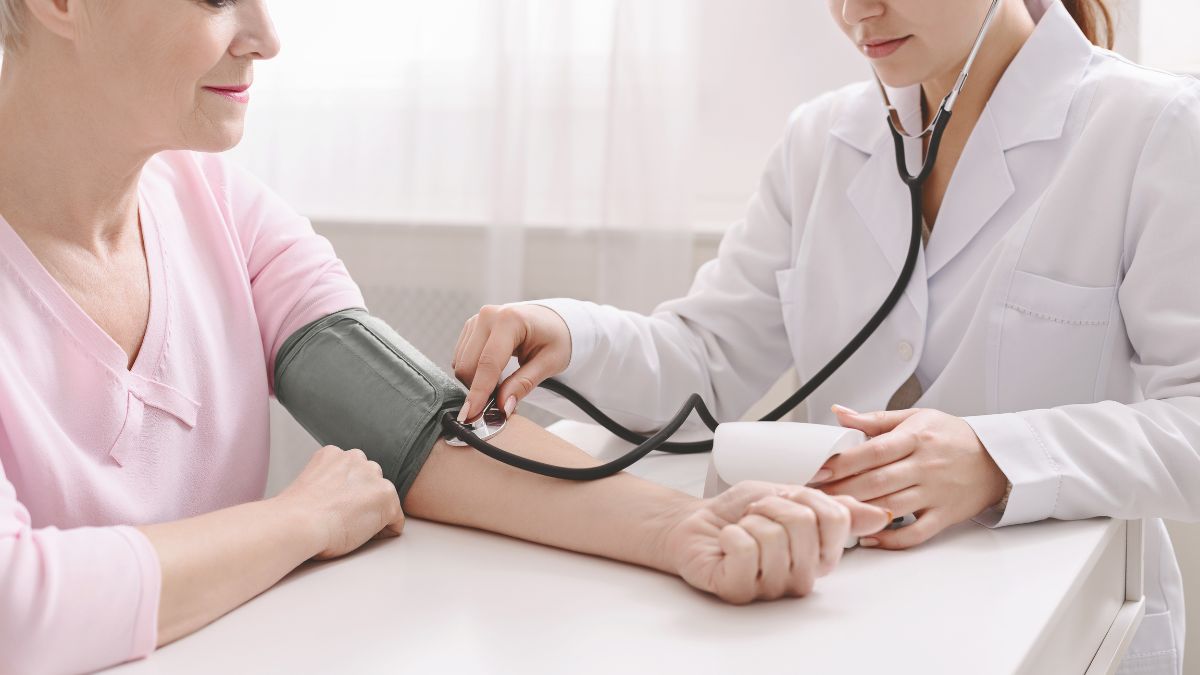
A blood pressure reading can be the difference between a clean bill of health and an unnecessary diagnosis, yet many people unknowingly sabotage their results before the cuff even goes on. Everyday habits in the hours leading up to a measurement can push numbers significantly higher than their true baseline. Medical professionals consistently flag a set of common pre-appointment behaviors that compromise accuracy and lead to misleading readings. Being aware of these habits and avoiding them gives patients a far clearer picture of their actual cardiovascular health.
Caffeine

Caffeine is one of the most well-documented culprits behind artificially elevated blood pressure readings. It works by stimulating the nervous system and temporarily causing blood vessels to constrict. Even moderate consumption from coffee, tea, or energy drinks can spike readings noticeably within thirty to sixty minutes. Most clinical guidelines recommend avoiding all caffeinated beverages for at least an hour before measurement. Patients who consume caffeine regularly are often surprised at how much their numbers improve once this habit is removed from the equation.
Smoking

Nicotine causes an immediate and measurable increase in blood pressure that can last up to thirty minutes after inhalation. The cardiovascular system responds to smoking by raising heart rate and tightening blood vessels at the same time. This effect is consistent whether the source is traditional cigarettes or electronic vaping devices. Clinicians advise patients to avoid smoking for a minimum of thirty minutes before any blood pressure appointment. A reading taken shortly after smoking reflects a stressed cardiovascular state rather than a resting baseline.
Alcohol

