect the conversation toward a predetermined diagnostic path. A doctor who regularly cuts off responses or steers away from elaboration may be operating under strict time constraints. This pattern can result in incomplete histories being recorded and potentially relevant complaints being overlooked entirely. Patients who notice repeated interruptions should consider asking explicitly for a few uninterrupted moments to finish describing their concerns.
Doorknob Questions

The term refers to the moment a patient raises an important new concern just as the physician is physically reaching for the door to exit. This scenario occurs with notable frequency and typically signals that the patient did not feel there was adequate time or space to raise all their concerns earlier in the visit. A doctor who responds to a doorknob question by glancing at a watch or subtly repositioning toward the exit may be signaling that time has already run out. Patients who find themselves saving concerns for the final seconds of an appointment often do so because the pace of the earlier conversation felt unwelcoming to additional questions. This dynamic is a meaningful indicator that appointment time was not structured around the patient’s full range of needs.
Prescription Speed

When a prescription is offered within the first few minutes of a consultation and before a thorough symptom discussion has taken place, it can suggest a pattern of formulaic care. Rapid prescribing is sometimes appropriate in straightforward or routine cases, but it becomes concerning when the patient has presented with complex or ambiguous complaints. A physician who reaches for the prescription pad before exploring lifestyle factors, medication history, or alternative explanations may be defaulting to efficiency over individualized assessment. Patients should feel comfortable asking what other options were considered before a treatment was selected. The speed at which a solution is offered can reveal how much deliberation was actually applied to the case.
Physical Examination

A perfunctory or abbreviated physical exam is one of the clearest signs that a visit is being condensed beyond clinical best practice. When a physician listens to the chest for only a few seconds, skips portions of a standard examination, or forgoes a hands-on assessment entirely, it limits the diagnostic information available for clinical decision-making. Physical examination remains a fundamental tool for detecting abnormalities that patients cannot self-report and that may not appear in initial test results. Patients who feel their physical assessment was cursory should not hesitate to ask whether a more thorough examination would be appropriate given their symptoms. The depth of a physical exam is often a reliable proxy for the overall quality of attention given during a visit.
Room Changes
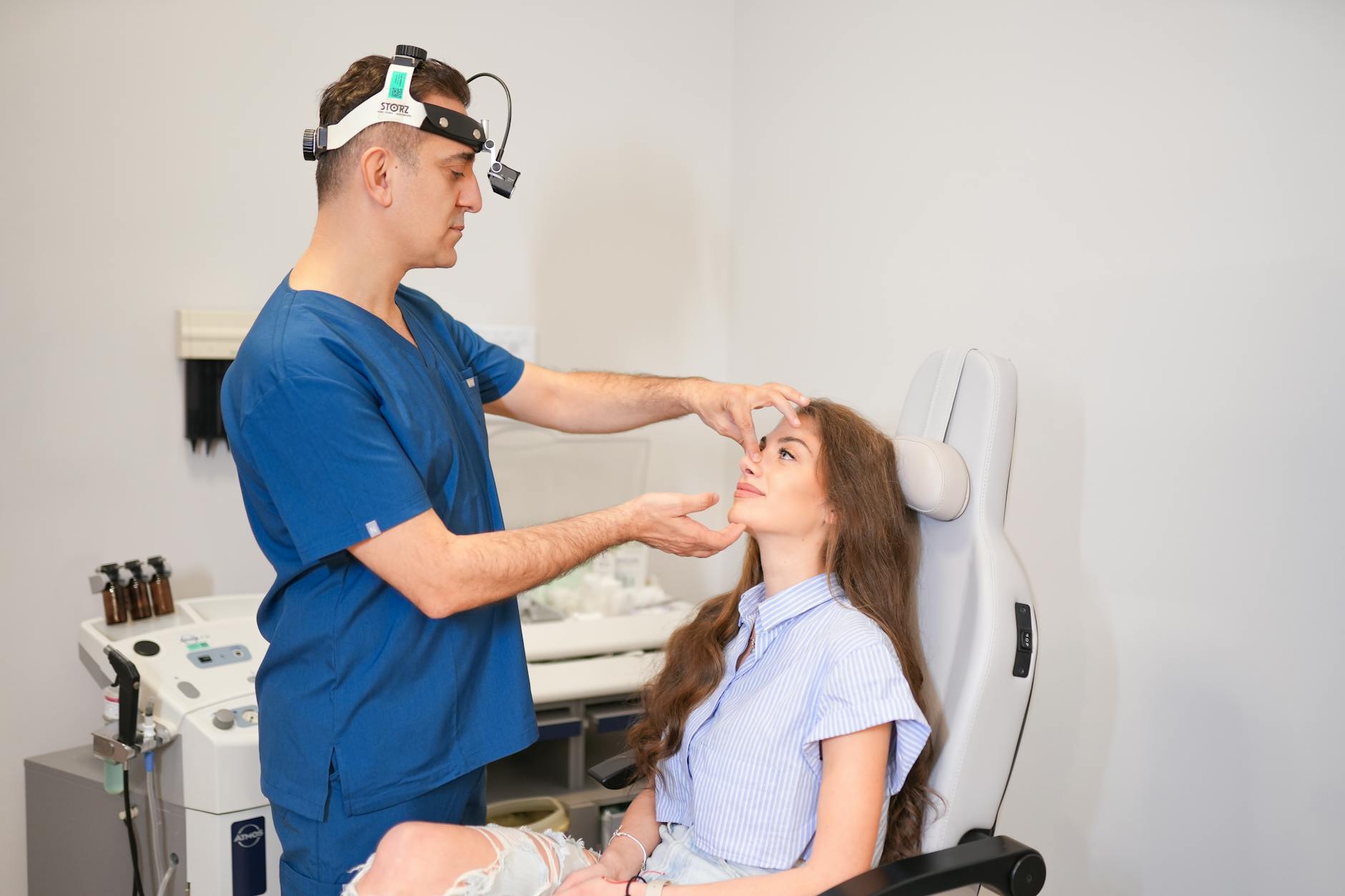
Being moved between rooms, nurses, or assistants multiple times before seeing the primary physician can reflect a clinic workflow designed around throughput rather than patient experience. Fragmented handoffs between staff members increase the risk that important context shared early in a visit will not be fully communicated to the treating doctor. When a physician arrives already summarizing information relayed by a nurse rather than gathering it directly, some nuance may have been lost in translation. Multiple room transitions also increase patient anxiety and reduce the sense of continuity that supports a productive consultation. This structural pattern is worth noting as a broader indicator of how time and attention are allocated across the clinic.
Dismissed Symptoms

