Most people treat the medicine cabinet as a permanent storage solution, but many common household items actually degrade, lose effectiveness, or even become hazardous over time. Knowing what to remove and why can protect your health in meaningful ways. A regular audit of this often-overlooked space is one of the simplest habits a health-conscious household can adopt. The items listed here are the most critical to address, starting with the least urgent and ending with those that demand immediate attention.
Hydrogen Peroxide

Hydrogen peroxide breaks down into plain water surprisingly quickly once the bottle has been opened. Most opened bottles lose their antiseptic properties within one to six months, making them essentially useless for wound care. Storing it in a warm or light-exposed cabinet accelerates this breakdown even further. Unopened bottles typically carry a shelf life of around three years but should always be tested before use.
Cotton Balls

Cotton balls seem harmless to store indefinitely, but they can absorb moisture and harbor bacterial growth over long periods. Once exposed to a humid bathroom environment, their sterility is no longer guaranteed. Using contaminated cotton near open wounds or eyes creates an unnecessary infection risk. Sealed storage helps but does not fully protect them from prolonged humidity exposure.
Rubbing Alcohol

Rubbing alcohol evaporates steadily through its container, gradually reducing its concentration below the effective antimicrobial threshold. A bottle that has been open for more than a year may no longer contain enough active ingredient to properly sanitize surfaces or skin. The standard effective concentration is between 70 and 90 percent, which drifts downward with time and exposure. Replacing it annually is a straightforward and inexpensive precaution.
Calamine Lotion

Calamine lotion can separate, thicken, or develop an inconsistent texture as it ages beyond its expiration date. Its active ingredients become less effective at soothing itching or irritation once the formula destabilizes. Expired lotion applied to irritated skin can sometimes cause unexpected reactions in sensitive individuals. Checking the expiration date on topical treatments is just as important as doing so for oral medications.
Petroleum Jelly

Petroleum jelly has an impressively long shelf life but is not immune to contamination from repeated finger contact. Each time unwashed hands dip into the jar they introduce bacteria into the product. Over time this can transform a protective skin barrier product into a source of irritation or infection. Using a clean applicator and replacing open jars annually reduces this risk significantly.
Sunscreen

Sunscreen formulas are required by regulators to maintain their stated SPF for three years from the date of manufacture. Beyond that point the active UV-filtering compounds break down and leave skin far less protected than the label suggests. Heat and humidity inside a bathroom accelerate this degradation considerably. Keeping sunscreen in a cool dry location and replacing it each season ensures reliable protection.
Adhesive Bandages

The adhesive on bandages weakens noticeably with age and humidity exposure, causing them to peel away from skin before a wound has properly closed. The sterile pad inside the packaging can also lose its sterility if the seal has been compromised. A bandage that does not stay in place offers almost no meaningful protection against contamination. Rotating stock and replacing old boxes each year is a minimal investment for reliable wound care.
Antibiotic Ointment
Antibiotic ointments such as those containing neomycin or bacitracin can degrade chemically over time, reducing their effectiveness against infection. An expired product applied to a wound may give false reassurance while providing little actual antimicrobial benefit. In some cases degraded antibiotic compounds have been associated with increased skin sensitivity. Single-use packets are a practical alternative that eliminate the issue of long-term storage entirely.
Nasal Spray

Preserved nasal sprays have a defined period of effectiveness after first use, typically ranging from three to six months depending on the formulation. Preservative-free versions are even more time-sensitive and can become contaminated with repeated use. Using a nasal spray past its recommended window can introduce bacteria directly into the nasal passage. Noting the date of first use on the bottle is a simple habit that prevents this oversight.
Eye Drops