Alcohol has a complex relationship with blood pressure that many patients underestimate before appointments. While light consumption can temporarily lower pressure in the short term, moderate to heavy intake raises it significantly within hours. The body processes alcohol in ways that activate stress hormones and disrupt normal vascular function overnight. Arriving at a medical appointment after an evening of drinking can lead to readings that do not reflect true resting levels. Doctors recommend avoiding alcohol for at least twelve to twenty-four hours before a blood pressure test when possible.
Exercise

Physical activity raises heart rate and dilates blood vessels in ways that linger well beyond the workout itself. Even a brisk walk to the clinic can temporarily alter readings in ways that misrepresent a patient’s true baseline. The cardiovascular system needs adequate time to return to a genuine resting state after any form of exertion. Most medical guidelines recommend avoiding vigorous activity for at least thirty minutes before a reading is taken. Patients who exercise heavily in the morning should schedule their appointments with this recovery window clearly in mind.
Full Bladder

A distended bladder creates measurable physiological stress on the body that directly influences blood pressure readings. Studies have shown that readings taken when the bladder is full can be several points higher than those taken after urination. This effect is linked to the activation of the sympathetic nervous system in response to internal pressure. Patients are routinely advised to use the restroom before sitting down for any blood pressure measurement. This simple step takes under a minute and meaningfully improves the accuracy of the result.
Stress

Mental and emotional stress triggers the release of adrenaline and cortisol, both of which raise blood pressure rapidly. Rushing to an appointment, arguing before leaving the house, or arriving anxious about results can all distort a reading. The physiological response to psychological stress is nearly identical to the response to physical exertion in terms of cardiovascular impact. Sitting quietly for five minutes before the reading is taken is a standard clinical recommendation for this reason. Even brief moments of calm breathing have been shown to bring elevated stress-related readings noticeably closer to true resting levels.
Cold Temperatures

Exposure to cold causes blood vessels to constrict as the body works to preserve core temperature. This vasoconstriction directly raises blood pressure and can persist for several minutes after coming indoors. Patients who travel to appointments in cold weather should allow time to warm up before any measurement is taken. The effect is particularly pronounced in older adults and those with existing cardiovascular conditions. Sitting in a warm room for ten minutes is generally sufficient to allow the body to return to a more accurate baseline state.
Salt

High sodium intake in the hours or days before an appointment can cause the body to retain fluid and raise blood pressure measurably. A single salt-heavy meal has been shown to produce noticeable changes in vascular pressure within a relatively short window of time. Processed foods, fast food, and restaurant meals are common sources of sodium levels that most people do not account for. Patients who eat consciously in the day or two before a scheduled reading tend to produce numbers that more accurately reflect their typical state. Reducing sodium intake is one of the most straightforward ways to ensure a clean and representative result.
Certain Medications
A wide range of over-the-counter and prescription medications can interfere with blood pressure readings in ways patients rarely anticipate. Common decongestants found in cold and allergy products are among the most frequent offenders due to their vasoconstrictive properties. Nonsteroidal anti-inflammatory drugs and some herbal supplements can also raise pressure temporarily. Patients are encouraged to inform their doctor of everything they have taken in the previous twenty-four hours before a measurement is recorded. Timing medication use with medical guidance can prevent inaccurate readings that lead to unnecessary treatment adjustments.
Large Meals

Eating a substantial meal shortly before a blood pressure test can distort results in multiple directions depending on the individual. Digestion redirects blood flow and activates the autonomic nervous system in ways that temporarily shift cardiovascular function. High-fat and high-carbohydrate meals in particular have been associated with post-meal blood pressure fluctuations. The postprandial period, meaning the window directly after eating, is generally considered an unreliable time for accurate measurement. Patients are advised to wait at least one to two hours after a large meal before having their blood pressure formally assessed.
Crossed Legs

