Every second counts when emergency responders arrive on scene, yet certain bystander and patient behaviors consistently slow down life-saving care. Paramedics train for years to manage chaos, trauma, and medical crises, but avoidable human obstacles can compromise outcomes in ways that are entirely preventable. Understanding what not to do during an emergency is just as important as knowing basic first aid. These are the most common behaviors that paramedics across the country repeatedly wish people would stop doing.
Crowding the Scene

When bystanders gather closely around an injured person, paramedics physically cannot access the patient efficiently. A tight crowd also limits airflow, raises stress for the injured person, and prevents equipment from being staged properly. Onlookers often believe they are helping simply by staying close, but the opposite is consistently true. Emergency crews need a clear working radius of several feet in every direction to function safely and effectively.
Filming Instead of Helping

Reaching for a phone to record an emergency scene delays any practical assistance a bystander could otherwise provide. Filming an injured or distressed person without their consent also raises serious ethical and legal concerns in many jurisdictions. Paramedics report that bystanders focused on capturing footage rarely respond to requests for help such as fetching an AED or directing traffic. Active emergencies require active assistance, not passive documentation.
Moving the Patient

Well-meaning bystanders frequently attempt to reposition someone who has collapsed or been injured before paramedics arrive. Moving a patient without proper training and assessment can worsen spinal injuries, displace fractures, and cause dangerous internal bleeding. The instinct to make an injured person more comfortable is understandable but can have serious medical consequences. Unless the person is in immediate danger from fire, water, or structural collapse, they should not be moved.
Withholding Medical History

When paramedics ask about medications, allergies, or pre-existing conditions, they need complete and immediate answers. Patients and family members sometimes omit information out of embarrassment or because they assume it is irrelevant to the current situation. A patient on blood thinners, for example, requires a fundamentally different treatment approach than one who is not. Every piece of health history shared on scene directly shapes the speed and accuracy of emergency care.
Calling Multiple Times

Placing repeated calls to emergency services for the same incident floods dispatch lines that other callers in crisis urgently need. Once a call has been made and acknowledged, additional calls from the same location do not speed up response times. In high-volume urban systems, duplicate calls can actually create confusion about the severity and nature of an incident. Trust that the first call has been received and that responders are already en route.
Giving Food or Water

Offering food or water to an injured or unwell person feels instinctively kind, but it can create serious complications. Patients who require emergency surgery must have empty stomachs to avoid aspiration during anaesthesia, and giving fluids can delay that window dangerously. Even a small sip of water given to someone with certain head or abdominal injuries can worsen their condition. Paramedics need patients to arrive at hospital in the same condition they left the scene.
Performing CPR Incorrectly
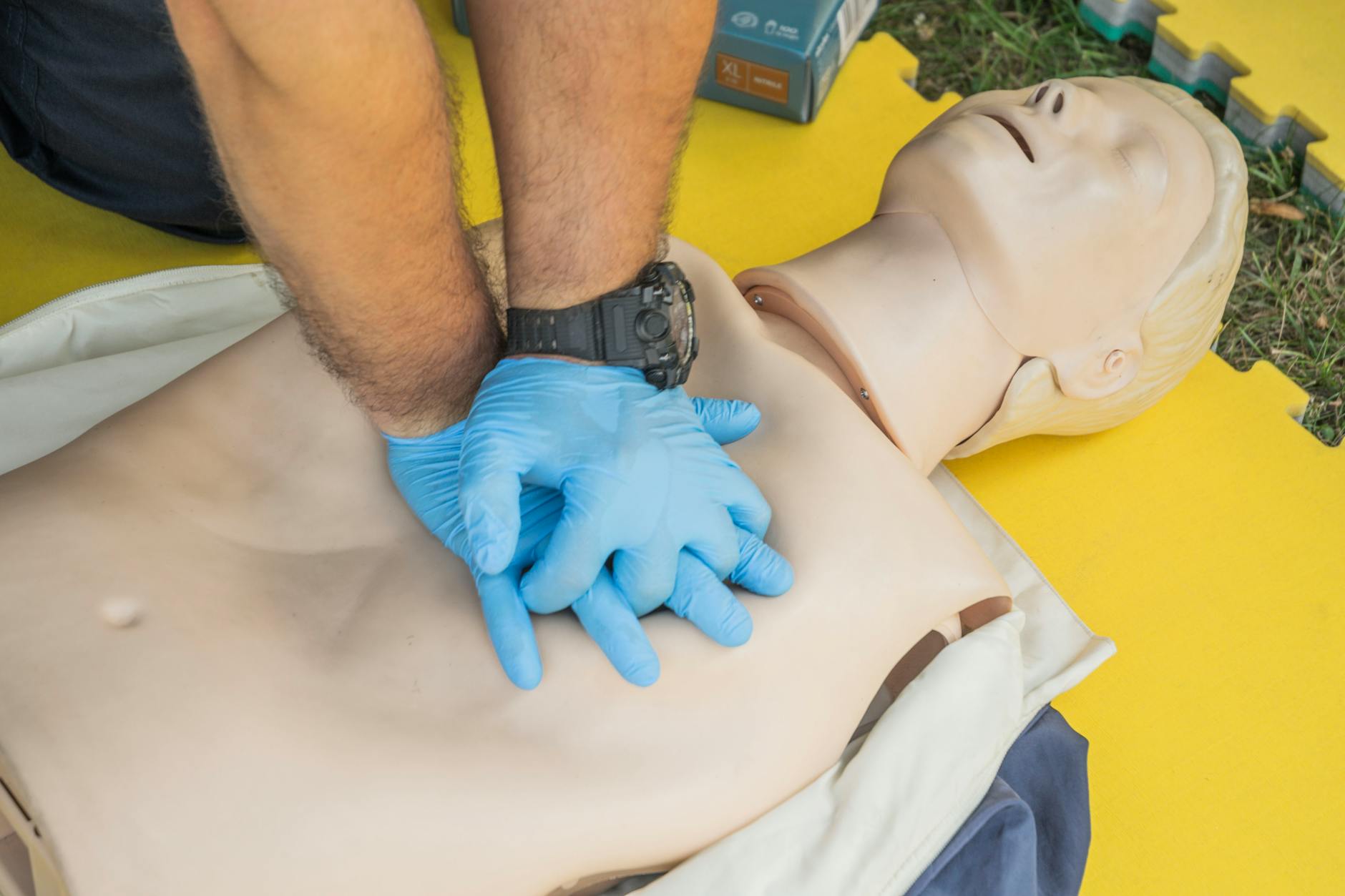
Bystander CPR saves lives, but only when performed at the correct depth, rate, and rhythm. Many people who attempt chest compressions do not push hard enough or fast enough to circulate blood effectively. Stopping compressions unnecessarily, even briefly, reduces survival rates in cardiac arrest patients. Those without formal CPR training are encouraged to follow dispatcher instructions in real time rather than relying on half-remembered technique.
Arguing With Responders