Eye drops are among the most contamination-prone products in any medicine cabinet due to direct contact with a highly sensitive mucous membrane. Most formulations carry a recommended discard period of 28 days after opening, regardless of remaining volume. Using expired or improperly stored eye drops risks introducing pathogens directly to the eye’s surface. Even products in sealed single-dose vials should be checked for expiration before use.
Thermometers
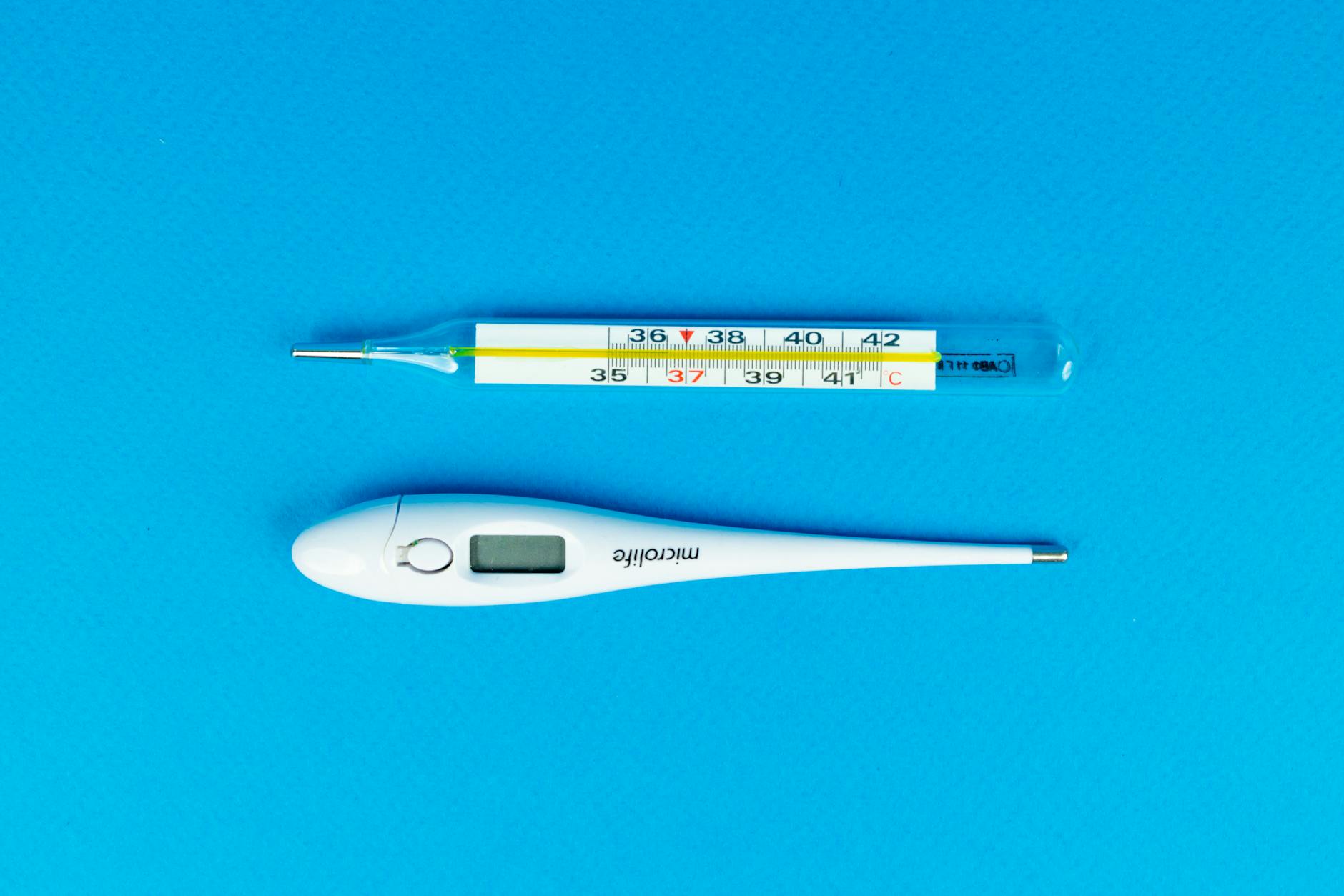
Older glass thermometers that contain mercury are classified as hazardous waste in many regions and pose a significant contamination risk if broken. Mercury vapor is toxic even in small quantities and is particularly dangerous in enclosed spaces. Many municipalities have banned their sale and offer collection programs for safe disposal. Digital alternatives are accurate and eliminate any risk associated with mercury exposure entirely.
Children’s Medication