Sitting with crossed legs during a blood pressure measurement is a habit so common that many patients do not realize it affects results. This position restricts blood flow from the lower body back to the heart and measurably increases peripheral resistance. Studies have consistently found that crossing the legs at the knee during measurement can add several points to the systolic reading. Proper positioning with both feet flat on the floor and the back supported is considered essential for an accurate result. Healthcare providers are trained to correct this posture before taking a reading but patients can also self-monitor this habit.
Tight Clothing

Wearing tight sleeves or clothing that compresses the upper arm before or during measurement creates artificial pressure on the vasculature. The cuff requires direct skin contact and an unobstructed artery to produce a reliable reading. Clothing that must be rolled up tightly to expose the arm can itself restrict circulation in a way that skews results upward. Patients scheduled for blood pressure checks are advised to wear loose-fitting tops with short or easily accessible sleeves. This small wardrobe consideration eliminates one of the most easily preventable sources of measurement error.
Talking

Engaging in conversation while blood pressure is being measured is a widely overlooked source of inaccuracy. The physical act of speaking activates the respiratory and cardiovascular systems simultaneously and can raise readings by a meaningful margin. This effect is amplified during animated or emotionally charged conversations in the moments just before or during the test. Clinical guidelines consistently recommend that patients remain silent for at least one full minute before and during the measurement process. Healthcare providers are advised to complete the reading before resuming any discussion with the patient.
Poor Sitting Position

The way a patient is positioned during a blood pressure reading has a direct and well-documented effect on the accuracy of the result. Slouching or leaning forward places physical compression on the abdomen and alters the posture of the vascular system. The arm being measured should be supported at heart level and extended comfortably rather than held up or allowed to hang down. Sitting upright in a chair with back support is the medically recommended standard for any formal reading. Patients who are measured while perched on examination tables without back support or foot rests are often receiving readings that do not reflect their true resting state.
White Coat Syndrome

The anxiety that many people experience simply from being in a medical setting is a recognized clinical phenomenon with measurable effects on blood pressure. The anticipation of a potentially alarming result is enough to activate the body’s stress response and raise readings significantly. This response can occur even in patients who have perfectly normal blood pressure in everyday life. Clinicians often take multiple readings across an appointment or recommend home monitoring to distinguish true hypertension from situational anxiety. Recognizing and naming this phenomenon is the first step toward managing it and ensuring that treatment decisions are based on accurate data.
Digital Devices

Using a smartphone or tablet in the minutes before a blood pressure reading can elevate both heart rate and mental arousal through stimulating content and notification-driven stress. Screen time activates the cognitive system in ways that prevent the body from reaching a genuine resting state. Social media and news consumption in particular have been linked to short-term spikes in stress hormones that affect cardiovascular readings. Patients are encouraged to put down their devices and sit quietly for at least five minutes before a measurement is taken. This brief digital detox is one of the simplest and most overlooked adjustments a patient can make before any blood pressure appointment.
Energy Drinks

Energy drinks combine high doses of caffeine with sugar and other stimulants that amplify cardiovascular effects far beyond standard coffee consumption. The combined impact on heart rate and vascular tone can significantly distort blood pressure readings for several hours after consumption. Many patients do not consider energy drinks to be in the same category as coffee when preparing for a medical appointment. The stimulant compounds found in these products are processed more slowly by the body than standard caffeine alone. Avoiding energy drinks for a minimum of three to four hours before any blood pressure assessment is a widely supported clinical recommendation.
Napping

Waking from a daytime nap and proceeding directly to a blood pressure measurement produces readings that reflect a transitional physiological state rather than a true waking baseline. The body takes time to normalize circulation and autonomic function after sleep of any duration. Blood pressure behaves differently during sleep and continues to fluctuate in the immediate post-sleep window. Patients who nap before afternoon appointments should allow at least twenty to thirty minutes of quiet wakefulness before having their pressure checked. This transition period ensures that the reading reflects stable daytime function rather than the physiological blur between sleep and alertness.
NSAIDs
Nonsteroidal anti-inflammatory drugs including common products like ibuprofen and naproxen are among the most frequently overlooked contributors to elevated pre-reading blood pressure. These medications work in part by affecting prostaglandins that help regulate kidney function and sodium retention which in turn influences vascular pressure. Regular use or even a single dose taken before an appointment can shift readings upward in susceptible individuals. Patients managing chronic pain or inflammation with these products should inform their prescribing doctor about the timing of their use around blood pressure checks. Alternatives with lower cardiovascular impact may be recommended in cases where monitoring accuracy is particularly important.
Dehydration