When a patient mentions a symptom and it is quickly labeled as stress, aging, or a minor concern without further exploration, the consultation may have moved too fast to fully assess the complaint. Symptom dismissal does not always reflect poor clinical judgment but can be a consequence of time pressure that pushes physicians toward rapid categorization. Symptoms that seem minor in isolation can occasionally be early markers of conditions that benefit significantly from early intervention. Patients whose concerns are brushed aside without follow-up questions or basic investigation should feel empowered to ask what criteria would warrant further testing. A thorough clinician will typically acknowledge even ambiguous symptoms with at least a brief explanatory response.
Absent Follow-Up Plans

A consultation that ends without a clear follow-up plan, a timeline for results, or instructions for when to return can indicate that the physician did not have sufficient time to close the visit properly. Clear communication about next steps is a core element of safe and effective outpatient care. When patients leave without knowing when they will hear back about test results or what symptoms should prompt a return visit, they are left without the safety net that good clinical practice provides. This gap is especially concerning for patients managing chronic conditions or waiting on results with potentially significant implications. The absence of a documented or verbally confirmed follow-up plan is a practical sign that the appointment concluded under time pressure.
Minimal Questions
A physician who asks very few open-ended questions during a consultation may be working from a compressed diagnostic checklist rather than conducting a genuine clinical inquiry. Open-ended questioning is the mechanism through which physicians uncover symptom patterns, patient concerns, and contextual information that structured intake forms cannot fully capture. When every question asked has a yes or no answer and the patient is not invited to elaborate, the history being gathered is likely incomplete. Doctors operating under significant time constraints often unconsciously shift toward closed questioning as a means of controlling the pace of the appointment. Patients who want to volunteer more information should feel within their rights to add context even when a question technically allows for a brief response.
Typing During Conversation