Children’s medications are frequently reformulated and re-dosed as pediatric guidance evolves, making older products potentially inappropriate for current use. Liquid formulations degrade faster than adult tablets and may develop bacterial growth if left opened for extended periods. Dosing recommendations tied to weight and age can shift significantly within just a few years. Pediatric medications should be reviewed by a pharmacist or physician before use if they have been stored for more than one year.
Vitamins and Supplements
Fat-soluble vitamins such as A, D, E, and K are particularly vulnerable to oxidation and can produce harmful compounds as they break down past expiration. Water-soluble vitamins lose potency more gradually but still decline measurably after their recommended date. Many supplements also contain fillers and binders that can degrade and affect absorption over time. Storing them in a cool dry cupboard away from the bathroom extends their shelf life considerably.
Cough Syrup

Liquid cough and cold preparations have a shorter effective life than most solid oral medications due to their water-based formulations. Microbial growth can occur in opened bottles over time, particularly those stored in warm conditions. Active ingredients such as dextromethorphan and guaifenesin lose measurable potency after expiration. Opened bottles should generally be discarded after one cold and flu season.
Insulin
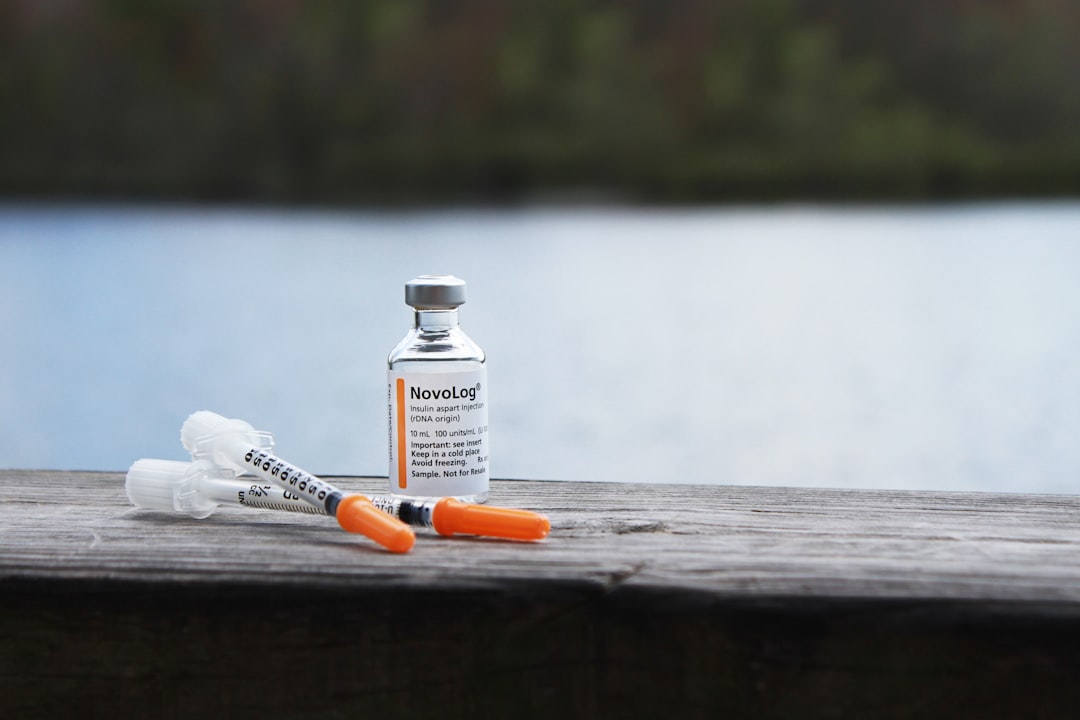
Insulin is a temperature-sensitive biological product that degrades rapidly when exposed to heat, freezing temperatures, or direct sunlight. Unopened insulin stored correctly in a refrigerator typically remains stable until the printed expiration date. Once opened and kept at room temperature, most formulations should be discarded after 28 to 30 days. Using degraded insulin can result in unpredictable blood sugar management, making proper storage genuinely life-critical.
Epinephrine Auto-Injectors
Epinephrine auto-injectors are among the most important emergency medications a household can keep on hand, but they are also highly time-sensitive. The solution degrades with exposure to light and temperature fluctuations, turning yellow or brown when it has deteriorated. An expired or discolored device may fail to deliver an effective dose during an anaphylactic emergency. These devices should be checked at every prescription renewal and replaced before expiration without exception.
Prescription Antidepressants