Inadequate hydration causes blood volume to decrease which forces the cardiovascular system to work harder to maintain adequate circulation. This compensatory effort can produce readings that suggest elevated pressure even in individuals with no underlying hypertension. Many patients arrive at morning appointments in a mildly dehydrated state after hours of sleep without fluid intake. Drinking an appropriate amount of water in the hours before a reading supports accurate vascular function and measurement. Staying well hydrated is one of the foundational lifestyle habits that benefits not only blood pressure accuracy but long-term cardiovascular health overall.
Skipping Medication
Patients who take prescribed antihypertensive medications and skip a dose before an appointment often do so with the mistaken belief that it will reveal their true blood pressure. In practice this produces readings that reflect medication withdrawal rather than either a treated or untreated baseline. Abruptly missing doses of certain blood pressure medications can cause rebound hypertension that actually inflates readings well above typical levels. Healthcare providers rely on readings taken under consistent medication conditions to evaluate treatment effectiveness accurately. Patients should always take their prescribed medications on schedule unless a doctor has explicitly instructed otherwise for diagnostic purposes.
Loud Environments

Exposure to loud or chaotic environments in the period leading up to a blood pressure reading activates the auditory stress response and elevates physiological arousal. Noisy waiting rooms, loud music during transit, and stressful ambient environments all stimulate the nervous system in ways that affect cardiovascular function. Patients who travel to appointments through high-traffic or high-noise settings may arrive with temporarily elevated readings that do not reflect their resting state. Seeking a quiet corner in the waiting area and sitting calmly for several minutes helps the body transition toward a more accurate measurement baseline. Noise pollution as a factor in blood pressure measurement accuracy is increasingly being studied and acknowledged in clinical literature.
Grapefruit

Grapefruit and grapefruit juice contain compounds that interfere with enzymes responsible for metabolizing a wide range of medications including many commonly prescribed antihypertensives. When these enzymes are inhibited the concentration of medication in the bloodstream can rise unpredictably leading to blood pressure that is either lower or more volatile than expected. This interaction is not limited to a specific medication class and affects calcium channel blockers as well as other cardiovascular drugs. Patients on blood pressure medication who consume grapefruit regularly may be producing readings that reflect pharmacological interference rather than true treatment response. Discussing grapefruit consumption with a prescribing physician is particularly important for anyone undergoing active blood pressure management.
Licorice

Licorice root and products made with real licorice contain glycyrrhizin, a compound that mimics the hormonal activity of aldosterone and causes the body to retain sodium and excrete potassium. This hormonal mimicry directly elevates blood pressure in ways that can persist for days after consumption. Many patients are unaware that certain herbal teas, candies, and supplements contain real licorice root in meaningful amounts. The effect is dose-dependent and builds over time meaning regular consumption creates a more sustained elevation than a single serving. Patients with hypertension or those undergoing blood pressure monitoring are consistently advised to avoid licorice-containing products around and between medical appointments.
Wrist Cuffs

Wrist blood pressure monitors are widely available for home use but are inherently less accurate than upper arm cuffs when used without strict positional control. The radial artery measured at the wrist is more sensitive to positioning and movement than the brachial artery used in clinical upper arm measurements. Readings taken with the wrist below or above heart level can deviate significantly from true values. Patients who rely on wrist-based home monitors without following precise positioning protocols frequently bring skewed data to clinical appointments. Upper arm monitors calibrated against clinical equipment remain the gold standard for accurate blood pressure self-monitoring.
If any of these habits sound familiar, share which ones surprised you most in the comments.