A physician who types continuously while a patient speaks may be completing documentation in real time as a time-saving strategy, but this practice can significantly compromise attentive listening. The cognitive demands of simultaneous typing and active listening mean that some verbal content will inevitably receive less attention than it would in a more focused exchange. Patients often modulate what they share based on how engaged their doctor appears, and a physician facing a screen may unconsciously discourage the kind of detailed disclosure that supports accurate diagnosis. Electronic health record requirements have placed substantial documentation burdens on physicians, and real-time typing is a common response to that pressure. While the practice is not inherently problematic, its consistent use throughout a consultation warrants awareness.
Skipped Medical History

When a physician proceeds to discuss symptoms or recommend treatment without reviewing or referencing the patient’s existing medical history, it can indicate a visit that is already running behind schedule. Medical history provides critical context for interpreting current symptoms, identifying contraindications, and personalizing care recommendations. Patients who have previously disclosed allergies, prior conditions, or current medications and find these details absent from the current conversation should gently reintroduce them. A failure to engage with existing records does not always reflect negligence but is a recognized indicator that the clinical encounter is being conducted under time constraints. Comprehensive care depends on treating the full patient rather than only the presenting complaint.
Short Visit Duration

Most medical guidelines recommend minimum consultation durations for various types of appointments, and visits that fall significantly below those benchmarks are a straightforward indicator of compressed care. Patients can reasonably observe whether an appointment felt proportionate to the complexity of their concerns or whether it concluded before all topics were addressed. A very short visit for a complex or multi-symptom presentation is a practical signal worth noting. Duration alone does not determine quality, but when brevity is paired with other signs on this list, it reinforces a pattern of rushed care. Patients who consistently feel that appointment lengths are insufficient are well within their rights to request longer bookings when scheduling.
Redirected Concerns

A physician who consistently redirects patient concerns back to a narrow diagnostic focus may be managing appointment scope in response to time limitations. Redirection can take the form of steering conversation away from emotional or contextual factors, dismissing questions as outside the scope of the visit, or deferring every secondary concern to an entirely separate appointment. While clinical focus has its place in efficient medicine, persistent redirection prevents a holistic view of the patient’s health from forming. Patients who repeatedly find their questions deferred or minimized may benefit from requesting a dedicated appointment specifically structured for a comprehensive review. Effective clinical care requires that patients feel their full range of concerns can at least be acknowledged within a single visit.
Nonverbal Cues

Body language communicates urgency and discomfort even when spoken words remain professionally measured and calm. A physician who positions their body toward the door, stands rather than sits, avoids settling into the room, or checks a watch or phone during a consultation is communicating through their physical presence that time is limited. These nonverbal signals are processed by patients even when they are not consciously identified and contribute to the overall feeling that an appointment was unsatisfying. Medical communication training increasingly emphasizes the importance of deliberate seated positioning and open body language as tools for building patient trust and encouraging disclosure. When a doctor’s physical stance signals departure before the conversation has concluded, the quality of the remaining exchange is likely to suffer.
Referral Without Explanation

Being referred to a specialist without receiving a clear explanation of why the referral is being made or what the physician expects the specialist to assess can indicate a consultation that ran short on time for discussion. Patients benefit significantly from understanding the clinical reasoning behind a referral, as this helps them prepare for the next appointment and reinforces their confidence in the care pathway being recommended. A referral that is offered rapidly at the end of a visit with minimal accompanying context may reflect a physician managing time rather than communicating comprehensively. Patients who receive unexplained referrals should ask what specific concern the specialist will be addressing and how the findings will be communicated back to their primary provider. Clarity at the handoff point between providers is essential for continuity and safety.
Staff Tone