Storing unused or discontinued prescription antidepressants long-term creates a significant safety risk, particularly in households with children or vulnerable individuals. These medications should never be self-administered outside of a current prescription and should not be shared under any circumstances. Most pharmacies and many hospitals participate in take-back programs designed specifically for the safe disposal of controlled and sensitive medications. Retaining them beyond the prescribed course offers no health benefit and introduces meaningful risk.
Testosterone and Hormone Therapies

Hormone-based medications degrade in potency over time and can produce inconsistent physiological effects when used past their expiration date. Topical hormone preparations are especially vulnerable to contamination and compositional changes with prolonged storage. Residual products in shared spaces also create a risk of accidental exposure for other household members. These medications require careful disposal through a pharmacist-supervised take-back program.
Prescription Painkillers

Prescription opioid painkillers represent one of the most serious long-term storage risks in any home environment. Their presence beyond the treatment period increases the likelihood of misuse, diversion, and accidental ingestion by children. Chemical degradation over time does not make expired opioids safe, but it does make their dosage unpredictable. Drug take-back programs exist in most communities and provide a legal and environmentally responsible disposal route.
Old Prescription Antibiotics
Storing leftover antibiotics encourages inappropriate self-medication, which contributes to the broader global crisis of antimicrobial resistance. Some antibiotic classes, most notably tetracyclines, are known to develop harmful breakdown compounds after expiration that can damage the kidneys. Even antibiotics that do not produce toxic degradation products lose enough efficacy to be medically unreliable. Completing a prescribed course in full and disposing of any remainder promptly is the medically recommended approach.
Benzodiazepines

Benzodiazepines are controlled substances that carry a high potential for dependence and misuse, making long-term unsupervised storage particularly dangerous. Unused prescriptions kept in accessible locations create risk for other household members and guests. These medications interact with alcohol and numerous other drugs in ways that can be life-threatening. Safe disposal through an authorized take-back program is strongly advised as soon as a prescription course is complete.
Liquid Medications Near Expiry

Liquid medications of any class degrade faster than their solid counterparts and often provide no visible indication that they have become less effective or unsafe. The combination of water, active pharmaceutical ingredients, and preservatives creates a chemically unstable environment over time. Once opened, most liquid medications should be treated as having a significantly shorter usable life than the printed expiration date suggests. Writing the date of first opening on the label is a practical method for tracking this accurately.
Sleep Aids
Over-the-counter sleep aids typically rely on antihistamines such as diphenhydramine, which lose efficacy with both age and regular use due to tolerance development. Storing them long-term can normalize their use in ways that mask underlying sleep disorders requiring professional attention. Expired antihistamine formulations may also cause unexpected or heightened side effects including confusion and dry mouth. A healthcare provider should be consulted for any sleep difficulty that persists beyond several weeks.
Expired Contraceptives
Hormonal contraceptives of any format lose documented reliability past their expiration date as active hormone compounds degrade. Barrier methods such as condoms are equally affected, with latex and spermicidal coatings breaking down in ways invisible to the naked eye. Storing them in a warm environment such as a bathroom cabinet accelerates this degradation significantly. Replacing contraceptives before expiration is a straightforward step with consequences that are serious enough to warrant consistent attention.
Aspirin

Aspirin is the most universally underestimated item on this list precisely because it appears in virtually every medicine cabinet as a permanent fixture. It breaks down into acetic acid and salicylic acid over time, producing a distinctive vinegar-like odor that signals significant degradation. An expired aspirin used during a suspected cardiac event may fail to deliver the antiplatelet effect that makes it medically critical in that context. Given its low cost and its potential role in life-threatening situations, replacing aspirin well before expiration is one of the highest-value habits a household can adopt.
Take a moment to audit your medicine cabinet today and share what surprised you most about what you found in the comments.