Paramedics make rapid clinical decisions under pressure and do not have time to negotiate or explain every action in detail on scene. Family members and bystanders who challenge treatment decisions or physically obstruct responders slow down care at the most critical moments. Questions about treatment are entirely valid but belong in the ambulance or hospital environment where there is more time and safety. Trusting the training of emergency professionals on scene is one of the most helpful things anyone can do.
Panicking Vocally

Loud crying, shouting, and expressions of panic in close proximity to a patient significantly raise that person’s stress and fear levels. Elevated stress responses can worsen certain cardiac events, breathing difficulties, and shock symptoms. Paramedics must also talk loudly over the noise to communicate with each other and with the patient. Those who cannot remain calm near the scene are strongly encouraged to step back and wait at a distance.
Administering Medication

Giving a patient medication without paramedic guidance, even a familiar over-the-counter product, can interfere with emergency treatment. Drug interactions, dosage issues, and contraindications are assessed by paramedics as part of their on-scene evaluation. Aspirin given to a stroke patient, for example, can make certain types of strokes significantly more dangerous. Only administer medication on scene if a dispatcher or clinician has explicitly instructed you to do so.
Blocking the Driveway

Ambulances and fire engines require unobstructed access to driveways, building entrances, and roadways to reach patients quickly. Vehicles parked across driveways or in narrow roads can add several critical minutes to a response time. In residential areas, neighbors are encouraged to move their cars proactively when they hear sirens approaching. The few seconds it takes to reposition a vehicle could be the most important action a bystander takes that day.
Lying About Symptoms

Patients and family members sometimes minimise or exaggerate symptoms, either out of fear of overreacting or because they want faster service. Paramedics depend on accurate symptom descriptions to triage correctly and prepare the appropriate equipment before arrival. Understating chest pain or difficulty breathing can mean a patient arrives undertreated with life-threatening consequences. Honest and precise descriptions of what is being experienced always produce the best outcomes.
Keeping Pets on Scene

Untethered or distressed animals near an emergency scene create unpredictable hazards for responders working quickly with sharp equipment and heavy gear. Dogs in particular may become defensive or aggressive when strangers handle their owner in ways that appear threatening. Paramedics have been bitten on scene often enough that the issue is treated as a genuine occupational safety concern. Pets should be moved to a closed room or secured outside immediately when responders enter a home.
Using a Tourniquet Incorrectly
Improvised tourniquets applied too loosely do not stop arterial bleeding and may actually increase blood loss. A tourniquet must be placed above the wound, tightened until bleeding stops, and the time of application noted clearly. Applying one to a joint, below a wound, or intermittently releasing it are all errors that worsen outcomes. Formal first aid training covers tourniquet use in detail and is one of the most valuable courses any adult can complete.
Directing Ambulances Incorrectly