The demeanor of administrative and nursing staff is often a reliable early indicator of the overall pace and culture of a clinical environment. Rushed greetings, minimal eye contact from reception staff, hurried intake processes, or a general sense of urgency in the waiting area can signal that the entire clinic is operating under pressure that will carry through to the physician encounter. Front-of-house staff tend to reflect the workflow norms established by the clinic’s scheduling and operational practices. Patients who notice that every staff member they interact with before seeing the doctor appears harried or distracted may reasonably expect that the same pressure is affecting the physician. Environmental and interpersonal cues in the reception area provide a meaningful preview of what the consultation itself may feel like.
Test Without Talk
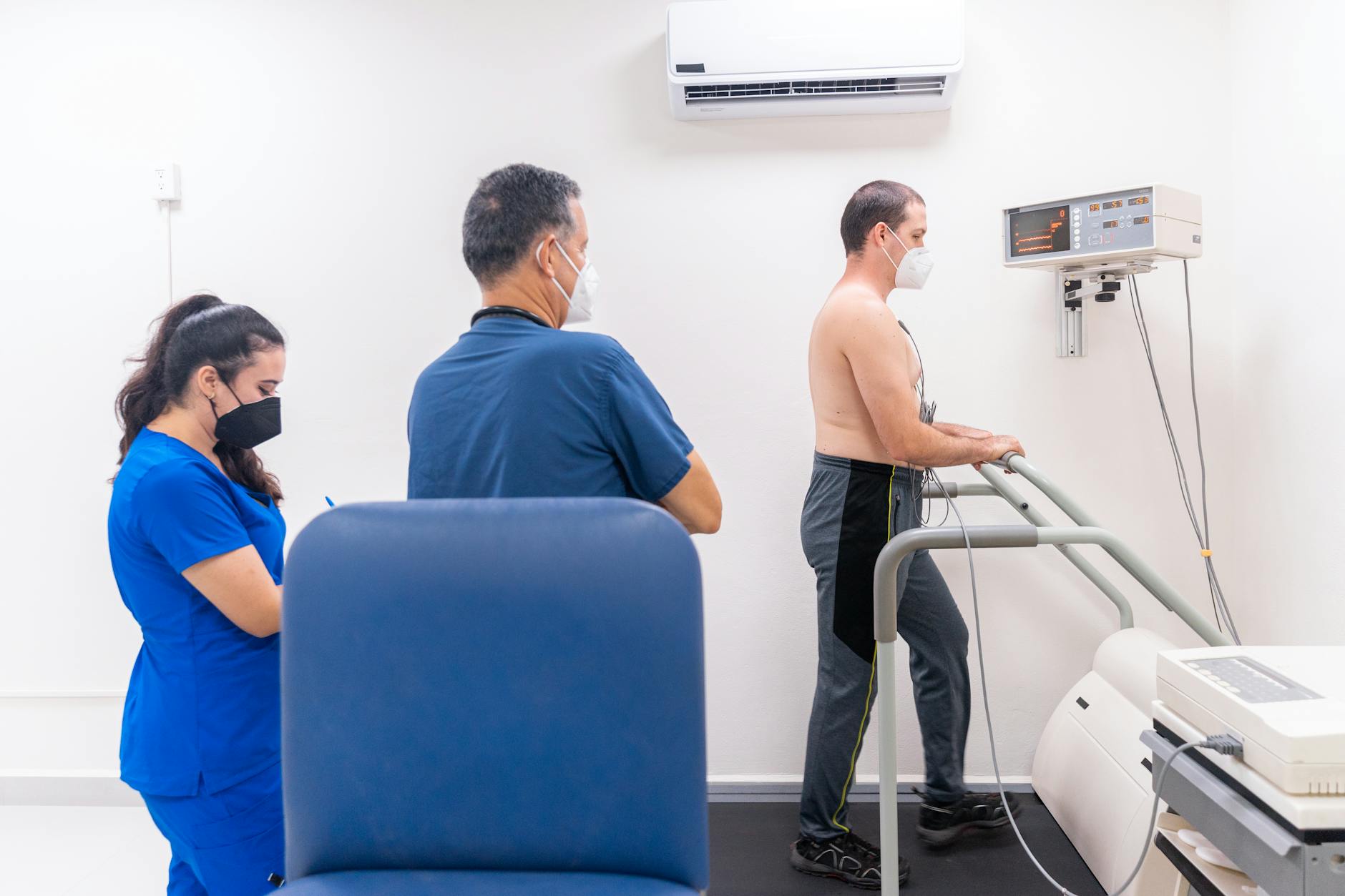
When a physician orders tests at the conclusion of a visit without discussing what the tests are looking for, what the results will mean, or how the patient will be notified, it can indicate that the appointment ended before clinical communication was complete. Test ordering accompanied by explanation is a best practice that supports informed consent and helps patients understand their role in the diagnostic process. Patients who receive a referral for blood work, imaging, or other investigations without understanding the clinical rationale should ask for a brief explanation before leaving the clinic. The absence of this conversation is not simply an inconvenience but can affect how patients interpret results and whether they follow through on the testing. A physician who consistently closes visits with unexplained test orders may be compressing the communication component of care in response to scheduling demands.
Have you experienced any of these signs during a medical appointment, and how did you handle it? Share your thoughts in the comments.