Well-intentioned people sometimes wave down an ambulance and guide it in the wrong direction to save time, inadvertently causing delays. Dispatchers use GPS and real-time mapping to route responders efficiently, and overriding that guidance creates confusion. If you need to flag down a responder, make yourself visible with large arm movements from a stationary position rather than running alongside the vehicle. Clear street numbers or landmarks communicated to dispatch are the most reliable way to guide emergency services.
Leaving the Scene Abruptly

Witnesses who leave before providing information to responders can remove context that is critical to understanding what happened. In cases involving collapse, accidents, or suspected overdose, knowing the sequence of events helps paramedics make faster and more accurate assessments. If you were present when an incident began, staying nearby until you have spoken to a responder takes only a few minutes and can be enormously valuable. You do not need to stay for the entire response, just long enough to share what you observed.
Ignoring Dispatcher Instructions

When someone calls emergency services, the dispatcher provides real-time guidance that is specifically designed for the situation at hand. Many callers become distracted, emotional, or convinced they already know what to do and stop listening to these instructions. Dispatcher protocols are evidence-based and updated regularly to reflect best practices in pre-hospital care. Staying on the line and following every instruction precisely is one of the highest-value actions a caller can take.
Assuming the Person Is Drunk

People experiencing diabetic emergencies, strokes, seizures, or severe infections can appear intoxicated to untrained observers. Bystanders who dismiss someone as simply drunk often delay calling for help by many critical minutes. A person who is unresponsive, unable to speak clearly, or behaving erratically always warrants a call to emergency services regardless of the perceived cause. Paramedics are trained to differentiate between intoxication and medical emergencies and should always be the ones making that assessment.
Removing Embedded Objects

An object embedded in a wound, whether glass, metal, or other material, should never be removed before paramedics arrive. Embedded objects often act as plugs that reduce blood loss, and removing them can trigger sudden severe haemorrhage. The correct approach is to stabilise the object without moving it and keep the patient as still as possible. Paramedics and emergency surgeons are equipped to manage object removal in a controlled clinical environment.
Giving Conflicting Instructions

When multiple bystanders shout different instructions at a patient or at each other, the result is confusion that slows every action. Research on bystander response consistently shows that a single designated leader produces faster and more effective results than a crowd of competing voices. If you are confident in your first aid training, take a clear leadership role and ask others to assist with specific tasks. Coordination always outperforms chaos in an emergency environment.
Turning Off Lights

In home emergencies, bystanders sometimes turn off lights in an attempt to calm a patient or create a quieter atmosphere. Paramedics require strong consistent lighting to assess wounds, check pupils, read medication labels, and access veins for IV lines. Dark environments create risks of equipment being misplaced or procedural errors being made under pressure. Turning on every available light in the room before responders arrive is always the right choice.
Withholding Information About Substances

In cases involving drug or alcohol use, bystanders and family members frequently omit this information out of fear of legal consequences for themselves or the patient. Paramedics operate under strict confidentiality and are not law enforcement officers. Knowing exactly what substances were taken, in what quantity and at what time, allows for faster and more targeted treatment that can prevent death. No patient has ever received worse care because a bystander told the truth about substances on scene.
Starting Unnecessary Fires

In vehicle accidents and some home emergencies, bystanders have been known to light flares or other open flames in areas where fuel leaks are present or suspected. Paramedics arriving at a scene with an active fire risk must stop all medical care and address the hazard before returning to the patient. Any visible fluid pooling near a crashed vehicle should be treated as a potential fuel or chemical leak until responders confirm otherwise. Keeping ignition sources away from accident scenes is a basic but frequently overlooked safety principle.
Downplaying Pediatric Symptoms

Parents and caregivers frequently minimise symptoms in children to avoid alarming them or out of genuine uncertainty about severity. Children can deteriorate much faster than adults, and a symptom that appears mild can indicate a serious underlying condition in a young patient. Paramedics always prefer to assess a child and find nothing serious than to arrive late to a situation that has escalated. When in doubt, always call emergency services and describe exactly what you are observing without filtering.
Dressing Wounds Before Paramedics Arrive

Applying improvised bandages, tight fabric, or tape to wounds before paramedics arrive can obscure the extent of an injury and complicate proper assessment. Responders need to see wounds directly to evaluate depth, contamination, and bleeding rate. Applying direct pressure with a clean flat hand is the appropriate bystander response to most bleeding wounds. Elaborate dressings are best left to trained responders with sterile materials and clinical judgment.
Leaving Children Unattended

In household emergencies, older children are sometimes left without supervision while adults attend to the crisis, which can lead to additional incidents. A frightened child who wanders toward an emergency scene, attempts to help, or accesses hazardous materials creates a secondary emergency. Assigning a trusted adult specifically to manage children during an emergency keeps them safe and keeps the primary scene clear. Planning in advance for how children will be cared for during a home emergency is a step most families overlook entirely.
Emergency responders dedicate their lives to helping others in the most critical moments imaginable, and understanding how to support rather than hinder their work is a responsibility every person shares. If you have encountered a situation where bystander behavior affected an emergency response, share your experience in the comments.